University of Maryland Medicine's Novel Critical Care Resuscitation Unit Improves Patients' Chances of Survival, Study Finds
January 13, 2020 | Deborah Kotz
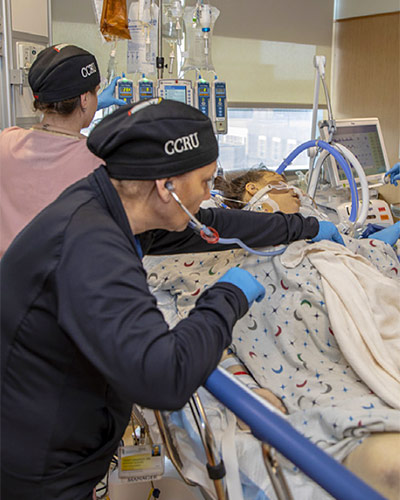
Critically Ill Patients Who Were Transferred to the UM Medicine’s Specialized Resuscitation Unit Had Better Outcomes Than Those Transferred Directly to a Traditional Intensive Care Unit
Patients with acutely life-threatening health conditions who were treated in the University of Maryland Medical Center's (UMMC) innovative Critical Care Resuscitation Unit (CCRU) received faster treatment and had better health outcomes, including a 36 percent lower risk of dying than those who were transferred from a hospital’s emergency department then evaluated and treated in a traditional intensive care unit, according to a recent study in the Journal of Emergency Medicine conducted by researchers at the University of Maryland School of Medicine (UMSOM).
Critically ill patients who experience a sudden life-threatening condition like a stroke, ruptured aneurysm, or a massive pulmonary embolism (blood clot in the lung) are often first brought to the emergency department of the closest hospital and then transferred to a larger institution if their condition is deemed to be beyond the scope of the hospital’s level of care. The process of evaluating and transferring these patients, however, is generally ad hoc and fragmented, which results in delays of patients getting time-sensitive care that could save their lives or prevent permanent disability.
To improve access to care for critically ill patients, the R Adams Cowley Shock Trauma Center, University of Maryland, in conjunction with the Program in Trauma at UMSOM, established the CCRU in 2013 as the first critical care resuscitation unit in the nation. The recent study demonstrated for the first time that utilization of the CCRU not only helped double the number of transferred patients from other hospitals’ emergency departments, but also led to faster access to critical care resources and definitive surgical treatment, which decreased a patient’s risk of dying from their illness.
 “We have provided an important validation of the CCRU model, showing that it significantly improves patient outcomes,” said Quincy Tran, MD, PhD, Assistant Professor of Emergency Medicine at UMSOM who led the study. “Now that we have the data on the lifesaving potential of the CCRU, we hope to see other hospitals creating similar models.”
“We have provided an important validation of the CCRU model, showing that it significantly improves patient outcomes,” said Quincy Tran, MD, PhD, Assistant Professor of Emergency Medicine at UMSOM who led the study. “Now that we have the data on the lifesaving potential of the CCRU, we hope to see other hospitals creating similar models.”
The study analyzed medical records from 1565 critically ill patients with 644 treated in the CCRU during the first year of its operation in 2013. The rest served as control groups who were transferred directly from other hospitals’ emergency department to traditional intensive care units at UMMC during the year 2012 before the CCRU opened, and the year 2013 after the CCRU was opened.
The researchers found that the average time to get into an intensive care unit after a transfer request was filed was 108 minutes for CCRU patients, compared to 158 minutes for the control group of patients who were transferred and treated in 2012 before the CCRU opened, and 185 minutes for those in 2013. CCRU patients requiring emergency surgery received that surgery about 3.5 hours on average after they arrived at UMMC compared to 6 to 7 hours after arrival for those in the control group.
After controlling for variations in the severity of disease and care, the researchers found that the CCRU patients were 36 percent more likely to survive than those in the control group, which was a statistically significant finding.
 “The CCRU is modeled after the highly-effective Trauma Resuscitation Unit at the R Adams Cowley Shock Trauma Center. It relies on efficient communication and consultation with referring facilities and intra-hospital transport providers in order to facilitate prompt transfer of patients requiring specialized care to the University of Maryland Medical Center,” said co-author Daniel Haase, MD, Assistant Professor of Emergency Medicine at UMSOM, and Medical Director of the CCRU. “Our job is to collaborate with our specialists to deliver immediate resuscitation of patients with time-sensitive emergencies.”
“The CCRU is modeled after the highly-effective Trauma Resuscitation Unit at the R Adams Cowley Shock Trauma Center. It relies on efficient communication and consultation with referring facilities and intra-hospital transport providers in order to facilitate prompt transfer of patients requiring specialized care to the University of Maryland Medical Center,” said co-author Daniel Haase, MD, Assistant Professor of Emergency Medicine at UMSOM, and Medical Director of the CCRU. “Our job is to collaborate with our specialists to deliver immediate resuscitation of patients with time-sensitive emergencies.”
Procedures performed in the CCRU include massive blood transfusions, continuous renal replacement therapy (dialysis) for patients with malfunctioning kidneys, continuous EEG monitoring of the brain, and organ support with a heart-lung machine.
 “We are leading the way in critical care medicine by having the first dedicated Critical Care Resuscitation Unit in the nation,” said UMSOM Dean E. Albert Reece, MD, PhD, MBA, University Executive Vice President for Medical Affairs and the John Z. and Akiko K. Bowers Distinguished Professor. “Having the data to demonstrate improved patient outcomes will hopefully convince other hospitals to consider adopting this model of care.”
“We are leading the way in critical care medicine by having the first dedicated Critical Care Resuscitation Unit in the nation,” said UMSOM Dean E. Albert Reece, MD, PhD, MBA, University Executive Vice President for Medical Affairs and the John Z. and Akiko K. Bowers Distinguished Professor. “Having the data to demonstrate improved patient outcomes will hopefully convince other hospitals to consider adopting this model of care.”
About the University of Maryland School of Medicine
Now in its third century, the University of Maryland School of Medicine was chartered in 1807 as the first public medical school in the United States. It continues today as one of the fastest growing, top-tier biomedical research enterprises in the world -- with 45 academic departments, centers, institutes, and programs; and a faculty of more than 3,000 physicians, scientists, and allied health professionals, including members of the National Academy of Medicine and the National Academy of Sciences, and a distinguished two-time winner of the Albert E. Lasker Award in Medical Research. With an operating budget of more than $1.2 billion, the School of Medicine works closely in partnership with the University of Maryland Medical Center and Medical System to provide research-intensive, academic and clinically based care for nearly 2 million patients each year. The School of Medicine has more than $540 million in extramural funding, with most of its academic departments highly ranked among all medical schools in the nation in research funding. As one of the seven professional schools that make up the University of Maryland, Baltimore campus, the School of Medicine has a total population of nearly 9,000 faculty and staff, including 2,500 student trainees, residents, and fellows. The combined School of Medicine and Medical System (“University of Maryland Medicine”) has an annual budget of nearly $6 billion and an economic impact more than $15 billion on the state and local community. The School of Medicine faculty, which ranks as the 8th highest among public medical schools in research productivity, is an innovator in translational medicine, with 600 active patents and 24 start-up companies. The School of Medicine works locally, nationally, and globally, with research and treatment facilities in 36 countries around the world. Visit medschool.umaryland.edu
About the University of Maryland Medical Center
The University of Maryland Medical Center (UMMC) is comprised of two hospital campuses in Baltimore: the 800-bed flagship institution of the 14-hospital University of Maryland Medical System (UMMS) — and the 200-bed UMMC Midtown Campus, both academic medical centers training physicians and health professionals and pursuing research and innovation to improve health. UMMC’s downtown campus is a national and regional referral center for trauma, cancer care, neurosciences, advanced cardiovascular care, women's and children's health, and has one of the largest solid organ transplant programs in the country. All physicians on staff at the downtown campus are clinical faculty physicians of the University of Maryland School of Medicine. The UMMC Midtown Campus medical staff is predominately faculty physicians specializing in diabetes, chronic diseases, behavioral health, long term acute care and an array of outpatient primary care and specialty services. UMMC Midtown has been a teaching hospital for 140 years and is located one mile away from the downtown campus. For more information, visit www.umm.edu.
Contact
Office of Public Affairs
655 West Baltimore Street
Bressler Research Building 14-002
Baltimore, Maryland 21201-1559
Contact Media Relations
(410) 706-5260
Deborah Kotz
Director of Media Relations
Office of Public Affairs & Communications
University of Maryland School of Medicine
o: 410-706-4255
c: 410-804-0054
t: @debkotz2
Related stories

