New Technique Consistently Works to Open Blood-Brain Barrier, Paving Way for Pre-Clinical Studies of Neurologic Drugs
January 31, 2022 | Vanessa McMains
University of Maryland School of Medicine researchers Piotr Walczak and Miroslaw Janowski devised protocol provides a way to better test a backlog of potential therapeutics for brain cancer, neurodegenerative disorders, and mental illness
 University of Maryland School of Medicine researchers developed a technique in laboratory animals to consistently and reproducibly open the blood-brain barrier (BBB). This barrier serves as a barricade securing the brain from the external world blocking out certain environmental toxins, but also prevents drug therapies from reaching their intended targets. The new technique is based on a routine procedure for removing clots from the brain’s arteries in patients. This advancement was conducted by Piotr Walczak, MD, PhD, Professor of Diagnostic Radiology and Nuclear Medicine at the University of Maryland School of Medicine, and Miroslaw Janowski, MD, PhD, Associate Professor of Diagnostic Radiology and Nuclear Medicine at the University of Maryland School of Medicine.
University of Maryland School of Medicine researchers developed a technique in laboratory animals to consistently and reproducibly open the blood-brain barrier (BBB). This barrier serves as a barricade securing the brain from the external world blocking out certain environmental toxins, but also prevents drug therapies from reaching their intended targets. The new technique is based on a routine procedure for removing clots from the brain’s arteries in patients. This advancement was conducted by Piotr Walczak, MD, PhD, Professor of Diagnostic Radiology and Nuclear Medicine at the University of Maryland School of Medicine, and Miroslaw Janowski, MD, PhD, Associate Professor of Diagnostic Radiology and Nuclear Medicine at the University of Maryland School of Medicine.
The team published their detailed procedure on December 13, 2021, in Nature Protocols. Their paper essentially provides a roadmap for other researchers to develop and test new therapies for brain diseases. The hope is for researchers to use this procedure for treatments against brain cancer, neurological disorders like epilepsy, neurodegenerative diseases like Alzheimer’s and Parkinson’s, or even mental illnesses. The researchers say the technique can potentially be applied in conjunction with the latest medical discoveries, such as genome editing or gene therapy to treat incurable cancers.
 The procedure uses magnetic resonance imaging (MRI), which provides feedback in real-time, to control where in the brain the blood-brain barrier gate opens, allowing materials to pass through into spaces that they are normally excluded.
The procedure uses magnetic resonance imaging (MRI), which provides feedback in real-time, to control where in the brain the blood-brain barrier gate opens, allowing materials to pass through into spaces that they are normally excluded.
“Scores of interventional radiologists worldwide navigate various sophisticated devices in arteries for standard plumbing tasks in the human brain, like aneurysms or strokes. If there is a leak, they fix it. If there is a clog, they pump it out. This route could be also used to deliver drugs, but the technique had not been perfected in mice and other laboratory animals,” said senior study author Dr. Walczak. “Since most preclinical research starts with mice, it was essential to show how to do this procedure properly in these animals, so scientists across the globe will be able to use it for their drugs to get them to the brain. Some of these drugs will ultimately land in patients as treatments benefiting society.”
Some scientists over the years tried to get drugs into the brains of laboratory animals using other routes such as injecting directly into the brain or the fluid surrounding the brain.
“Researchers had no way of knowing if the drug made it where it was supposed to go at the time of the experiment and some researchers found the procedure unsafe in animals,” said co-author Dr. Janowski, and co-director with Dr. Walczak of the Program in Image-Guided Neurointerventions.
