UM Medicine Faculty-Scientists and Clinicians Perform Second Historic Transplant of Pig Heart into Patient with End-Stage Cardiovascular Disease
September 22, 2023 | Deborah Kotz
After world’s first successful transplant in 2022, also performed at the University of Maryland Medical Center (UMMC), this groundbreaking transplant team performed second pig heart transplant on patient deemed ineligible for traditional heart transplant.
Resources for the Media:
Photos, Surgery Video, Patient & Surgeon Interviews.
Please download video and images to your computer before viewing them.
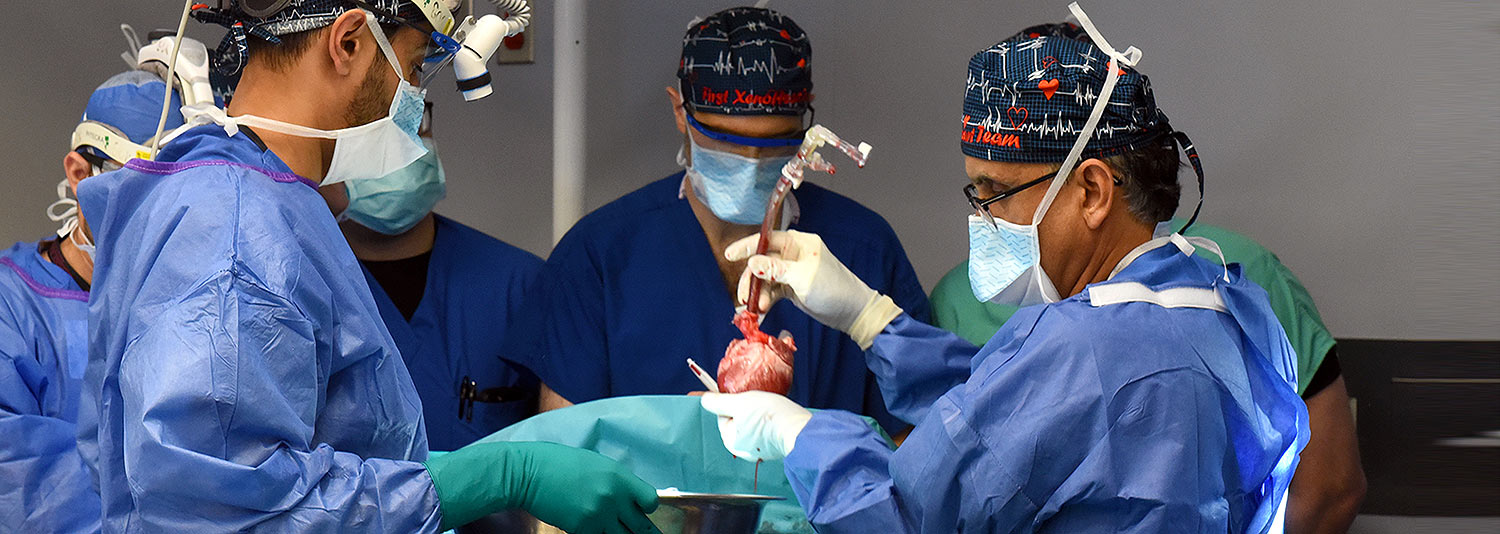