Friday, December 19, 2025
Sharon M. Henry, MD, Appointed First Vice President-Elect of the American College of Surgeons
Sharon M. Henry, MD, FACS, the Anne Scalea Professor of Trauma Surgery at the University of Maryland School of Medicine (UMSOM) and Director of the Division of Wound Healing and Metabolism at the R Adams Cowley Shock Trauma Center, has been elected First Vice President-Elect of the American College of Surgeons (ACS). The historic election, which took place on October 7 at the ACS Clinical Congress, marks the first time a Black woman has been appointed to this leadership position in the organization’s history.

Friday, May 17, 2024
Gov. Moore Signs Significant Funding Bills Securing the Future of Trauma Care for Marylanders
Dozens of Shock Trauma team members, trauma survivors, and supporters traveled to the state capital yesterday to support Maryland Governor Wes Moore, Senate President Bill Ferguson, and House Speaker Adrienne Jones as they signed a consequential bill into law expanding annual funding for Maryland’s renowned statewide trauma system. It will ensure access to world-class trauma care for Marylanders well into to the future.

Wednesday, October 26, 2016
Researchers Develop System to Classify Gunshot Wounds and Other Similar Injuries to the Head
Every year, more than 32,000 Americans die from gunshot wounds. A significant proportion of these deaths involve head wounds. Despite this massive public health burden, researchers know little about the variables that determine whether a victim of these injuries will live or die.
