Surgical First: Patient Avoids Dialysis Thanks to Simultaneous Polycystic Kidney Removal and Kidney Transplant During 28-Person Kidney Swap
June 24, 2016

Complex Procedure Coordinated in Conjunction with National Kidney Registry
In a first-of-its-kind procedure in the United States, a patient was able to avoid dialysis when surgeons simultaneously removed two diseased kidneys and also transplanted a kidney from a living donor – all as part of a 28-person paired kidney exchange (PKE). The procedure, performed in May on a patient with polycystic kidney disease (PKD), eliminated the need for the patient to ever undergo dialysis.
“We worked closely with the National Kidney Registry, which coordinated the 28-person swap that led to a compatible living donor for our patient,” says David B. Leeser, MD, associate professor of surgery at the University of Maryland School of Medicine (UM SOM) and chief of kidney and pancreas transplant at the University of Maryland Medical Center (UMMC), who developed the plan. “On the day of the transplant, we removed our patient’s two large kidneys, weighing 10 pounds each, precisely timing our procedure with the hospital that was providing the donor kidney, so our patient was able to avoid dialysis.”
The recipient’s wife was unable to donate a kidney to her husband, due to incompatible blood types. Because kidneys from living donors have better outcomes than those from deceased donors, a kidney swap was the only option for him to get a living donor kidney. As part of the PKE, the patient’s wife donated a kidney to another patient, continuing the chain.
“The success of the procedure was even more dramatic because the UMMC pair was the key to fast- track repair for this swap that involved 28 surgeries over a three-week window,” says Garet Hil, CEO of the National Kidney Registry (NKR).”These kinds of bold and complex breakthroughs are what we have come to expect from NKR member centers that are always looking to find new ways to improve the lives of patients suffering from kidney failure.”
Leeser explained that University of Maryland surgeons routinely remove both polycystic kidneys during a transplant, with one team working in one operating room, and another team in an adjacent OR to procure the donor organ. While another center had combined PKD removal with a PKE swap for a patient who was already on dialysis, this procedure was especially complex due to the need for precise timing in the absence of dialysis.
Leeser and his team developed a detailed plan for this case, including backup plans to minimize any risks or problems, such as a delay in the arrival of the donor kidney. The team was prepared to initiate an immediate dialysis session, but it was not needed. They also had a backup plan to keep the paired kidney chain going in the event they could not complete the PKD procedure. Another compatible recipient was available to accept the donor organ, if needed.
Leeser says the entire process was almost seamless. “Just as the new kidney arrived in our operating room, we wrapped up our removal procedure, and other members of our transplant team began working in that same OR to transplant the donor kidney."
PKD is a genetic disorder that can enlarge kidneys to the size of footballs, cram them with fluid-filled sacs and impede the ability of the kidneys to clear toxins and fluids from the body. PKD affects about 500,000 people in the U.S.
UMMC is one of only a handful of centers in the U.S. that treat PKD by removing both dysfunctional kidneys (a procedure called a bilateral nephrectomy) and replacing them with a living donor kidney in one operation. Patients with PKD benefit both from this surgical approach as well as an innovative PKD research program led by UM SOM faculty members, as explained in this video.
The kidney recipient, 49-year-old Wayne Hubbard of Cincinnati, a retired police officer, had been diagnosed with PKD in his 20s, but his condition worsened markedly in the last seven years, with the enlarged kidneys impeding his breathing, and causing fatigue. “I could have gone on dialysis, but that wouldn't have solved my other problems,” says Hubbard.
"When I saw that UMMC would remove both kidneys and do a transplant at the same time, I went on the paired kidney exchange waiting list for about a year-and-a-half, until everything aligned."
“The hereditary nature of polycystic kidney disease can make it difficult for patients with PKD to find suitable donors among their siblings, parents or children who may have PKD themselves. In that case, the patient may turn to non-blood relatives or friends and co-workers to find a living kidney donor,” says E. Albert Reece, MD, PhD, MBA, vice president for medical affairs at the University of Maryland and the John Z. and Akiko K. Bowers Distinguished Professor and dean of the University of Maryland School of Medicine. “This surgical breakthrough may widen the options for PKD patients by drawing on the powerful ability of a paired kidney exchange to find compatible donors from throughout the U.S.”
At the UM SOM Baltimore Polycystic Kidney Disease Research and Clinical Core Center, researchers have worked to better understand the disease, which is caused by mutations in two genes. The center is currently involved in a range of clinical trials. UM SOM scientists are also doing research on how to improve organ transplantation. Among their efforts:
- Developing better ways of helping the body accept the transplant without rejection;
- Using tissue regeneration to increase the number of available organs;
- Creating more efficient operative tools, materials and techniques;
- And developing medical devices to help patients who need a transplant but are not at the top of the wait list, or don’t have an available donor organ.
About the University of Maryland School of Medicine
The University of Maryland School of Medicine was chartered in 1807 and is the first public medical school in the United States and continues today as an innovative leader in accelerating innovation and discovery in medicine. The School of Medicine is the founding school of the University of Maryland and is an integral part of the 11-campus University System of Maryland. Located on the University of Maryland’s Baltimore campus, the School of Medicine works closely with the University of Maryland Medical Center and Medical System to provide a research-intensive, academic and clinically based education. With 43 academic departments, centers and institutes and a faculty of more than 3,000 physicians and research scientists plus more than $400 million in extramural funding, the School is regarded as one of the leading biomedical research institutions in the U.S. with top-tier faculty and programs in cancer, brain science, surgery and transplantation, trauma and emergency medicine, vaccine development and human genomics, among other centers of excellence. The School is not only concerned with the health of the citizens of Maryland and the nation, but also has a global presence, with research and treatment facilities in more than 35 countries around the world. For more information, visit http://medschool.umaryland.edu.
About the University of Maryland Medical Center
The University of Maryland Medical Center (UMMC) is comprised of two hospitals in Baltimore: an 800-bed teaching hospital — the flagship institution of the 12-hospital University of Maryland Medical System (UMMS) — and a 200-bed community teaching hospital, UMMC Midtown Campus. UMMC is a national and regional referral center for trauma, cancer care, neurocare, cardiac care, diabetes and endocrinology, women's and children's health, and has one of the largest solid organ transplant programs in the country. All physicians on staff at the flagship hospital are faculty physicians of the University of Maryland School of Medicine. At UMMC Midtown Campus, faculty physicians work alongside community physicians to provide patients with the highest quality care. UMMC Midtown Campus was founded in 1881 and is located one mile away from the University Campus hospital. For more information, visit www.umm.edu.
Contact
Department of Anesthesiology
(410) 328-6120 (phone)
(410) 328-5531 (fax)
swalsh@som.umaryland.edu
Bill Seiler
Media Relations
410-328-8919
bseiler@umm.edu
Related stories

