Researchers Develop System to Classify Gunshot Wounds and Other Similar Injuries to the Head
October 26, 2016

Study Will Help Doctors Better Understand How To Improve Survival From These Injuries
Every year, more than 32,000 Americans die from gunshot wounds. A significant proportion of these deaths involve head wounds. Despite this massive public health burden, researchers know little about the variables that determine whether a victim of these injuries will live or die.
Now, for the first time ever, researchers at the University of Maryland School of Medicine (UM SOM) have developed a system to help answer this question. The system has created a way to better understand the variables involved in survival from these wounds. The paper appears in the latest issue of the journal Neurology.
"This kind of analysis has never been done before," said one of the study’s principal authors, Thomas M. Scalea, MD, FACS, MCCM, the Honorable Francis X. Kelly Distinguished Professor of Trauma Surgery, Director, Program in Trauma, and Physician-in-Chief, R Adams Cowley Shock Trauma Center. "Using this knowledge, we can improve treatments and focus our care to maximize survival chances."
 The study was a partnership between scientists at UM SOM and researchers at the University of Massachusetts Medical School, Massachusetts General Hospital and Brigham & Women’s Hospital, Harvard Medical School and Yale University. Besides Dr. Scalea, the other UM SOM researcher was Deborah M. Stein, MD, MPH, FACS, FCCM, R Adams Cowley Professor in Shock & Trauma, University of Maryland School of Medicine, Chief of Trauma and Director of Neurotrauma Critical Care.
The study was a partnership between scientists at UM SOM and researchers at the University of Massachusetts Medical School, Massachusetts General Hospital and Brigham & Women’s Hospital, Harvard Medical School and Yale University. Besides Dr. Scalea, the other UM SOM researcher was Deborah M. Stein, MD, MPH, FACS, FCCM, R Adams Cowley Professor in Shock & Trauma, University of Maryland School of Medicine, Chief of Trauma and Director of Neurotrauma Critical Care.
The researchers looked at 413 patients, most whom were treated at the Shock Trauma Center. All of the patients had penetrating brain injuries, 93 percent of them from gunshot wounds. Of the overall group, 42 percent, 175 in total, survived. The researchers looked at a range of variables to see which seemed to correlate with survival.
 One key variable appears to be the level of consciousness upon arrival. The researchers used a measure known as the Glasgow Coma Scale (GCS), which tracks patient awareness after injury. The higher the score, the more aware the person is. The study found that patients with a lower GCS score were significantly less likely to survive. This was particularly true for movement – patients who were not moving after injury had a higher risk of death.
One key variable appears to be the level of consciousness upon arrival. The researchers used a measure known as the Glasgow Coma Scale (GCS), which tracks patient awareness after injury. The higher the score, the more aware the person is. The study found that patients with a lower GCS score were significantly less likely to survive. This was particularly true for movement – patients who were not moving after injury had a higher risk of death.
Another key measure appears to be pupillary reactivity, the ability of the eye’s pupils to change diameter in response to light. This is a measure of the nervous system’s basic functioning. In patients with low or absent pupillary reactivity, survival rates were significantly lower. Also crucial was Injury Severity Score (ISS), a measure of overall bodily trauma. The higher the ISS, the lower the survival rate.
The study also found that having only a single penetrating brain injury, rather than multiple penetrating brain injuries, was associated with 87 percent higher odds for survival.
Interestingly, female patients had 76 percent higher odds for survival than men. The reason for this is not clear. The researchers note that progesterone, a hormone that tends to be higher in women than in men, may have a protective effect in these injuries. The overwhelming majority of the subjects in the study, however, were men: women made up only 13 percent of the subjects in the study.
“Gunshot wounds and other penetrating brain injuries are a severe public health problem,” said UM SOM Dean E. Albert Reece, MD, PhD, MBA, who is also vice president for medical affairs at the University of Maryland and the John Z. and Akiko K. Bowers Distinguished Professor. “This groundbreaking research points the way to better understanding who is most at risk of death from these events, and how we can improve our treatment.”
About the University of Maryland School of Medicine
The University of Maryland School of Medicine was chartered in 1807 and is the first public medical school in the United States and continues today as an innovative leader in accelerating innovation and discovery in medicine. The School of Medicine is the founding school of the University of Maryland and is an integral part of the 11-campus University System of Maryland. Located on the University of Maryland’s Baltimore campus, the School of Medicine works closely with the University of Maryland Medical Center and Medical System to provide a research-intensive, academic and clinically based education. With 43 academic departments, centers and institutes and a faculty of more than 3,000 physicians and research scientists plus more than $400 million in extramural funding, the School is regarded as one of the leading biomedical research institutions in the U.S. with top-tier faculty and programs in cancer, brain science, surgery and transplantation, trauma and emergency medicine, vaccine development and human genomics, among other centers of excellence. The School is not only concerned with the health of the citizens of Maryland and the nation, but also has a global presence, with research and treatment facilities in more than 35 countries around the world.
Contact
Office of Public Affairs
655 West Baltimore Street
Bressler Research Building 14-002
Baltimore, Maryland 21201-1559
Contact Media Relations
(410) 706-5260
Related stories

