UM School of Medicine Researcher Warns of Need for Malaria Drug to Treat Severe Cases in U.S.
August 19, 2019 | Joanne Morrison

Increased Global Travel Gives Rise to U.S.-Based Malaria Cases and Need for Better Access to Intravenous Treatment
Each year there are more than 200 million cases of malaria worldwide, a mosquito-borne disease caused by a parasite that brings on fever and body aches and, in some cases, more serious conditions such as coma and death. While the vast majority of these cases occur in sub-Saharan Africa and South Asia, the U.S. each year sees more than 1,500 cases, and currently there is limited access to an intravenously-administered (IV) drug needed for the more serious cases, according to a top malaria researcher at the University of Maryland School Medicine (UMSOM).
Treatment for severe malaria cases is an intravenous-administered (IV) form of quinidine gluconate. However, there is no longer a widely available supply of this drug in IV form in the United States, warned Mark Travassos, MD, MSc, Assistant Professor of Pediatrics at UMSOM and scientist at the Center for Vaccine Development and Global Health (CVD), in a commentary published in Annals of Internal Medicine today. Oral doses of quinidine are available, but they are not typically effective in more serious malaria cases, he said.
“Severe malaria is a medical emergency that requires immediate treatment with IV medication to reduce the risk of death,” said Dr. Travassos, a pediatric infectious diseases specialist and malaria expert in UMSOM’s Malaria Research Program within the CVD. Dr. Travassos cited 2015 Centers for Disease Control and Prevention (CDC) statistics showing more than 1,500 malaria cases in the U.S., of which 259 were serious and needed IV treatment. Now, with increased global interconnectedness, the rate of U.S. malaria cases is indeed rising steadily over the past 40 years, according to the CDC.
Dr. Travassos notes that while oral treatments for malaria are available in the U.S., often times these are not effective in more serious cases. “Severe malaria patients can have brain involvement or repeated vomiting and may not tolerate oral medication, placing them at high risk for complications,” said Dr. Travassos.
Since 1991, quinidine has been the only Food and Drug Administration-approved (FDA) treatment for severe malaria. However, since April of 2019, remaining supplies of IV-administered quinidine have expired, leaving U.S. physicians with no readily available treatment.
Without a broad supply of the IV drug, physicians treating serious malaria cases must on a case-by-case basis request IV artesunate, a non-FDA-approved drug for severe malaria that is only available from the CDC at ten different airports in the U.S. The CDC will then ship the drug to the airport closest to a requesting hospital. Delivery times will take on average eight hours, but they could be as long as 24 hours.
“This plan raises serious concerns,” said Dr. Travassos, adding that the CDC’s recommendation that a physician treat a patient with oral medication while waiting for IV treatment to arrive does not meet the standard of care for severe malaria and will not reduce parasite replication in the blood as rapidly as an effective intravenous medication.
 “Malaria is a leading killer worldwide, impacting millions of people each year. While we continue to work on developing vaccines and other treatments, it is critical that patients everywhere have access to the regimens needed to combat this disease,” said Kathleen Neuzil, MD, MPH, Professor of Medicine and Pediatrics and Director of the CVD.
“Malaria is a leading killer worldwide, impacting millions of people each year. While we continue to work on developing vaccines and other treatments, it is critical that patients everywhere have access to the regimens needed to combat this disease,” said Kathleen Neuzil, MD, MPH, Professor of Medicine and Pediatrics and Director of the CVD.