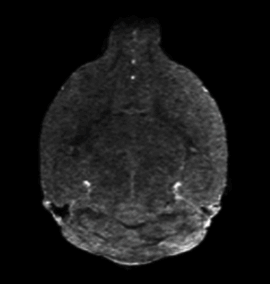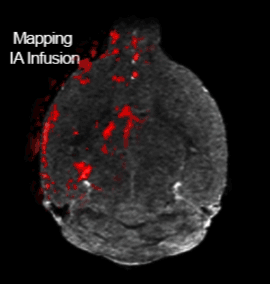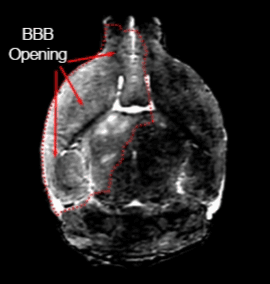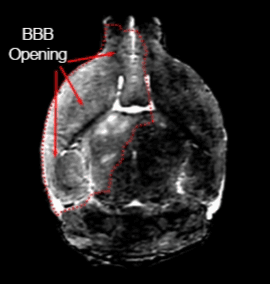 For their specific MRI-guided injection technique, the researchers anesthetized a mouse and surgically inserted the catheter in the neck into the carotid artery that runs to the brain (in people, they use an artery in the groin or hand without requiring surgery). Then, they put the mouse in the MRI machine and performed a scan, while a pump precisely controlled injection speed. To open the blood-brain barrier, the researchers used a solution of mannitol (a type of sugar — a low-cost substance currently used in patients for other treatments) that essentially sucks the liquid out of the cells in blood vessel walls, opening the seals between these cells. Before opening the barrier, they infused gadolinium — a contrast agent used in human medical procedures — through the catheter into the artery, allowing them to see whether the injected material went to its proper destination. If the injection did not work, they adjusted the parameters. Once the conditions were optimized, they opened the barrier in that area of the brain. They used this approach in several other studies targeting biotechnological drugs, such as antibodies, to the brain. Now, the researchers hope their detailed protocol will help other researchers deliver their drug of choice to the brains of their favorite mouse models and eventually help patients.
For their specific MRI-guided injection technique, the researchers anesthetized a mouse and surgically inserted the catheter in the neck into the carotid artery that runs to the brain (in people, they use an artery in the groin or hand without requiring surgery). Then, they put the mouse in the MRI machine and performed a scan, while a pump precisely controlled injection speed. To open the blood-brain barrier, the researchers used a solution of mannitol (a type of sugar — a low-cost substance currently used in patients for other treatments) that essentially sucks the liquid out of the cells in blood vessel walls, opening the seals between these cells. Before opening the barrier, they infused gadolinium — a contrast agent used in human medical procedures — through the catheter into the artery, allowing them to see whether the injected material went to its proper destination. If the injection did not work, they adjusted the parameters. Once the conditions were optimized, they opened the barrier in that area of the brain. They used this approach in several other studies targeting biotechnological drugs, such as antibodies, to the brain. Now, the researchers hope their detailed protocol will help other researchers deliver their drug of choice to the brains of their favorite mouse models and eventually help patients.
“Arterial procedures are typically guided using x-ray imaging methods, and that only lets you see the map of the highways in the brain, but these maps are not detailed enough if you needed to go beyond that to the backroads to reach the forest of the brain cells,” said Dr. Janowski. “We believe that by adding MRI, we closed the gap, both in animal studies and in the future in the clinical trials, by providing the necessary level of precision for opening the gate to the brain for the drugs.”
 University of Maryland School of Medicine Dean E. Albert Reece, MD, PhD, MBA, who is Executive Vice President for Medical Affairs and the John Z. and Akiko K. Bowers Distinguished Professor, said, “Perfecting basic science techniques like this one are key to laying the groundwork to advancing treatment options for the many diseases of the brain. Sometimes in order to advance clinical research, we have to go back to basics first.”
University of Maryland School of Medicine Dean E. Albert Reece, MD, PhD, MBA, who is Executive Vice President for Medical Affairs and the John Z. and Akiko K. Bowers Distinguished Professor, said, “Perfecting basic science techniques like this one are key to laying the groundwork to advancing treatment options for the many diseases of the brain. Sometimes in order to advance clinical research, we have to go back to basics first.”
Additional authors of the study included Post-Doctoral Fellows Chengyan Chu, MD, Yue Gao, MD, and Xiaoyan Lan, MD; Research Associate Anna Jablonska, PhD, Yajie Liang, MD, PhD, Assistant Professor of Diagnostic Radiology and Nuclear Medicine, and Monica Pearl, MD, Adjunct Associate Professor of Diagnostic Radiology and Nuclear Medicine at the University of Maryland School of Medicine; Wojciech Lesniak, PhD, and Guanshu Liu, PhD, of Johns Hopkins Medicine; Shen Li, MD of Dalian Municipal Central Hospital, China; and Tim Magnus, MD, PhD of University Medical Center Hamburg-Eppendorf, Germany.