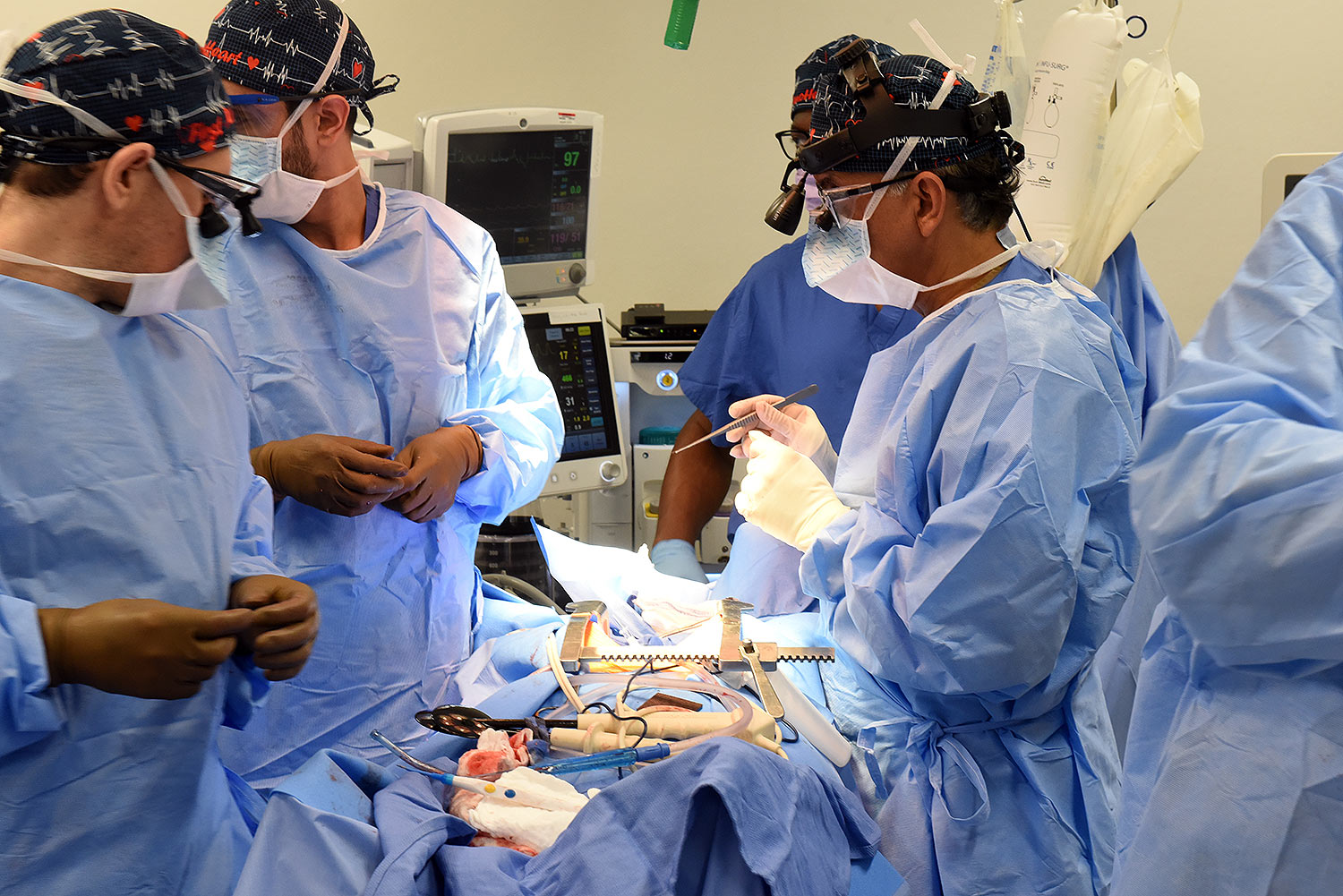
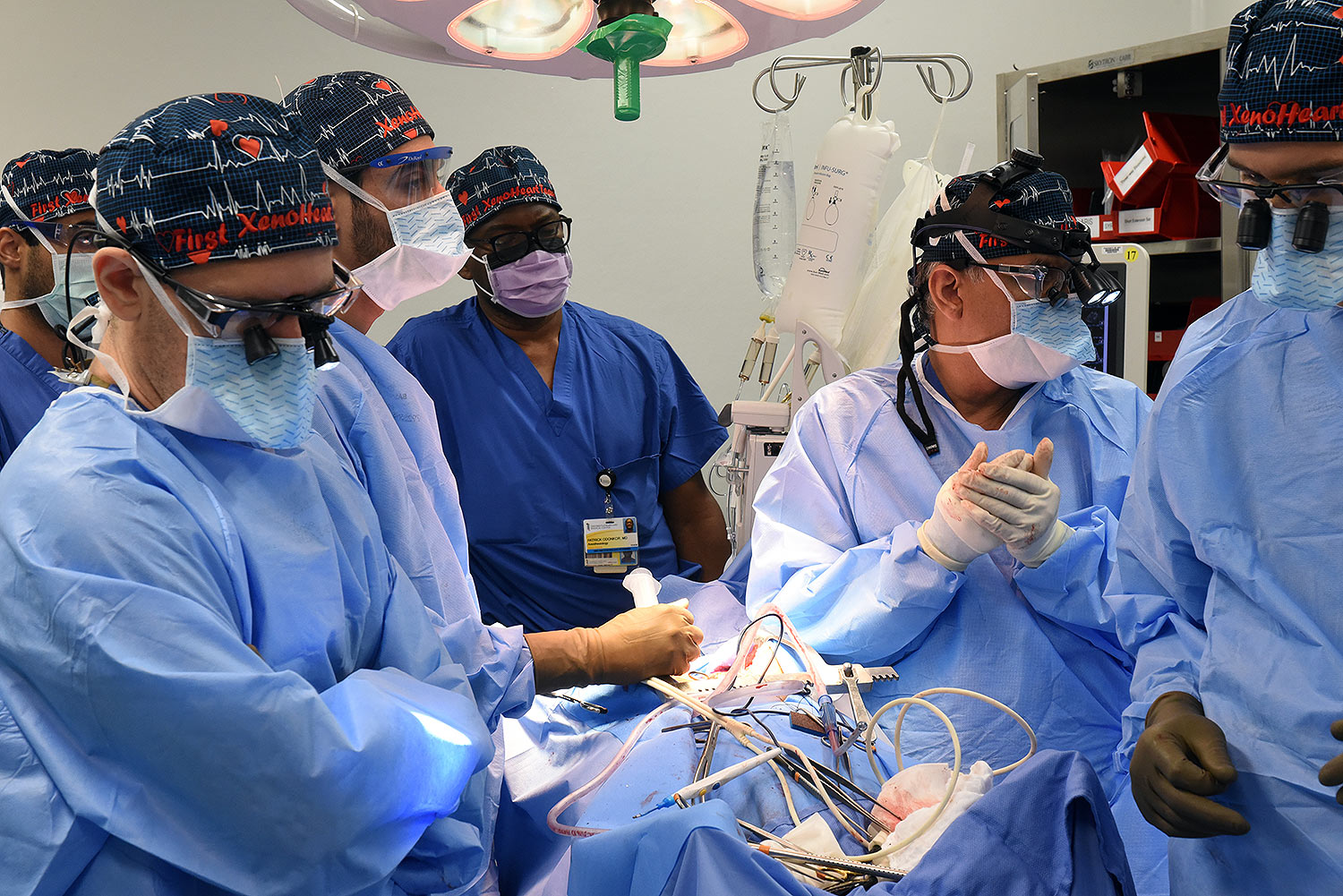
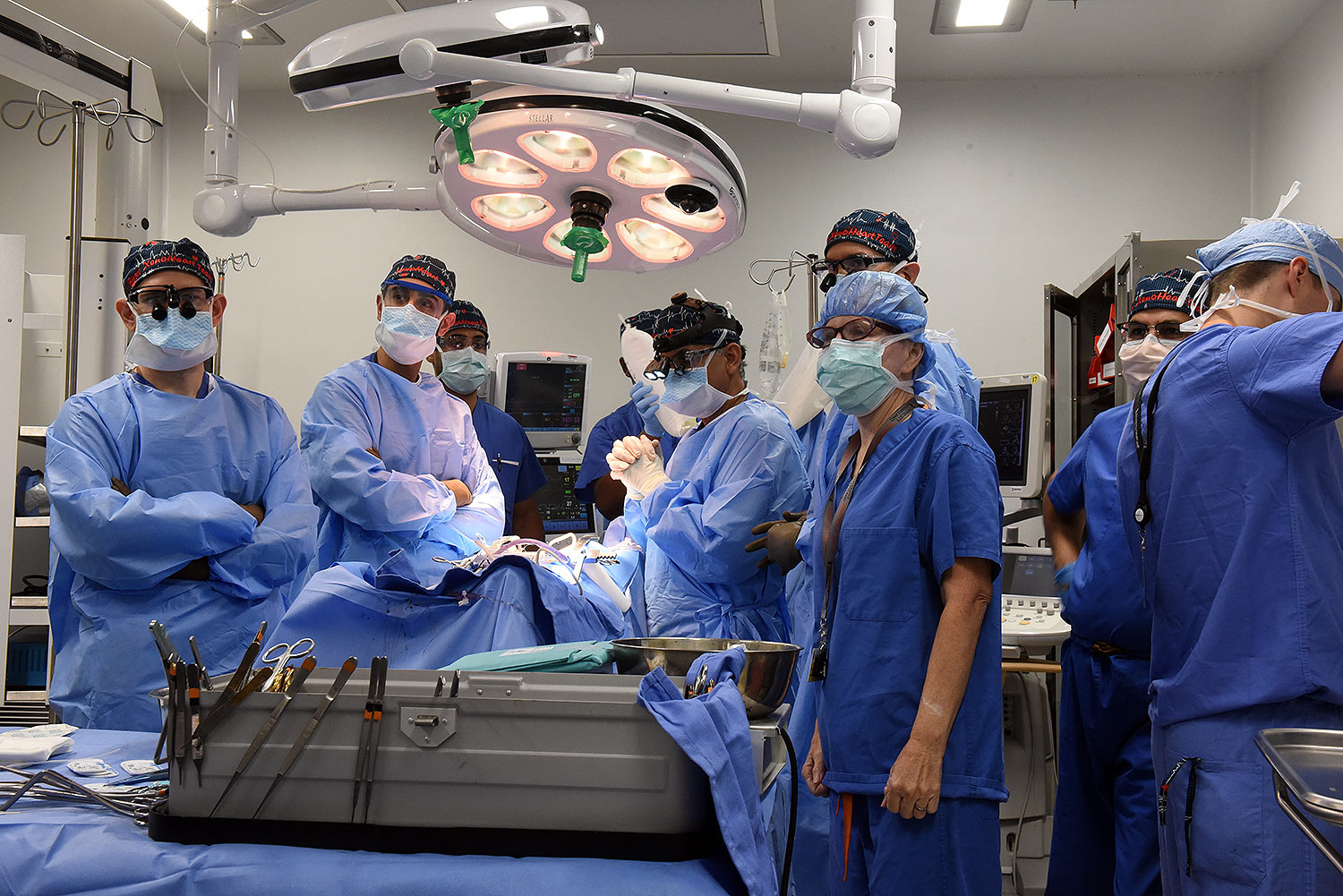
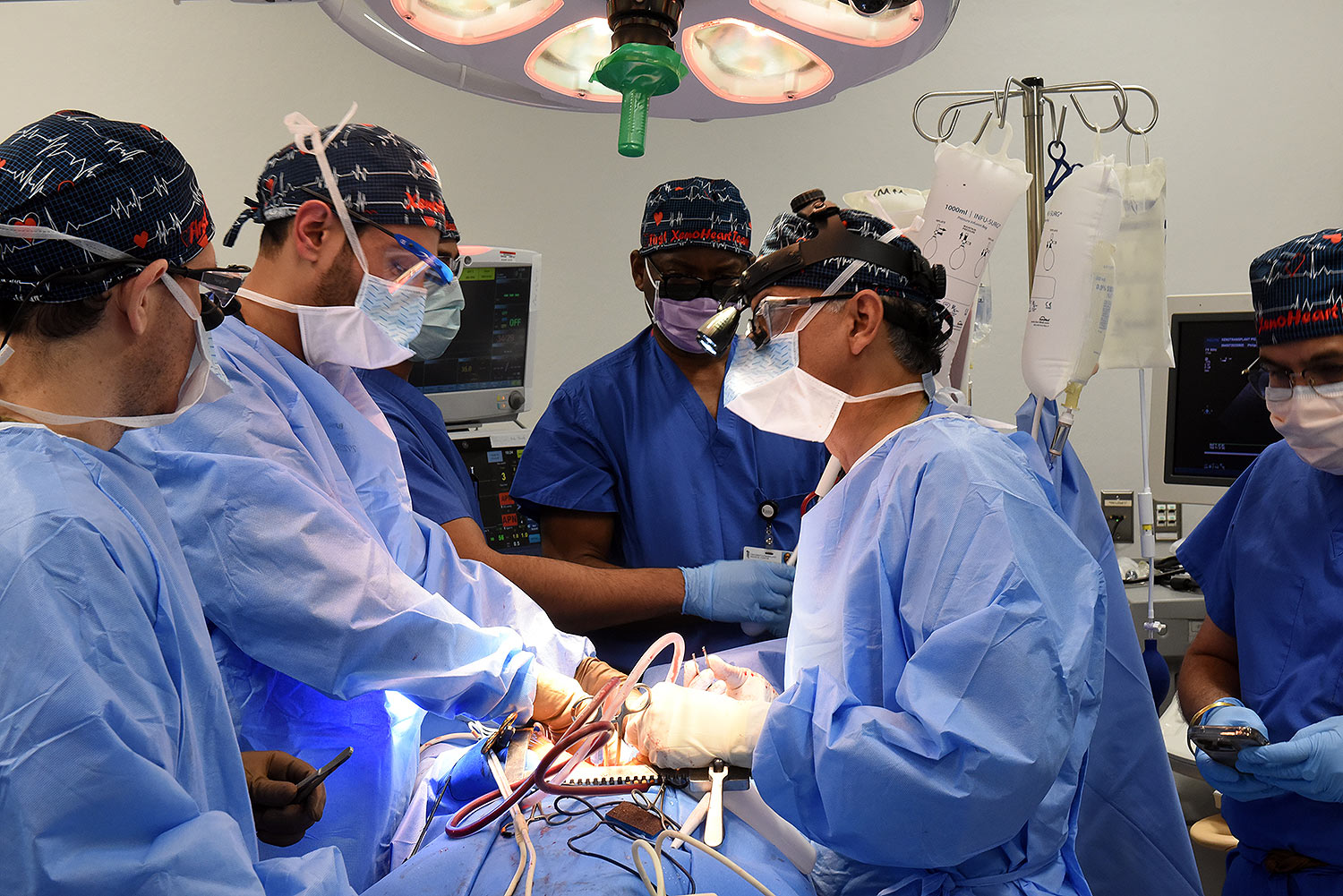
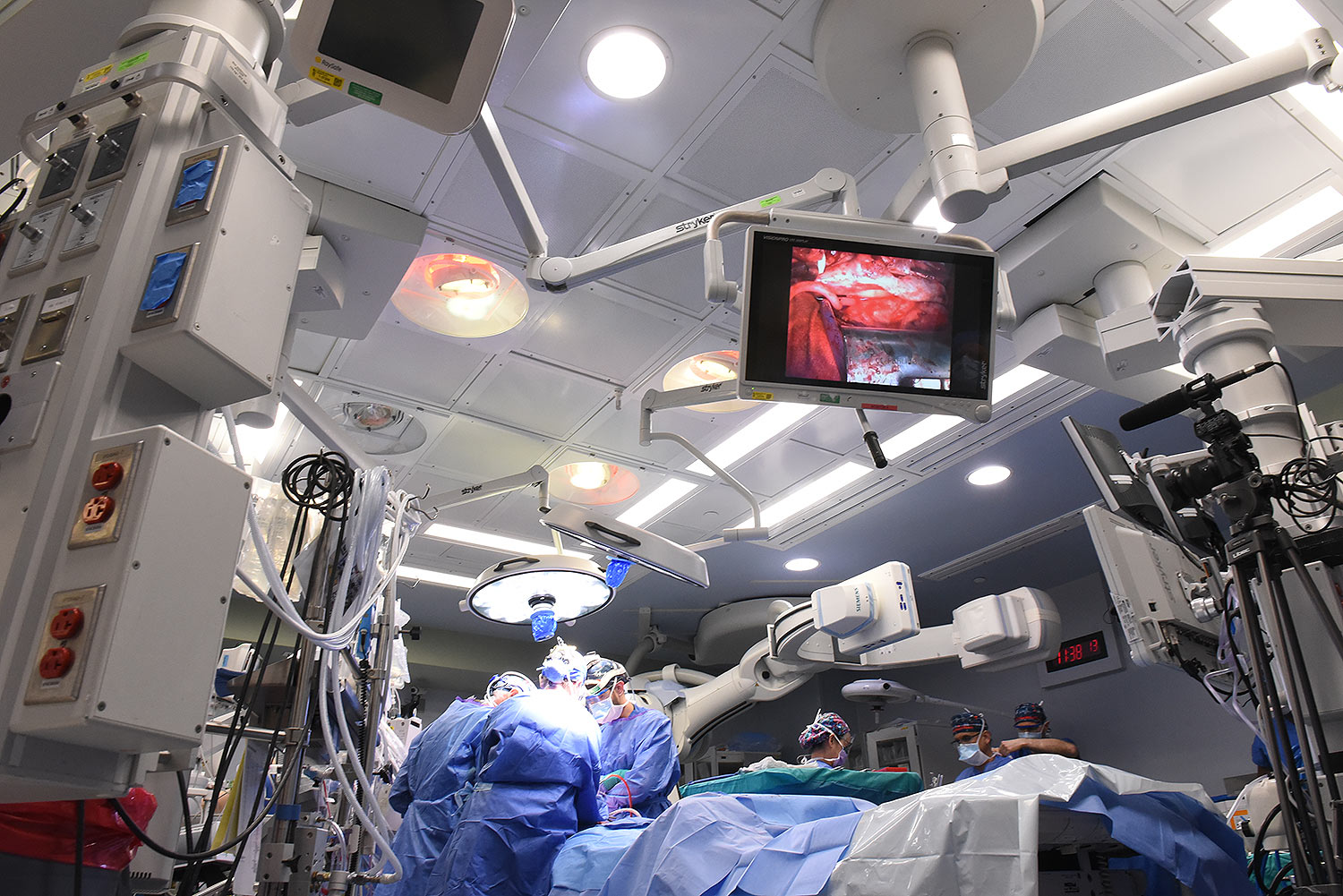
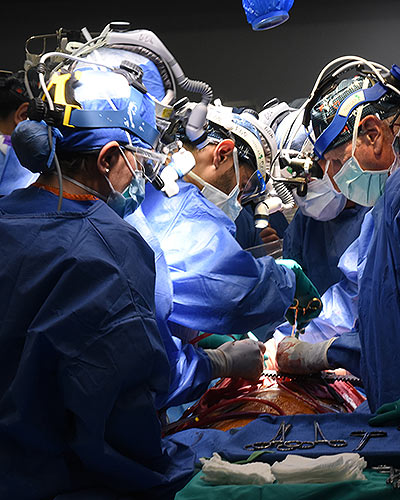
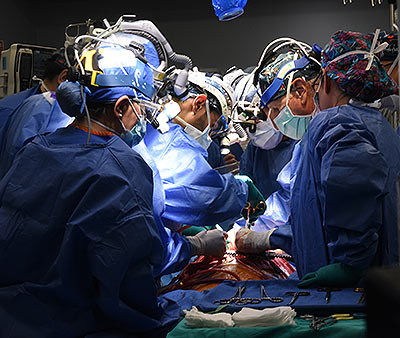 A 58-year-old patient with terminal heart disease became the second patient in the world to receive a historic transplant of a genetically-modified pig heart on September 20. He is recovering and communicating with his loved ones. This is only the second time in the world that a genetically modified pig heart has been transplanted into a living patient. Both historic surgeries were performed by University of Maryland School of Medicine (UMSOM) faculty at the University of Maryland Medical Center (UMMC).
A 58-year-old patient with terminal heart disease became the second patient in the world to receive a historic transplant of a genetically-modified pig heart on September 20. He is recovering and communicating with his loved ones. This is only the second time in the world that a genetically modified pig heart has been transplanted into a living patient. Both historic surgeries were performed by University of Maryland School of Medicine (UMSOM) faculty at the University of Maryland Medical Center (UMMC).