Federal agencies and professional societies need to work to remedy this situation, Dr. Travassos recommended in his commentary. The CDC should identify potential pharmaceutical companies for manufacture of IV form of artesunate and evaluate the need for incentives, Dr. Travassos recommended. He added that a priority review of a new drug application for IV artesunate would reduce the time for FDA approval to as little as six months. He further cautioned that given the shortage of IV treatments for the most serious malaria cases, hospitals in the U.S. should develop a preparedness plan.
At the hospital level, a plan should address potential delays in diagnosis and treatment of malaria, with anticipation of different scenarios. At triage, patients should be questioned about recent travel outside the country. Those who are febrile and have recently traveled to malaria-endemic regions should immediately have a rapid diagnostic test for malaria, and a thick and thin blood smear should be sent for an immediate reading, Dr. Travassos recommended.
 “As we become more connected globally in the U.S., it is important to understand the risks and concerns of diseases like malaria. At the University of Maryland School of Medicine, our scientists and physician-scientists are studying the best treatments and approaches for managing and treating the most complex and challenging diseases,” said UMSOM Dean E. Albert Reece, MD, PhD, MBA, who is also the Executive Vice President for Medical Affairs, University of Maryland and the John Z. and Akiko K. Bowers Distinguished Professor.
“As we become more connected globally in the U.S., it is important to understand the risks and concerns of diseases like malaria. At the University of Maryland School of Medicine, our scientists and physician-scientists are studying the best treatments and approaches for managing and treating the most complex and challenging diseases,” said UMSOM Dean E. Albert Reece, MD, PhD, MBA, who is also the Executive Vice President for Medical Affairs, University of Maryland and the John Z. and Akiko K. Bowers Distinguished Professor.
About the University of Maryland School of Medicine
Now in its third century, the University of Maryland School of Medicine was chartered in 1807 as the first public medical school in the United States. It continues today as one of the fastest growing, top-tier biomedical research enterprises in the world, with 43 academic departments, centers, institutes, and programs. The School of Medicine has a faculty of more than 3,000 physicians, scientists, and allied health professionals, including members of the National Academy of Medicine and the National Academy of Sciences, and a distinguished recipient of the Albert E. Lasker Award in Medical Research. With an operating budget of more than $1.2 billion, the School of Medicine works closely in partnership with the University of Maryland Medical Center and Medical System to provide research-intensive, academic and clinically based care for more than 1.2 million patients each year. The School has over 2,500 students, residents, and fellows, and nearly $575 million in extramural funding, with most of its academic departments highly ranked among all medical schools in the nation in research funding. As one of the seven professional schools that make up the University of Maryland, Baltimore campus, the School of Medicine has a total workforce of nearly 7,000 individuals. The combined School and Medical System (“University of Maryland Medicine”) has an annual budget of over $6 billion and an economic impact of more than $15 billion on the state and local community. The School of Medicine faculty, which ranks as the 8th highest among public medical schools in research productivity, is an innovator in translational medicine, with 600 active patents and 24 start-up companies. The School works locally, nationally, and globally, with research and treatment facilities in 36 countries around the world. Visit medschool.umaryland.edu
Contact
Department of Anesthesiology
(410) 328-6120 (phone)
(410) 328-5531 (fax)
swalsh@som.umaryland.edu
Joanne Morrison
Director of Marketing and Public Relations
Center for Vaccine Development and Global Health
University of Maryland School of Medicine
jmorrison@som.umaryland.edu
Office: (410) 706-2884
Mobile: (202) 841-3369
Related stories