This work was funded by the Maryland Stem Cell Research Fund (2017-MSCRFF-3942 and 2019-MSCRFF-5031) and grants from the National Institute of Neurological Disorders and Stroke (R01NS091110, R01NS102675, and R21NS091599).
Dr. Pearl, Dr. Janowski, and Dr. Walczak are founders and equity holders in IntraART. Dr. Janowski and Dr. Walczak are founders and equity holders in Ti-Com.
About the University of Maryland School of Medicine
Now in its third century, the University of Maryland School of Medicine was chartered in 1807 as the first public medical school in the United States. It continues today as one of the fastest growing, top-tier biomedical research enterprises in the world -- with 46 academic departments, centers, institutes, and programs, and a faculty of more than 3,000 physicians, scientists, and allied health professionals, including members of the National Academy of Medicine and the National Academy of Sciences, and a distinguished two-time winner of the Albert E. Lasker Award in Medical Research. With an operating budget of more than $1.2 billion, the School of Medicine works closely in partnership with the University of Maryland Medical Center and Medical System to provide research-intensive, academic and clinically based care for nearly 2 million patients each year. The School of Medicine has nearly $600 million in extramural funding, with most of its academic departments highly ranked among all medical schools in the nation in research funding. As one of the seven professional schools that make up the University of Maryland, Baltimore campus, the School of Medicine has a total population of nearly 9,000 faculty and staff, including 2,500 students, trainees, residents, and fellows. The combined School of Medicine and Medical System (“University of Maryland Medicine”) has an annual budget of over $6 billion and an economic impact of nearly $20 billion on the state and local community. The School of Medicine, which ranks as the 8th highest among public medical schools in research productivity (according to the Association of American Medical Colleges profile) is an innovator in translational medicine, with 606 active patents and 52 start-up companies. In the latest U.S. News & World Report ranking of the Best Medical Schools, published in 2021, the UM School of Medicine is ranked #9 among the 92 public medical schools in the U.S., and in the top 15 percent (#27) of all 192 public and private U.S. medical schools. The School of Medicine works locally, nationally, and globally, with research and treatment facilities in 36 countries around the world. Visit medschool.umaryland.edu
Contact
Vanessa McMains
Director, Media & Public Affairs
University of Maryland School of Medicine
Institute of Human Virology
vmcmains@ihv.umaryland.edu
Cell: 443-875-6099
Related stories

Tuesday, May 02, 2023
AI in Medical Imaging Could Magnify Health Inequities, Study Finds
Artificial intelligence (AI) technology in the medical field has the possibility to automate diagnoses, decrease physician workload, and even to bring specialized healthcare to people in rural areas or developing countries. However, with possibility comes potential pitfalls.

Wednesday, April 26, 2023
Long COVID Sufferers with Cognitive Complaints and Mental Health Issues Have Changes in Brain Function, New Study Suggests
Those who experience brain fog, memory issues or other neuropsychiatric symptoms for months after a COVID-19 diagnosis were found to have abnormal brain activity during memory tests on functional magnetic resonance imaging (MRI), according to a new study led by University of Maryland School of Medicine (UMSOM) researchers.

Friday, April 21, 2023
In Memoriam: Rao P. Gullapalli, PhD, MBA
The University of Maryland School of Medicine community is mourning the loss of one of its longtime senior faculty members, Rao P. Gullapalli, PhD, MBA, who was Professor of Diagnostic Radiology and Nuclear Medicine, Associate Vice Chair for Research in the Department and Director of the Core for Translational Research in Imaging (C-TRIM) and Director of the Center for Metabolic Imaging and Therapeutics (CMIT). He also held several leadership roles in cancer imaging at the UM Marlene and Stewart Greenebaum Comprehensive Cancer Center.

Friday, July 29, 2022
Children Who Lack Sleep May Experience Detrimental Impact on Brain and Cognitive Development That Persists Over Time, UM School of Medicine Study Finds
Elementary school-age children who get less than nine hours of sleep per night have significant differences in certain brain regions responsible for memory, intelligence, and well-being compared to those who get the recommended 9-12 hours of sleep per night, according to a new study led by University of Maryland School of Medicine (UMSOM) researchers. Such differences correlated with greater mental health problems like depression, anxiety, and impulsive behaviors in those who lacked sleep. Inadequate sleep was also linked to cognitive difficulties with memory, problem solving and decision making. The findings were published today in the journal Lancet Child & Adolescent Health.