The first historic surgery, performed in January, 2022, was conducted on David Bennett by University of Maryland Medicine surgeons (comprising UMSOM and UMMC), who are recognized as the leaders in cardiac xenotransplantation. This new patient, Lawrence Faucette, had end-stage heart disease. He was deemed ineligible for a traditional transplant with a human heart, by UMMC and several other leading transplant hospitals, due to his pre-existing peripheral vascular disease and complications with internal bleeding.
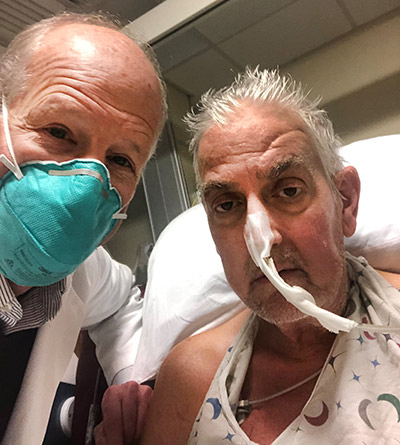
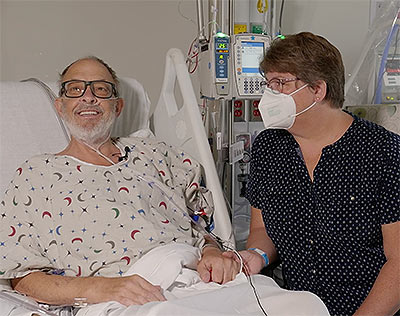 This transplant was the only option available for Mr. Faucette who was facing near-certain death from heart failure. The patient, who lives in Frederick, MD, is a married father of two and a 20-year Navy veteran and most recently worked as a lab technician at the National Institutes of Health before his retirement. He is currently breathing on his own, and his heart is functioning well without any assistance from supportive devices.
This transplant was the only option available for Mr. Faucette who was facing near-certain death from heart failure. The patient, who lives in Frederick, MD, is a married father of two and a 20-year Navy veteran and most recently worked as a lab technician at the National Institutes of Health before his retirement. He is currently breathing on his own, and his heart is functioning well without any assistance from supportive devices.
“My only real hope left is to go with the pig heart, the xenotransplant,” said Mr. Faucette during an interview from his hospital room a few days before his surgery. “Dr. Griffith, Dr. Mohiuddin and their entire staff have been incredible, but nobody knows from this point forward. At least now I have hope, and I have a chance."
 Added his wife, Ann Faucette: “We have no expectations other than hoping for more time together. That could be as simple as sitting on the front porch and having coffee together."
Added his wife, Ann Faucette: “We have no expectations other than hoping for more time together. That could be as simple as sitting on the front porch and having coffee together."
The U.S. Food and Drug Administration granted emergency approval for the surgery on Friday September 15 through its single patient investigational new drug (IND) “compassionate use” pathway. This approval process is used when an experimental medical product, in this case the genetically-modified pig’s heart, is the only option available for a patient faced with a serious or life-threatening medical condition. The approval was granted in the hope of saving the patient’s life.
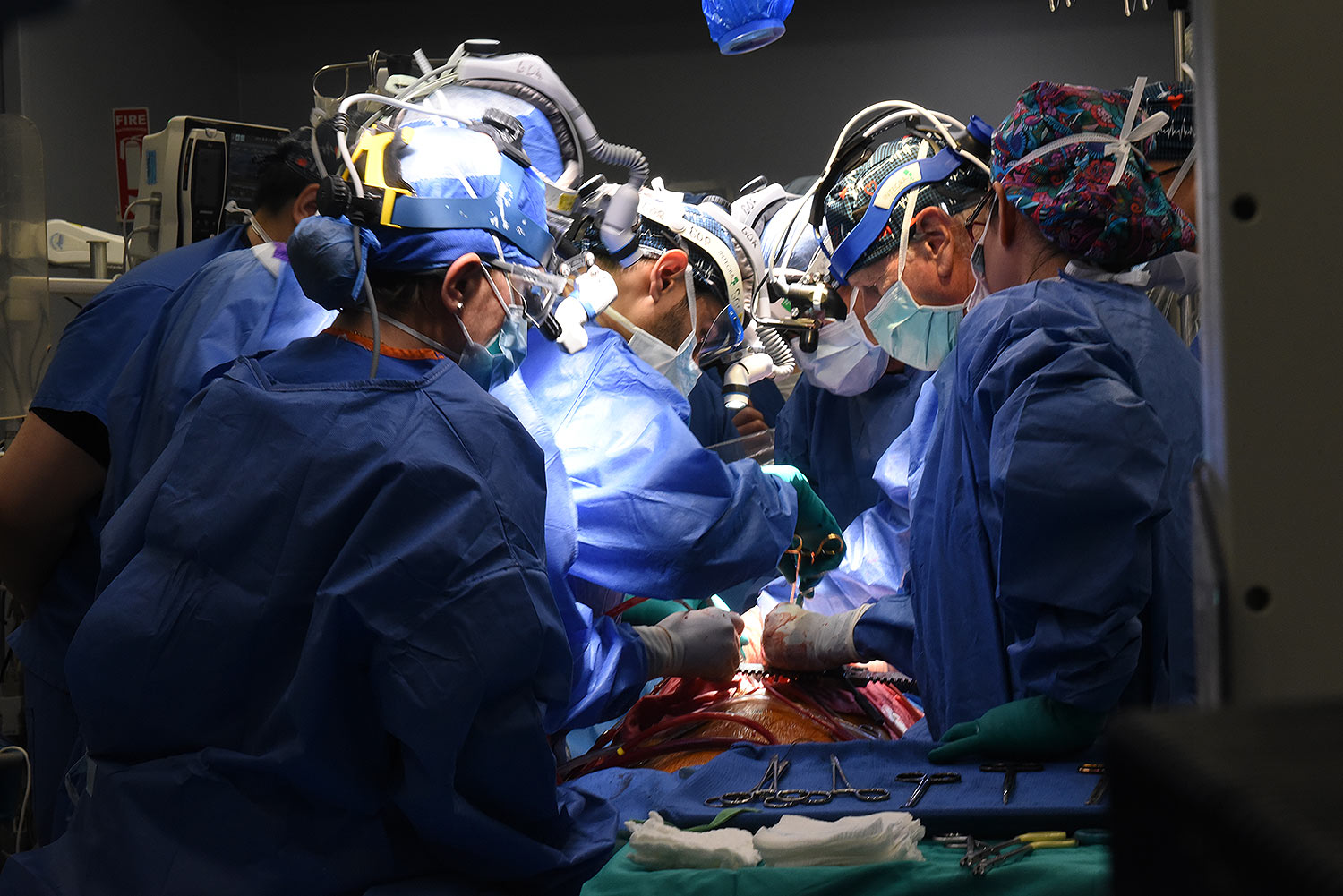
“We are once again offering a dying patient a shot at a longer life, and we are incredibly grateful to Mr. Faucette for his bravery and willingness to help advance our knowledge of this field,” said Bartley P. Griffith, MD, who surgically transplanted the pig heart into both the first and second patient at UMMC. Dr. Griffith is the Thomas E. and Alice Marie Hales Distinguished Professor in Transplant Surgery and Clinical Director of the Cardiac Xenotransplantation Program at UMSOM. “We are hopeful that he will get home soon to enjoy more time with his wife and the rest of his loving family.”
 Considered one of the world’s foremost experts on xenotransplantation, Muhammad M. Mohiuddin, MD, Professor of Surgery at UMSOM, joined the UMSOM faculty seven years ago and established the Cardiac Xenotransplantation Program. Dr. Mohiuddin serves as the program’s Program/Scientific Director. Dr Mohiuddin co-led this procedure with Dr Griffith.
Considered one of the world’s foremost experts on xenotransplantation, Muhammad M. Mohiuddin, MD, Professor of Surgery at UMSOM, joined the UMSOM faculty seven years ago and established the Cardiac Xenotransplantation Program. Dr. Mohiuddin serves as the program’s Program/Scientific Director. Dr Mohiuddin co-led this procedure with Dr Griffith.