Tuesday, May 21, 2024
University of Maryland School of Medicine Launches Vaccine Development Program to Prevent Sepsis in Newborns
University of Maryland School of Medicine (UMSOM) researchers at the Center for Vaccine Development and Global Health (CVD) have been awarded up to $3.96 million over three years to develop and test a vaccine in an animal model that could eventually be used in pregnant women to prevent sepsis in newborns and infants.

Thursday, March 28, 2024
NIH selects Dr. Kathleen Neuzil as Director of The Fogarty International Center
Kathleen M. Neuzil, MD, MPH, Director of the University of Maryland School of Medicine’s (UMSOM) Center for Vaccine Development and Global Health, has been named the 13th director of the Fogarty International Center (FIC), which is part of the National Institutes of Health (NIH). Dr. Neuzil will be the first woman to hold the permanent directorship since the center’s founding in 1968 and will also hold the position of Associate Director for International Research at NIH.

Tuesday, December 20, 2022
COVID Vaccines Prevented 3 Million Deaths in the U.S., New Analysis Finds
In the two years since the first COVID-19 vaccines were given to patients in the U.S., the vaccines had the cumulative effect of preventing 18 million hospitalizations and 3 million deaths. That is based on a new modeling analysis conducted by a researcher at the University of Maryland School of Medicine (UMSOM) and her colleagues. Results of the analysis were published by the Commonwealth Fund.
Monday, July 18, 2022
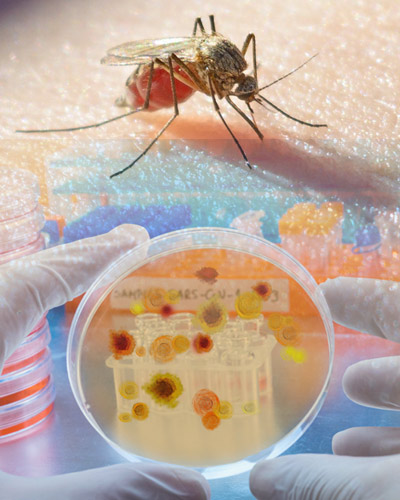
New Genomic Research Shows Why Testing Malaria Vaccines in the Clinic is as Rigorous as Natural Exposure in the Field
Malaria is the deadliest mosquito-borne parasitic infection of humans. In 2021, after a century of research, the World Health Organization (WHO) approved the world’s first malaria vaccine. That vaccine reduces the incidence of malaria infections in young children aged 5-17 months by only 30 percent, meaning that it remains critical to continue developing and testing more effective vaccines.

Wednesday, January 26, 2022
Trial Co-led by University of Maryland School of Medicine Scientist Confirms Safety of “Mix-and-Match” COVID-19 Vaccine Booster Dosing
A University of Maryland School of Medicine (UMSOM), Center for Vaccine Development and Global Health (CVD), expert is co-leading an ongoing study that was pivotal in recommending adults and teens receive booster COVID-19 shots of their choosing starting in fall 2021. The preliminary clinical trial results, reported today in The New England Journal of Medicine, found that is safe and effective to receive boosters that are the same or a different one from the person’s primary vaccine(s).

Friday, February 05, 2021
UM School of Medicine Researchers Demonstrate Strong Immune Response for New COVID-19 Vaccine in Pre-Clinical Tests
Researchers at the University of Maryland School of Medicine (UMSOM) have found promising results in pre-clinical studies for a new experimental vaccine against COVID-19 made by Novavax. The vaccine was found to generate a robust immune response in animals exposed to the vaccine with strong data indicating safety and efficacy, according to the study published recently in the journal Nature Communications. The results have been used to begin testing the vaccine in human trials in the U.S. with a Phase 3 trial that recently launched at the UMSOM’s Center for Vaccine Development and Global Health.

Thursday, January 30, 2020
UMSOM Pediatric Infectious Disease Experts Sound Alarm Over Risk of Outbreaks in U.S. Border Detention Centers
Over the past year, at least seven children have died from diseases including influenza while being detained by the U.S. Department of Homeland Security’s Customs and Border Protection (CBP) agency. Infectious disease experts at the University of Maryland School of Medicine (UMSOM) called for protections like influenza vaccinations to prevent serious outbreaks.

Tuesday, December 10, 2019
UMSOM Researchers to Test Vaccine Designed to Protect Against Serious Illness from Contaminated Food and Water
Each year, millions of people contract serious diarrheal illnesses typically from contaminated food and water. Among the biggest causes of diarrheal diseases are the bacteria Shigella and enterotoxigenic Escherichia coli (ETEC), and researchers at the University of Maryland School of Medicine are testing a vaccine designed to offer protection against these serious pathogens.