Friday, December 19, 2025
Sharon M. Henry, MD, Appointed First Vice President-Elect of the American College of Surgeons
Sharon M. Henry, MD, FACS, the Anne Scalea Professor of Trauma Surgery at the University of Maryland School of Medicine (UMSOM) and Director of the Division of Wound Healing and Metabolism at the R Adams Cowley Shock Trauma Center, has been elected First Vice President-Elect of the American College of Surgeons (ACS). The historic election, which took place on October 7 at the ACS Clinical Congress, marks the first time a Black woman has been appointed to this leadership position in the organization’s history.

Monday, August 04, 2025
New Review Highlights Significant Need for Comprehensive Care for Gun Violence Survivors
A new review article published in JAMA underscores the critical need for comprehensive long-term medical care for patients treated for firearm injuries, which has become an epidemic in the U.S. fueled by years of rising gun violence. More than 48,000 people died of firearm injuries in the U.S. in 2022, according to the Centers for Disease Control and Prevention with 120,000 suffering from gunshot wounds that they recover from.

Friday, May 17, 2024
Gov. Moore Signs Significant Funding Bills Securing the Future of Trauma Care for Marylanders
Dozens of Shock Trauma team members, trauma survivors, and supporters traveled to the state capital yesterday to support Maryland Governor Wes Moore, Senate President Bill Ferguson, and House Speaker Adrienne Jones as they signed a consequential bill into law expanding annual funding for Maryland’s renowned statewide trauma system. It will ensure access to world-class trauma care for Marylanders well into to the future.

Wednesday, December 13, 2023
UM School of Medicine Awarded Up to $7.3M from DARPA to Drive Innovation in Trauma Triage Technology, Improve Mass Casualty Response Efforts
In an effort to better optimize the triage of patients during mass casualty events, University of Maryland School of Medicine (UMSOM) researchers are receiving up to $7.3 million in funding from the Defense Advanced Research Project Agency (DARPA) for vital new research. The funding will be used to support a study that will collect data over the next 3.5 years on trauma patients with the aim of identifying and implementing lifesaving advancements in medical triage for large-scale mass casualty incidents.

Wednesday, July 20, 2022
University of Maryland School of Medicine Faculty Member Featured on NBC Nightly News Special Report on Gun Violence in America
A University of Maryland School of Medicine (UMSOM) faculty member was featured in a prestigious national news program over the weekend highlighting the lifesaving critical care medicine practiced at the R Adams Cowley Shock Trauma Center at the University of Maryland Medical Center (UMMC). In an extended segment called “One Night in America” that comprised half of the evening newscast for NBC Nightly News and additional coverage on MSNBC, a reporter was embedded in the trauma center from Saturday evening, July 16, into Sunday morning to document emergency trauma cases caused by gun violence. Reporters were also embedded in three other major cities showing different perspectives including police response to shootings and community support from a local street pastor.