“We are continuing to pursue the pathway to clinical trials by providing important new data on pre-clinical research that has been requested by the FDA,” said Dr. Mohiuddin. “The FDA used our data from these new studies, as well as our experience with the first patient, to determine that we were ready to attempt a second transplant in an end-stage heart disease patient who had no other treatment options.”
About 110,000 Americans are currently waiting for an organ transplant, and more than 6,000 patients die each year before getting one, according to the federal government’s organdonor.gov. Transplanting animal organs (known as xenotransplantation) could potentially save thousands of lives but carries a unique set of risks. Besides the fear of transmitting an unknown pathogen from the animal to human, xenotransplants are more likely to trigger a dangerous immune response. These responses can trigger an immediate rejection of the organ with a potentially deadly outcome to the patient.
Watch the video
This video can also be viewed on YouTube. You will need to login to view it.
 “As a cardiothoracic surgeon who does lung transplants, I am so grateful to our team of surgeons who are working to help solve the organ shortage crisis,” said Christine Lau, MD, MBA the Dr. Robert W. Buxton Professor and Chair of the Department of Surgery at UMSOM and Surgeon-in-Chief at UMMC. “Once again, we are at the forefront of a historic accomplishment that brings us one step closer to making xenotransplantation a life-saving reality for patients in need.”
“As a cardiothoracic surgeon who does lung transplants, I am so grateful to our team of surgeons who are working to help solve the organ shortage crisis,” said Christine Lau, MD, MBA the Dr. Robert W. Buxton Professor and Chair of the Department of Surgery at UMSOM and Surgeon-in-Chief at UMMC. “Once again, we are at the forefront of a historic accomplishment that brings us one step closer to making xenotransplantation a life-saving reality for patients in need.”