Wednesday, October 30, 2019
UM School of Medicine's Myron M. Levine, MD, DTPH, to Receive Prestigious Lifetime Award for Five Decades of Pioneering Vaccine Research
Myron M. Levine, MD, DTPH, the Simon and Bessie Grollman Distinguished Professor at the University of Maryland School of Medicine (UMSOM), Associate Dean for Global Health, Vaccinology and Infectious Diseases, and Founder and Former Director of the Center for Vaccine Development and Global Health (CVD) is a co-recipient of the 2020 Research! America Geoffrey Beene Foundation Builders of Science Award for his pioneering vaccine and infectious disease research.

Monday, October 21, 2019
UM School of Medicine's Kathleen M Neuzil Elected as Member of Prestigious National Academy of Medicine
Kathleen M. Neuzil, MD, MPH, Professor of Medicine and Pediatrics and Director of the Center for Vaccine Development and Global Health (CVD) at the University of Maryland School of Medicine (UMSOM), has been elected as a member of the National Academy of Medicine (NAM), in recognition of her pivotal research that has informed and shaped global vaccine and public health policy. Her membership was announced at the annual NAM meeting in Washington, D.C., placing her among the 2,178 U.S. members of this important organization. Membership in the Academy is considered one of the highest honors for individuals who have made major contributions to the advancement of the medical sciences, health care and public health.

Friday, September 20, 2019
UM School of Medicine's Center for Vaccine Development and Global Health Receives NIH Contract of up to More than $200 Million for Influenza Research
Kathleen Neuzil, MD, MPH, Professor of Medicine and Pediatrics and Director of the Center for Vaccine Development and Global Health (CVD) at the University of Maryland School of Medicine (UMSOM) and Dean E. Albert Reece, MD, PhD, MBA, announced that CVD has been awarded a contract from the National Institute of Allergy and Infectious Diseases (NIAID), with total funding up to more than $200 million over seven years if all contract options are exercised.

Tuesday, August 13, 2019
UM School of Medicine Researchers Begin Phase 1 Clinical Trial of Vaccine Against Mosquito-Borne Diseases
Mosquito-borne diseases including malaria, dengue and yellow fever, have a severe impact resulting in millions of deaths worldwide, hitting the world’s most vulnerable populations the hardest. Researchers at the University of Maryland School of Medicine (UMSOM) have begun testing an experimental vaccine that is designed to protect against a series of these diseases.
Wednesday, July 17, 2019
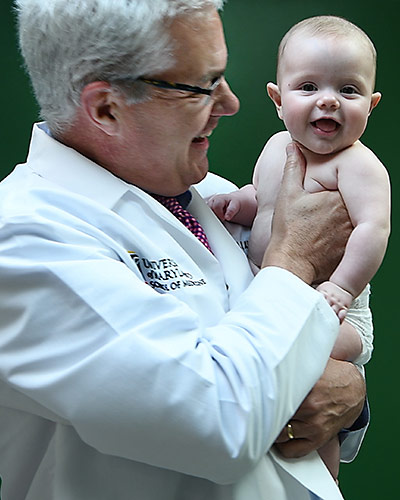
Vaccines Tested in UM School of Medicine’s Center for Vaccine Development Protect Children Around the World
For 30 years, the Center for Vaccine Development and Global Health (CVD) at the University of Maryland School of Medicine (UMSOM) has collaborated with the Pediatric Center of Frederick to test vaccines used in pediatric care.
Friday, March 08, 2019
UMSOM Researchers Unveil Progress and Challenges in Introducing Typhoid Conjugate Vaccine in Sub-Saharan Africa and Asia
Each year there are nearly 11 million cases of typhoid, a disease that is spread through contaminated food, drink and water. Researchers at the University of Maryland School of Medicine are leading an international consortium that is studying the impact of a typhoid conjugate vaccine (TCV) in an effort to accelerate introduction of the vaccine in countries in sub-Saharan Africa and Asia where there is a high burden of typhoid.