Monday, March 14, 2022
UMSOM Transplant Surgeon Performs Maryland's First Robot-Assisted Living Donor Kidney Transplant
Innovative Surgery Performed at the University of Maryland Medical Center Promises Reduced Hospital Stay and New Options for Obese Patients

Wednesday, March 09, 2022
IN MEMORIAM: David Bennett, Sr.
David Bennett, the 57 year old patient with terminal heart disease who made history as the first person to receive a genetically modified pig’s heart, passed away yesterday on March 8. Mr. Bennett received the transplant on January 7 and lived for two months following the surgery. His condition began deteriorating several days ago. After it became clear that he would not recover, he was given compassionate palliative care. He was able to communicate with his family during his final hours.

Friday, May 28, 2021
Grateful Patient David Carroll Makes a $1 Million Bequest Pledge to Support the Future of the Advanced Heart Failure Program
University of Maryland School of Medicine (UMSOM) Dean E. Albert Reece, MD, PhD, MBA, announced today that grateful patient David Carroll has made a generous $1 million bequest pledge in support of the Advanced Heart Failure (AHF) program in UMSOM’s Department of Medicine’s Division of Cardiovascular Medicine. This gift follows an initial five-year pledge of $5,000 made by Mr. Carroll in 2017 for operating support of the program.

Monday, March 29, 2021
Cancer Drug Lessens the Toxicity of a Protein from the Virus that Causes Covid-19, UM School of Medicine Study Finds
University of Maryland School of Medicine (UMSOM) researchers have identified the most toxic proteins made by SARS-COV-2—the virus that causes COVID-19 – and then used an FDA-approved cancer drug to blunt the viral protein’s detrimental effects. In their experiments in fruit flies and human cell lines, the team discovered the cell process that the virus hijacks, illuminating new potential candidate drugs that could be tested for treating severe COVID-19 disease patients. Their findings were published in two studies simultaneously on March 25 in Cell & Bioscience, a Springer Nature journal.
Wednesday, August 23, 2017
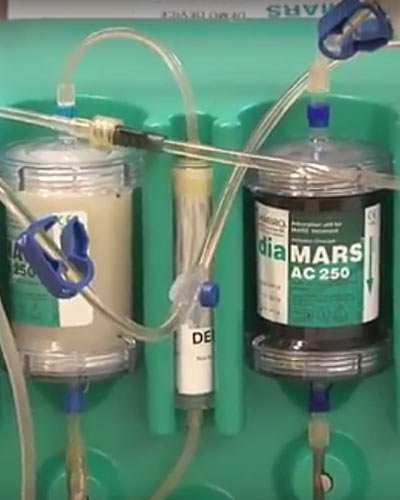
New Use of Blood Cleaning Device Saves High-Risk Patients With Liver Failure
Severe acute liver failure (ALF), a rare but life-threatening illness, is associated with high death rates if patients don’t receive timely treatment or a liver transplant. Unlike the heart or the kidneys, there is no established mechanical device to replace the liver’s function. Now, University of Maryland School of Medicine (UM SOM) researchers report that a device that removes toxins from the blood can also effectively provide a bridge to liver transplantation or buy time for a traumatically injured liver to heal, suggesting broader uses for the device than previously thought.
