Simulation Program
The University of Maryland’s Anesthesiology Simulation Program encompasses all anesthesia delivery and teaching areas within the institution. University of Maryland School of Medicine Department of Anesthesiology has integrated simulation into its education and training program for medical students, residents, fellows, CRNAs, allied health professionals and faculty to develop and enhance their anesthesia and related cognitive, clinical, and team skills. Training is conducted primarily in the Maryland Advanced Simulation Training Research and Innovation Center (MASTRI).
Simulation Faculty
Program Director: Ross Carpenter, MD
Program Director: Robert Noorani, MD
Program Director: Matthew Tulis, MD
Facilities and Equipment
The Anesthesiology Simulation Program utilizes many resources from Maryland Advanced Simulation Training and Research Innovation Center (MASTRI), Shock Trauma Center (STC), UM Nursing, UM OB/Gyn and other centers and resources as needed. MASTRI is located on a 3600 square foot B wing of the south hospital at the University of Maryland Medical Center. It consists of four converted operating rooms which now serve as clinical staging areas (OR, ICU, PACU, ER). The broad range of human patient simulation modalities provides not only flexibility in scenario development, but also allows for concurrent training sessions to include more participants during a single time period.
Click here to visit the MASTRI Center website
There are two conference areas for teaching and debriefing and facilities for simulation preparation. Embedded audio/visual capabilities for live viewing, recording and playback ability are available in all spaces.
Additional technology includes:
- Virtual reality simulators
- Sim man and various patient simulators
- Partial task trainers
Undergraduate Education
A key function of the Anesthesiology Simulation program is to help medical students enhance their airway skills and learn peripheral, arterial and central line placement. The Anesthesiology faculty, fellow and residents are actively involved with medical students throughout the school year by leading airway workshops designed to teach students airway techniques as well as how to assess patients prior to intubation.
Medical students rotating on the anesthesiology subspecialty rotation attend an airway workshop in the simulation center. During this workshop, students learn how about mask ventilation, oral/nasal airways, laryngeal mask airways and direct/indirect laryngoscopy. The medical students rotating in trauma attend a scenario based simulation session run by the trauma anesthesiology faculty.
Medical students rotating on the anesthesiology elective attend an additional session in the simulation center. This session focuses on line placement. Each student is given an opportunity to practice peripheral, arterial and central line placement.
Graduate Medical Education
We specialize in simulation and task training to meet provider needs:
- Airway Management
- Crisis Resource Management
- Communication/Team Training
- Interdepartmental training scenarios
Residency Training
Task Training Sessions: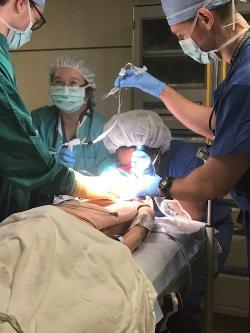
- Introduction to Simulation
- Anesthesia Information System (Metavision) Charting
- Airway I: difficult airway techniques: cricothyroidotomy, fiberoptic bronchoscopy, VR bronchoscopy
- Airway II: difficult airway techniques: retrograde wires, Fastrach LMA, Aintree Intubation Catheter
- Airway III: difficult airway techniques: supraglottic techniques, chest tubes, double lumen exchange
- Arterial line placement; FloTrac technology; Placement and interpretation of pulmonary artery catheters
- Central Line Insertion: sterile technique, identification of landmarks, ultrasound guidance
- Difficult Airway Management & ASA Algorithm
- Interosseus access (IO), lumbar drains and IVC catheter management
- Pediatric Anesthesia Techniques: intravenous access, IO access, caudal blocks
- Point of Care Ultrasound (POCS): transthoracic ECHO, FAST exam, Pulmonary exam
- OB skills: fetal monitoring, blood patches, combined spinal/epidural
Our philosophy at the Maryland Anesthesiology Program in Simulation (MAPS) involves the concept that “anesthesiologists do not function in a vacuum”. In our daily activities, we work with a myriad of professionals both in the operating room, intensive care units and throughout the hospital requiring us to develop our ability to be leaders of diverse multidisciplinary teams. An important quality of an anesthesiologist is that they not only master knowledge and procedural skills but be exceptional “team players”, assuming a preeminent role in the prevention and treatment of perioperative problems and the effective management of the clinical team to coordinate patient care activities. The nontechnical skills such as communication, leadership, situational awareness, decision making, prioritizing and utilizing resources are critical to an anesthesiologist’s professional development. We utilize high-fidelity critical situation simulations to create an atmosphere to nurture the growth of the individual clinician anesthesiologist in our residents while encouraging the growth of multidisciplinary team behaviors through reality-based clinical experiences with immediate constructive feedback but without incurring patient risk.