Wednesday, December 26, 2018
Multicenter Trial Supports Use of Topical Antibiotic as a Tool to Eliminate Staph Colonization in NICU Babies
A team of doctors led by Karen L. Kotloff, M.D., University of Maryland School of Medicine (UMSOM), Center for Vaccine Development and Global Health (CVD), has performed a clinical trial involving multiple hospitals that tested the effectiveness of applying a topical antibiotic known as mupirocin for prevention of Staphylococcus aureus (SA) infection in babies in the neonatal intensive care unit (NICU). This study was published in the journal Pediatrics.

Thursday, December 20, 2018
Data From Largest Global Diarrheal Disease Study Available to Scientists on Public Sites
Data collected from the Global Enteric Multicenter Study (GEMS), a multi-site research project studying diarrheal diseases that was designed and coordinated by researchers in the Center for Vaccine Development and Global Health (CVD) at the University of Maryland School of Medicine (UMSOM), are now available to scientists on two online data resources.
Monday, December 03, 2018
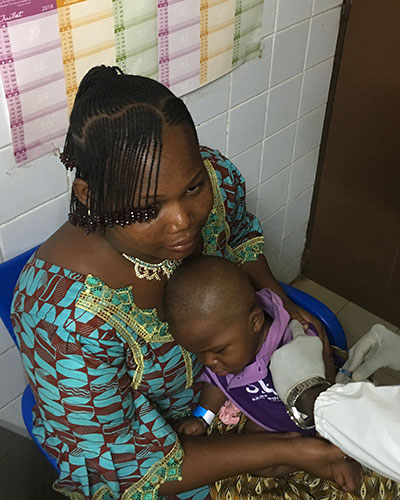
UMSOM and Groupe De Recherche Action En Sante Begin Second Typhoid Conjugate Vaccine Study in Africa
A new study has been launched in Burkina Faso for Bharat Biotech’s typhoid conjugate vaccine (TCV). It is the second clinical study underway in Africa for the vaccine and the first in West Africa. The vaccine study is a joint effort by the Center for Vaccine Development and Global Health (CVD) at the University of Maryland School of Medicine, (UMSOM) and Groupe de Recherche Action en Santé (GRAS) in Burkina Faso.

Friday, November 02, 2018
UMSOM Global Health Expert Named to Prestigious World Health Organization Immunization Panel
Kathleen Neuzil, MD, MPH, Professor of Medicine and Pediatrics and Director of the Center for Vaccine Development and Global Health (CVD) at the University of Maryland School of Medicine (UMSOM), has been named to the World Health Organization’s (WHO) Strategic Advisory Group of Experts (SAGE) on Immunization.

Sunday, October 28, 2018
American Society of Tropical Medicine & Hygiene Awards Dr. Miriam Laufer the LePrince Medal for Malaria Research
Miriam Laufer, MD, MPH, Professor of Pediatrics and Associate Director for Malaria Research at the University of Maryland School of Medicine’s (UMSOM) Center for Vaccine Development and Global Health (CVD), was awarded the Joseph Augustin LePrince Medal by the American Society of Tropical Medicine and Hygiene (ASTMH).

Wednesday, June 06, 2018
UMSOM Researchers Find that Silent Carriers of Malaria are Unlikely to Develop the Disease
In regions where malaria illness is widespread, it is common to find many individuals who are infected with malaria parasites (Plasmodium falciparum), but without symptoms. New research conducted by the University of Maryland School of Medicine (UMSOM) shows that treating these silent malaria cases could help stop the spread of malaria to others.

Tuesday, May 15, 2018
Tackling Malaria Transmission in Sub-Saharan Africa
Two malaria experts in the Center for Vaccine Development and Global Health at the University of Maryland School of Medicine wrote a commentary published in the June Issue of The Lancet Global Health discussing the prevalence of malaria in school-age children in sub-Saharan Africa. Miriam Laufer, MD, Associate Professor of Pediatrics and Associate Director for Malaria Research CVD, and Lauren Cohee, MD, Instructor, Pediatrics, noted that often malaria infection is more common in school-age children than younger children and adults.