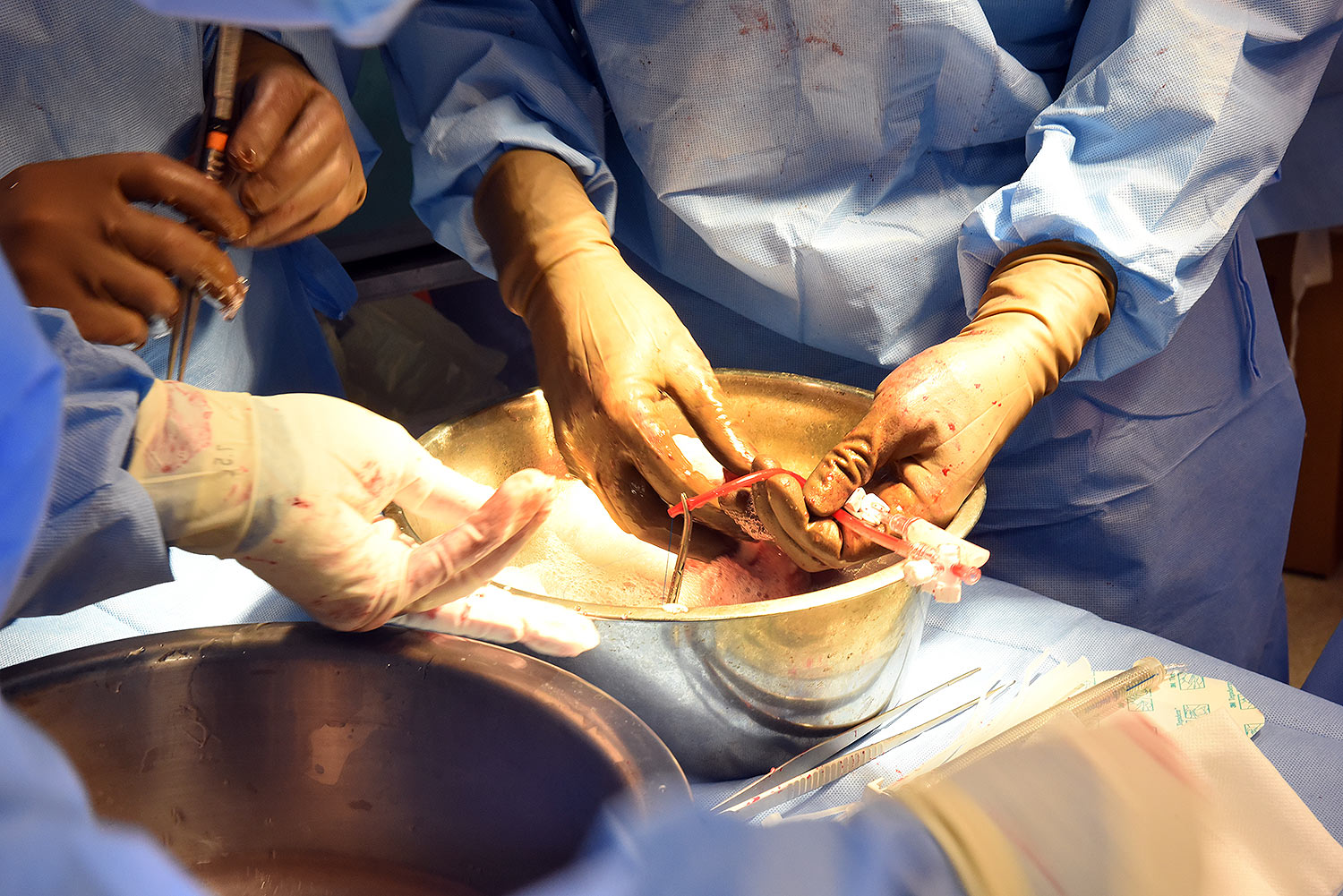
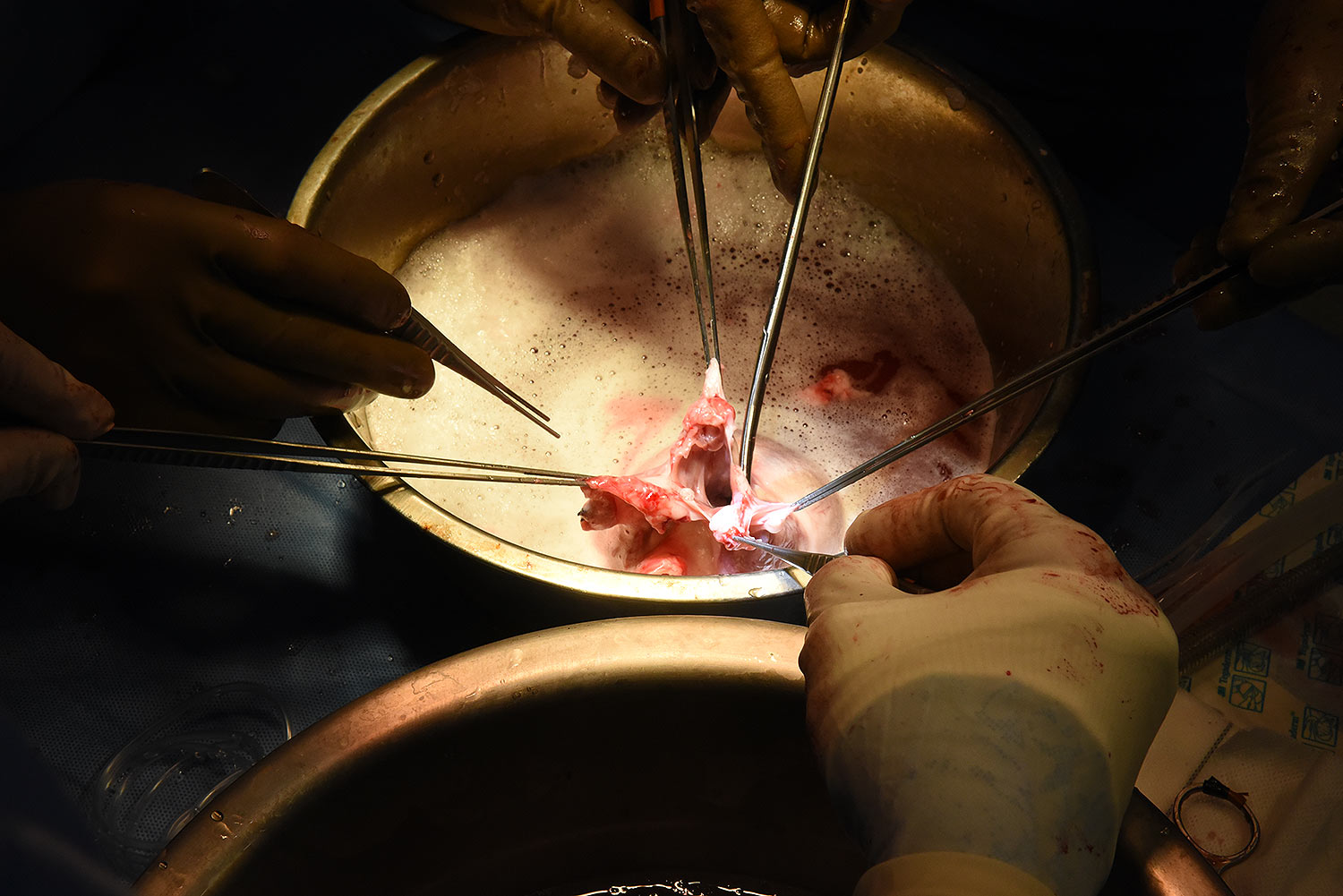
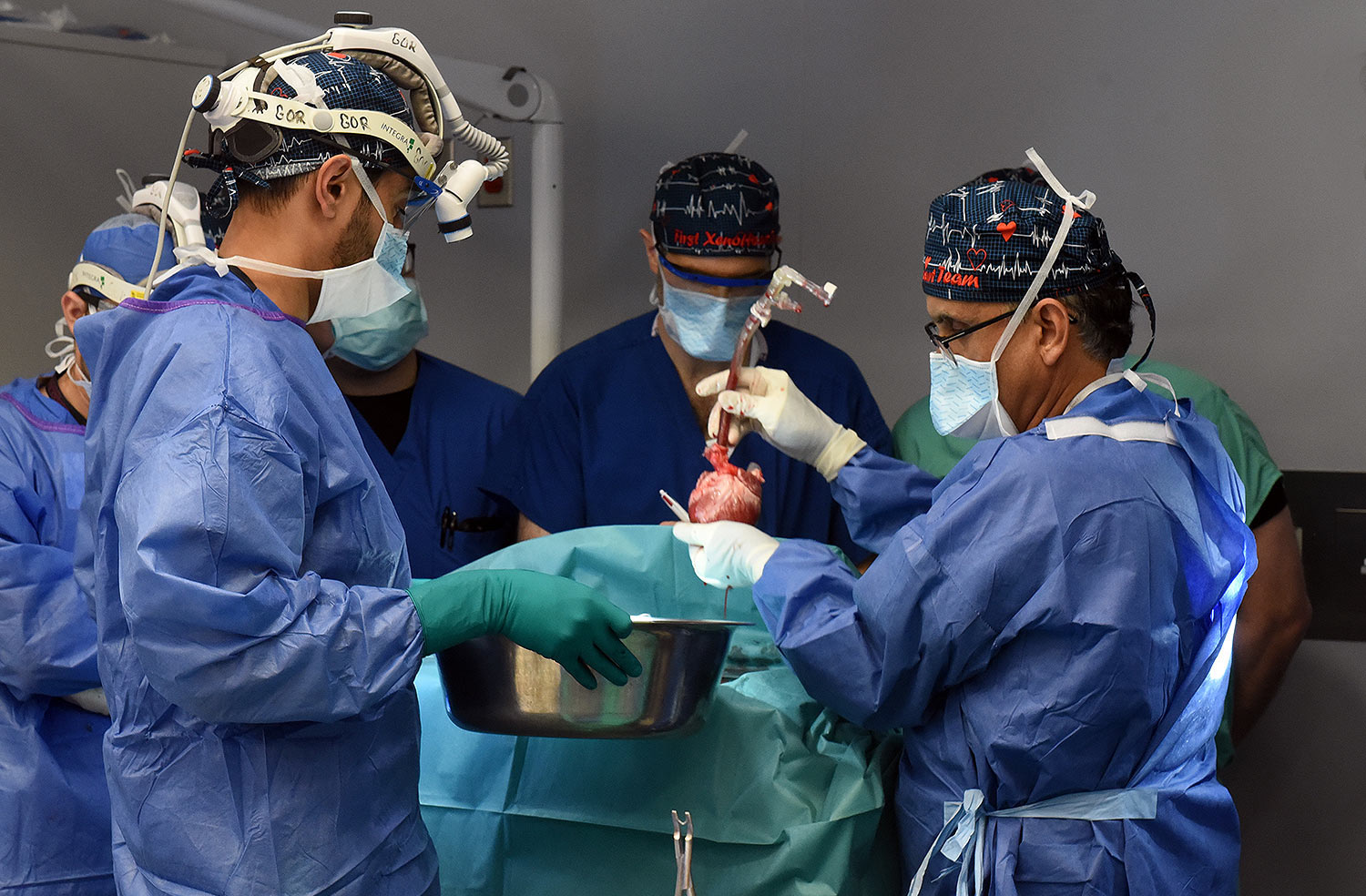
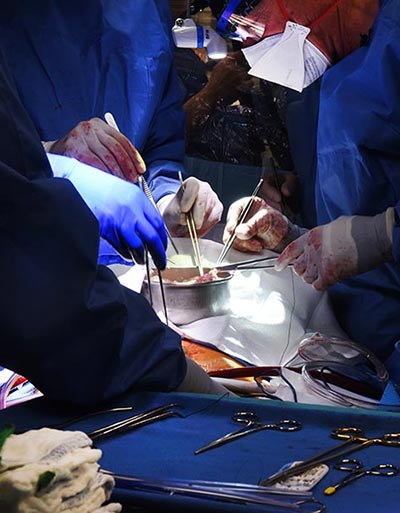
United Therapeutics Corporation, through its xenotransplantation subsidiary Revivicor, based in Blacksburg, VA, provided the genetically-modified pig to the xenotransplantation laboratory at UMSOM. On the morning of the transplant surgery, the surgical team, led by Dr. Griffith and Dr. Mohiuddin, removed the pig’s heart and placed it in the XVIVO Heart Box, a machine perfusion device, to keep the heart preserved until surgery.
 The physician-scientists are also treating the patient with a novel antibody therapy along with conventional anti-rejection drugs, which are designed to suppress the immune system and prevent the body from damaging or rejecting the foreign organ. The novel therapy being developed by Eledon Pharmaceuticals is an experimental antibody, called tegoprubart; it blocks CD154, a protein involved in immune system activation.
The physician-scientists are also treating the patient with a novel antibody therapy along with conventional anti-rejection drugs, which are designed to suppress the immune system and prevent the body from damaging or rejecting the foreign organ. The novel therapy being developed by Eledon Pharmaceuticals is an experimental antibody, called tegoprubart; it blocks CD154, a protein involved in immune system activation.
Before consenting to receive the transplant, Mr. Faucette was fully informed of the procedure’s risks, and that the procedure was experimental with unknown risks and benefits. He was admitted to UMMC on Thursday, September 14 after experiencing complications from his heart failure and peripheral vascular disease. Mr. Faucette underwent a psychiatric evaluation and met with a medical ethicist, social workers and other members of the UMMC care team to discuss the procedure’s risks and benefits and to obtain his informed consent.