Wednesday, January 19, 2022
World-Renowned University of Maryland School of Medicine Trauma Surgeon and Physician-Scientist Celebrates 25th Anniversary
As the Honorable Francis X. Kelly Distinguished Professor of Trauma Surgery and Director of the Program in Trauma at the University of Maryland School of Medicine (UMSOM) and Physician-in-Chief of the R Adams Cowley Shock Trauma Center at the University of Maryland Medical Center (UMMC), Thomas M. Scalea, MD, FACS, MCCM, has pioneered advances to trauma care for patients in the United States and around the world. He has cared for tens of thousands of Marylanders critically injured in motor vehicle collisions, falls and violent attacks, traveled to China and Haiti to render assistance to earthquake victims, helped train thousands of U.S. Air Force personnel and worked alongside military physicians in war-torn Afghanistan. He has steered Maryland’s highest-level trauma center through two years of the COVID-19 pandemic.

Thursday, August 06, 2020
Philanthropist and Real Estate Developer, Howard S. Brown Makes $2.5 Million Gift to UMSOM in Honor of Renowned Trauma Surgeon and Leader, Thomas M. Scalea, MD
Mr. Brown’s Gift Memorializes his Daughter, Esther Ann Brown Adler, and Establishes the Thomas M. Scalea, MD Endowed Distinguished Professorship in Trauma Surgery

Tuesday, July 21, 2020
University of Maryland School of Medicine Names Renowned Trauma Surgeon-Scientist, Dr. David Efron, as Professor of Trauma Surgery and New Chief of Trauma
Thomas M. Scalea, MD, the Honorable Francis X. Kelly Distinguished Professor of Trauma Surgery and Director of the Program in Trauma at the University of Maryland School of Medicine (UMSOM), and Physician-in-Chief at the UM R Adams Cowley Shock Trauma Center, along with UMSOM Dean, E. Albert Reece, MD, PhD, MBA, announced today that David Thomas Efron, MD, one of the leading trauma surgeon-scientists in the U.S., will become the Inaugural Thomas M. Scalea Distinguished Professor of Trauma Surgery in the Department of Surgery, Chief of Trauma and Medical Director of the R. Adams Cowley Shock Trauma Center. He will begin his new position effective September 1.
Monday, January 13, 2020
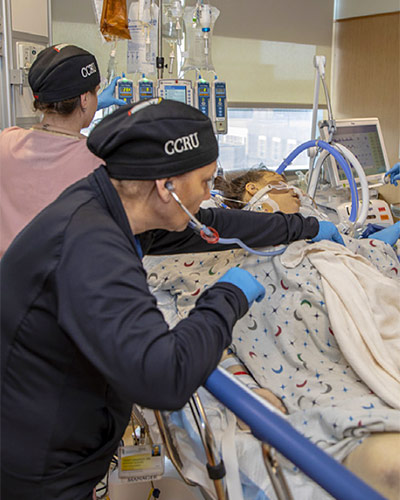
University of Maryland Medicine's Novel Critical Care Resuscitation Unit Improves Patients' Chances of Survival, Study Finds
Patients with acutely life-threatening health conditions who were treated in the innovative Critical Care Resuscitation Unit (CCRU) received faster treatment and had better health outcomes, including a 36 percent lower risk of dying than those who were transferred from a hospital’s emergency department then evaluated and treated in a traditional intensive care unit, according to a recent study in the Journal of Emergency Medicine conducted by researchers at the University of Maryland School of Medicine (UMSOM).

Tuesday, October 16, 2018
UMSOM Faculty Members Named 2018 “Top Docs” by Baltimore Magazine
More than 70 doctors who provide care to patients at the University of Maryland Medical Center Downtown and Midtown Campuses have been recognized as "Top Doctors" in the November 2018 issue of Baltimore magazine. All of the recognized physicians are also faculty members of the University of Maryland School of Medicine.