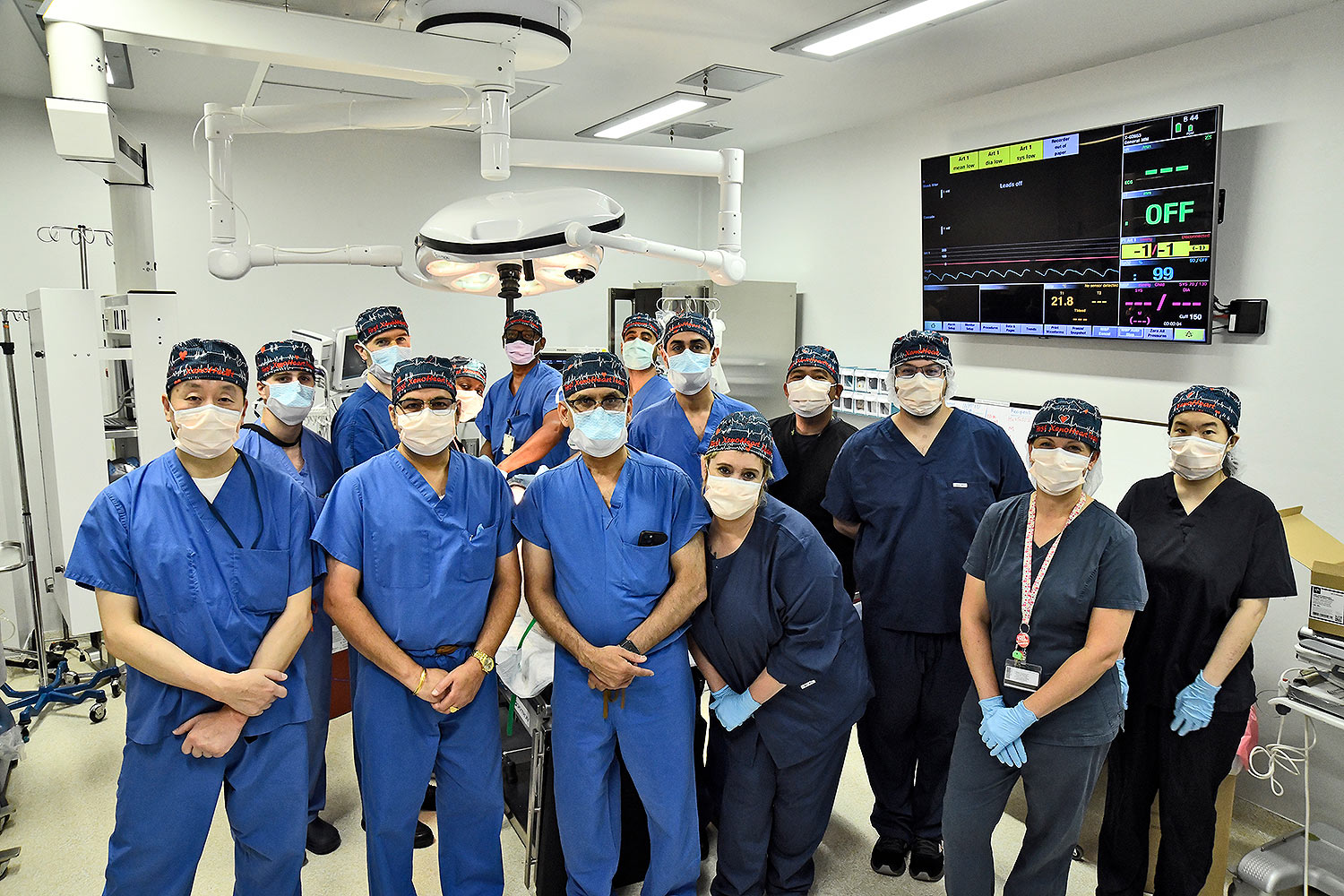
“This innovative program embodies the future of molecular medicine in surgery and speaks to a possible future where organs may be available to all patients,” said UMSOM Dean Mark Gladwin MD, who is also Executive Vice President for Medical Affairs, UM Baltimore, and the John Z. and Akiko K. Bowers Distinguished Professor at UMSOM. “We recognize a heroic partnership with Mr. Faucette and his family, as we partner to advance the field of transplantation medicine into the next era. I appreciate the hard work of so many of our clinical, research and administrative teams at the University of Maryland Medicine. They have worked so hard over the last year to prepare for this day, doing everything possible to optimize the outcome of this historic surgery.”
 “This transplant is another remarkable achievement for medicine and humanity that would not have been possible without the close relationship between University of Maryland Medical Center and our University of Maryland School of Medicine partners,” said Bert W. O'Malley, MD, President and CEO of the University of Maryland Medical Center. “The Faucettes and thousands of families like them are the reason we are pressing onward to propel the xenotransplantation field forward. We are immensely proud to have taken another significant leap toward a day when more people who need a lifesaving organ transplant can get one.”
“This transplant is another remarkable achievement for medicine and humanity that would not have been possible without the close relationship between University of Maryland Medical Center and our University of Maryland School of Medicine partners,” said Bert W. O'Malley, MD, President and CEO of the University of Maryland Medical Center. “The Faucettes and thousands of families like them are the reason we are pressing onward to propel the xenotransplantation field forward. We are immensely proud to have taken another significant leap toward a day when more people who need a lifesaving organ transplant can get one.”
 “This is an exciting time for everyone in the xenotransplantation field,” said Mohan Suntha, MD, MBA, University of Maryland Medical System President and CEO. “We’ve seen an astonishing amount of progress in a short period of time and our System is proud to be part of this incredible milestone. This is the result of the resolve and tenacity of researchers who have held fast to the vision over decades. Those team members who have been directly involved in this work as well as those who have watched in hopeful interest are each part of a medical community that can feel the magnitude of this moment.”
“This is an exciting time for everyone in the xenotransplantation field,” said Mohan Suntha, MD, MBA, University of Maryland Medical System President and CEO. “We’ve seen an astonishing amount of progress in a short period of time and our System is proud to be part of this incredible milestone. This is the result of the resolve and tenacity of researchers who have held fast to the vision over decades. Those team members who have been directly involved in this work as well as those who have watched in hopeful interest are each part of a medical community that can feel the magnitude of this moment.”
Organs from genetically modified pigs have been the focus of much of the research in xenotransplantation, in part because of physiologic similarities between pigs and human and nonhuman primates. United Therapeutics has funded a $22 million research program to test their genetically-modified pig hearts from Revivicor in baboon studies conducted at UMSOM.
Three genes--responsible for a rapid antibody-mediated rejection of pig organs by humans—were “knocked out” in the donor pig. Six human genes responsible for immune acceptance of the pig heart were inserted into the genome. One additional gene in the pig was knocked out to prevent excessive growth of the pig heart tissue, for a total of 10 unique gene edits made in the donor pig.
“This procedure is another significant step forward in bringing our vision of lifesaving xenotransplantation to those patients in desperate need,” said David Ayares, PhD, President and Chief Scientific Officer of United Therapeutics Corporation’s Revivicor subsidiary. “This second successful transplantation of United Therapeutics’ UHeart™ is a product of decades of gene editing, animal husbandry, and creative thinking by the team of scientists at United Therapeutics and Revivicor, and at the University of Maryland—especially Drs. Mohiuddin and Griffith. All of us at United Therapeutics recognize the bravery and unconditional willingness by Mr. Faucette to advance the cause of science and medical treatment in this remarkable way.”
During the nearly two years since the first surgery, UMSOM faculty-scientists have extensively investigated Mr. Bennett’s experience with the world’s first genetically modified cardiac xenotransplant. They published their initial findings in the New England Journal of Medicine and then published their follow-up findings from an extensive investigation in The Lancet. They demonstrated that the pig heart functioned well in the patient for several weeks with no signs of acute rejection. Mr. Bennett’s death from heart failure was likely caused by a multitude of factors including his poor state of health that left him hospitalized on a heart-lung bypass machine for six weeks prior to the transplant.
Prior to performing the first surgery in Mr. Bennett in 2022, Dr. Mohiuddin, Dr. Griffith, and their research team spent five years perfecting the surgical technique on non-human primates. Dr. Mohiuddin’s xenotransplant research experience spans over 30 years, during which time he demonstrated in peer-reviewed research that a genetically-modified pig’s heart can function when placed in the abdomen for as long as three years.
Xenotransplant Image gallery
About the University of Maryland School of Medicine
Now in its third century, the University of Maryland School of Medicine was chartered in 1807 as the first public medical school in the United States. It continues today as one of the fastest growing, top-tier biomedical research enterprises in the world -- with 46 academic departments, centers, institutes, and programs, and a faculty of more than 3,000 physicians, scientists, and allied health professionals, including members of the National Academy of Medicine and the National Academy of Sciences, and a distinguished two-time winner of the Albert E. Lasker Award in Medical Research. With an operating budget of more than $1.2 billion, the School of Medicine works closely in partnership with the University of Maryland Medical Center and Medical System to provide research-intensive, academic and clinically based care for nearly 2 million patients each year. The School of Medicine has nearly $600 million in extramural funding, with most of its academic departments highly ranked among all medical schools in the nation in research funding. As one of the seven professional schools that make up the University of Maryland, Baltimore campus, the School of Medicine has a total population of nearly 9,000 faculty and staff, including 2,500 students, trainees, residents, and fellows. The combined School of Medicine and Medical System (“University of Maryland Medicine”) has an annual budget of over $6 billion and an economic impact of nearly $20 billion on the state and local community. The School of Medicine, which ranks as the 8th highest among public medical schools in research productivity (according to the Association of American Medical Colleges profile) is an innovator in translational medicine, with 606 active patents and 52 start-up companies. In the latest U.S. News & World Report ranking of the Best Medical Schools, published in 2023, the UM School of Medicine is ranked #10 among the 92 public medical schools in the U.S., and in the top 16 percent (#32) of all 192 public and private U.S. medical schools. The School of Medicine works locally, nationally, and globally, with research and treatment facilities in 36 countries around the world. Visit medschool.umaryland.edu
About the University of Maryland Medical Center
The University of Maryland Medical Center (UMMC) is comprised of two hospital campuses in Baltimore: the 800-bed flagship institution of the 11-hospital University of Maryland Medical System (UMMS) and the 200-bed UMMC Midtown Campus. Both campuses are academic medical centers for training physicians and health professionals and for pursuing research and innovation to improve health. UMMC's downtown campus is a national and regional referral center for trauma, cancer care, neurosciences, advanced cardiovascular care, and women's and children's health, and has one of the largest solid organ transplant programs in the country. All physicians on staff at the downtown campus are clinical faculty physicians of the University of Maryland School of Medicine. The UMMC Midtown Campus medical staff is predominantly faculty physicians specializing in a wide spectrum of medical and surgical subspecialties, primary care for adults and children and behavioral health. UMMC Midtown has been a teaching hospital for 140 years and is located one mile away from the downtown campus. For more information, visit www.umm.edu.
About the University of Maryland Medical System
The University of Maryland Medical System (UMMS) is an academic private health system, focused on delivering compassionate, high quality care and putting discovery and innovation into practice at the bedside. Partnering with the University of Maryland School of Medicine and University of Maryland, Baltimore who educate the state's future health care professionals, UMMS is an integrated network of care, delivering 25 percent of all hospital care in urban, suburban and rural communities across the state of Maryland. UMMS puts academic medicine within reach through primary and specialty care delivered at 11 hospitals, including the flagship University of Maryland Medical Center, the System's anchor institution in downtown Baltimore, as well as through a network of University of Maryland Urgent Care centers and more than 150 other locations in 13 counties. For more information, visit www.umms.org.
Contact
Deborah Kotz
Senior Director of Media Relations
Office of Public Affairs & Communications
University of Maryland School of Medicine
Email: DKotz@som.umaryland.edu
o: 410-706-4255
c: 410-804-0054
t: @debkotz2
Related stories
Wednesday, January 08, 2025
Presenting a Path Forward for Future Genetically-Modified Pig Heart Transplants: Lessons Learned from Second Patient
Continuing significant advancements in the field of xenotransplantation, surgeon-scientists from the University of Maryland School of Medicine provided an extensive analysis on the second patient in the world to receive a genetically-modified pig organ. Lawrence Faucette, 58, received a pig heart at the University of Maryland Medical Center in 2023 to treat his end-stage heart failure. He lived for 40 days before choosing to forgo additional treatment after the transplant began to fail due to rejection.

Wednesday, January 31, 2024
Renowned Surgeon Dr. Bartley Griffith Named Vice Chair for Innovation in UM School of Medicine’s Department of Surgery
University of Maryland School of Medicine (UMSOM) Department of Surgery Chair Christine Lau, MD, MBA, along with UMSOM Dean Mark T. Gladwin, MD, announced today the appointment of Bartley P. Griffith, MD, as the Department of Surgery’s first Vice Chair for Innovation. In this role, Dr. Griffith will nurture a culture of innovation, entrepreneurship, and collaboration in the Department, and expand the integration of related sciences into surgical practice. The appointment is effective on February 1.
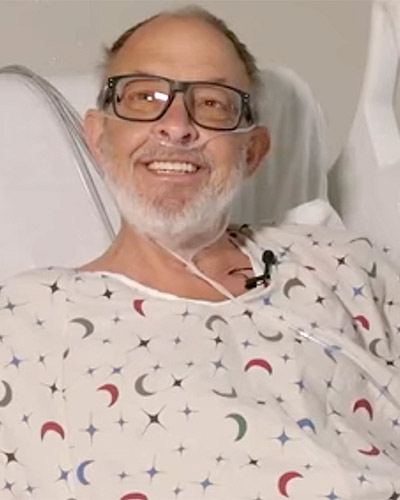
Tuesday, October 31, 2023
In Memoriam: Lawrence Faucette
It is with great sadness that we announce the passing of Lawrence Faucette, the 58-year-old patient with terminal heart disease who received the world’s second genetically-modified pig heart transplant. Mr. Faucette received the transplant on September 20 and lived for nearly six weeks following the surgery.
Friday, June 30, 2023
Lessons Learned from World’s First Successful Transplant of Genetically-Modified Pig Heart into Human Patient
A new study published today in the Lancet has revealed the most extensive analysis to date on what led to the eventual heart failure in the world's first successful transplant of a genetically-modified pig heart into a human patient. This groundbreaking procedure was conducted by University of Maryland School of Medicine (UMSOM) physician-scientists back in January 2022 and marked an important milestone for medical science.

Friday, December 16, 2022
UM School of Medicine Surgeon-Scientist Named One of Nature’s 10 People Who Helped Shape the Science Stories of 2022
The world-renowned journal Nature, named Muhammad Mohiuddin, MD, DSc, Program and Scientific Director of the Cardiac Xenotransplantation Program at the University of Maryland School of Medicine (UMSOM), on its annual list of 10 people who helped shaped science in 2022. His pivotal work over the past three decades transplanting genetically-modified pig hearts into non-human primates led to the historic xenotransplant of a pig heart into a human patient this past January. The surgery was led by Bartley Griffith, MD, the Thomas E. and Alice Marie Hales Distinguished Professor of Transplant Surgery and Clinical Director of the Cardiac Xenotransplantation Program, who was also recognized by Nature for his ground-breaking efforts to move the field of transplantation into a new era.

Monday, November 14, 2022
Unexpected Electrical Changes Seen in First Successful Transplant of Genetically-Modified Pig Heart
Ten months after transplanting the first genetically-modified pig heart into a human patient, University of Maryland School of Medicine (UMSOM) researchers continue to report on new findings from the landmark transplant. Their latest study demonstrates for the first time that unexpected electrical changes occurred in the pig heart transplanted into the patient David Bennett. The findings were presented at the American Heart Association (AHA) meeting this past weekend.
Wednesday, June 22, 2022
University of Maryland School of Medicine Faculty Scientists and Clinicians Publish Findings of World’s First Successful Transplant of Genetically Modified Pig Heart into Human Patient
Six months ago, University of Maryland School of Medicine surgeon-scientists successfully implanted a genetically modified pig heart into a 57 year-old patient with terminal heart disease in a first-of-its-kind surgery. It was considered an early success because the patient lived for two months with a strong functioning heart showing no obvious signs of rejection, according to a new paper published today in the New England Journal of Medicine.

Wednesday, March 09, 2022
IN MEMORIAM: David Bennett, Sr.
David Bennett, the 57 year old patient with terminal heart disease who made history as the first person to receive a genetically modified pig’s heart, passed away yesterday on March 8. Mr. Bennett received the transplant on January 7 and lived for two months following the surgery. His condition began deteriorating several days ago. After it became clear that he would not recover, he was given compassionate palliative care. He was able to communicate with his family during his final hours.