Monday, October 15, 2018
University of Maryland School of Medicine Scientists Receive Prestigious UMB Founders Week Awards
Several experts at the UMSOM received prestigious awards commemorating the UMB 2018 Founders Week. Among them, Karen Kotloff, MD, Professor of Pediatrics, was named "Researcher of the Year" for her extensive work in infectious diseases in the U.S. and developing countries. The MARS team – Steven I. Hanish, MD, Visiting Associate Professor of Surgery, Thomas M. Scalea, MD, FACS, FCCM, The Honorable Francis X. Kelly Distinguished Professor in Trauma Surgery, and Deborah Stein, MD, MPH, FACS, FCCM, The R Adams Cowley, MD Professor in Shock and Trauma– were named "Entrepreneurs of the Year" for their liver dialysis device called the Molecular Absorbent Recirculating System (MARS).

Friday, March 30, 2018
Stop the Bleed Team at Shock Trauma Center Trains Campus Leaders
The University of Maryland R Adams Cowley Shock Trauma Center provided special training today on methods to control bleeding as part of the “Stop the Bleed” campaign, a national effort to teach basic bleeding control.

Wednesday, January 04, 2017
Honoring a Hero: Dr. Thomas Scalea, Physician-in-Chief at the R Adams Cowley Shock Trauma Center, Marks 20 Years at the University of Maryland
Under his leadership, Shock Trauma has grown tremendously – from the construction of the cutting-edge Critical Care Tower to the expansion of hands-on training opportunities for physicians, nurses and medical students.

Thursday, September 08, 2016
Largest-Ever Study to Compare Medications to Prevent Life-Threatening Clots in Orthopaedic Trauma Patients
Is the blood thinner heparin the most effective option to reduce the risk of blood clots for fracture patients? A comprehensive new study involving 13,000 patients, led by researchers at the University of Maryland School of Medicine (UM SOM), will try to resolve this important question.

Thursday, May 26, 2016
Leading Surgeon Scientist and Trauma Chief Dr. Deborah Stein Invested as Inaugural R Adams Cowley Professor at the UM SOM
In a moving speech before a large audience recently at Westminster Hall, Deborah M. Stein, MD, MPH, newly invested as the R Adams Cowley, MD Professor in Shock and Trauma, used those words to reflect on her father’s influence and how proud he is to see the family’s legacy of healing continue. "Becoming a surgeon was all about my father -- I wanted to be him, and to heal with my hands, just as he had done."

Thursday, January 07, 2016
UM SOM Names Dr. Samuel Tisherman as Director of the Division of Critical Care and Trauma Education
Stephen T. Bartlett, MD, the Peter Angelos Distinguished Professor of Surgery and Chair, Department of Surgery at University of Maryland School of Medicine (UM SOM), and Executive Vice President and Surgeon in Chief for the University of Maryland Medical System, and Thomas M. Scalea, MD, FACS, the Honorable Francis X. Kelly Distinguished Professor of Trauma Surgery at UM SOM, in conjunction with Dean E. Albert Reece, MD, PhD, MBA, announced today that Samuel A. Tisherman, MD, FACS, FCCM, has been appointed as the Director of the Division of Critical Care and Trauma Education at the Program in Trauma at UM SOM.

Monday, January 04, 2016
R Adams Cowley Shock Trauma Center at the University of Maryland Showcased in Discovery Life Series - Shock Trauma: Edge of Life
Discovery Life’s new unscripted docudrama series Shock Trauma: Edge of Life follows a team of medical professionals at the world-renown University of Maryland R Adams Cowley Shock Trauma Center (“Shock Trauma” UM School of Medicine (SOM) faculty physicians and trauma surgeons, alongside University of Maryland Medical Center (UMMC) residents, fellows, nurses, patient care technicians, and an array of specialists, perform lifesaving medical care in the first and highest volume trauma center of its kind in the United States.
