Vol. 4 Issue 1
Please select a topic or scroll down the page:
Letter from Chair | Promoted Faculty | Clinical Spotlight | Research Spotlight | Welcome New Faculty | Philanthropy | Service Excellence | Resident Updates | Archive

Letter from the Chair
Happy New Year to all, and I am already hoping for an early Spring! Fortunately, Spring is just around the corner now, and one of my favorite times of year for a multitude of reasons. I love the longer days of sunlight, the warmth, and the rebirth of all the trees and flowers.
Reflecting on this past year, I am struck by how dedicated everyone has been, and how we have continued to adapt to the changing tides of healthcare. Notably, we have developed ambulatory strategies, stretched to find financial sustainable solutions for complex problems, grown with our system partners, and maintained our commitment to high quality care. We have continued to expand our footprint by mostly growing off the downtown campus. As a Department, we have focused on expanding our clinical enterprise throughout Maryland and into surrounding states. Research and education remain essential elements of our core mission, and we continue to find ways to incorporate these into all we do. To do all this we have relied on the power of partnership between the SOM and UMMC, and this has never been stronger. The Department of Surgery is shining brightly.
The Department has forged new relationships in Pennsylvania, allowing the University of Maryland faculty to provide excellent care to a new patient population and enabling its educators to expand their influence in training the next generation of surgeons into new areas. This expansion of services is a testament to the Department's commitment to providing quality healthcare to a diverse patient population. Along these lines last month, the Department of Surgery opened its third office-based lab and clinic within Prince George's County, adjacent to the University of Maryland Capital Region Health Campus. This project has been an extensive undertaking for the entire Department and will allow for the expansion of critical services within Southern Maryland. This new facility, in conjunction with the efforts of the University of Maryland Capital Region Health team, will also allow for continued expansion of faculty services in the region, including the development of a new cancer care service line. With plans for a dedicated cancer center to be opened in the Spring of 2024, the Department is committed to expanding cancer services in Prince George's County, led by the recruitment of Dr. Magesh Sundaram and Dr. Benjamin Powers. Their goal is to provide high-level surgical oncology care in a community with a higher-than-average mortality rate due to all malignancies.
The fall of 2023 provided many examples of innovation and education in the Department. With her connections to the R.H. Smith School of Business, Dr. Kimberly Lumpkins organized for the Department a mini-MBA for faculty, residents, and staff. This three-day program was a resounding success, and we look forward to continuing this collaboration. Making national and international headlines the world’s second swine to human cardiac transplant was performed under the leadership of Dr. Muhammad Mohiuddin and Dr. Bartley Griffith. This work continues to allow us to dream of the day when organ shortage is eliminated, and more individuals can benefit from lifesaving transplantation.
As we embark on 2024, the Department of Surgery continues its four-prong commitment to teaching, research, innovation, and clinical excellence. We have significant philanthropic support (showcased in this newsletter) which we will continue to leverage for critical unsupported needs. The Department will continue transforming and growing as an organization with the help of all of you. With gratitude and unwavering dedication, the Department is poised for team success. Looking forward to a great and prosperous 2024!
Best wishes,
Christine Lau, MD, MBA
Recently Promoted Faculty
Faculty were promoted to the titles listed below their name.

Michael W. Phelan, MD
Professor, Division of Urology

Yvonne M. Rasko, MD
Professor, Division of Plastic Surgery

Mohammad Minhaj Siddiqi, MD, FACS
Professor, Division of Urology

James M. Brown, MD
Professor, Division of Cardiac Surgery

Mehrdard Ghoreishi, MD
Associate Professor, Division of Cardiac Surgery
Clinical Spotlight

Rachel Bluebond-Langner, MD
Grand Rounds:
Dr. Kristin Stueber Plastic Surgery Endowed Lectureship
Thursday, February 8, 2024 / 7:30 am
Shock Trauma Auditorium
22 S. Greene Street, T1R18
Baltimore, MD 21201
Presented by:
Rachel Bluebond-Langner, MD
Laura and Isaac Perlmutter Professor of Reconstructive Plastic Surgery
Hansjorg Wyss Department of Plastic Surgery
NYU Langone Health
Kristin Stueber, MD, '69, FACS
Kristin Stueber, MD is a 1969 University of Maryland School of Medicine graduate. She served as a resident from 1970-1972, was the first full-time plastic surgeon on staff at the University of Maryland, and was a faculty member from 1977-1987.
Dr. Stueber serves on the Board of Directors of the Medical Alumni Association of the University of Maryland and is a member of the 1807 Circle of the John Beale Davidge Alliance, a recognition society for major donors of the University of Maryland School of Medicine. Dr. Stueber lives and works in Springfield, Massachusetts.
Research Spotlight

Bradley S. Taylor, MD, MPH
Division Head, Division of Cardiac Surgery
Dr. Joseph S. and Irene P. McLaughlin Professorship in Cardio-Thoracic Surgery Director, System Integration University of Maryland School of Medicine Co-Director, Aortic Center University of Maryland Medical Center
UM Center for Aortic Disease at the Forefront of Innovation in the OR with Trial Research
The Endo-Bentall procedure is a groundbreaking step forward in aortic root/ascending aortic repair and means that more people can survive these devastating Type A dissections in a less invasive manner,” says Bradley S. Taylor, MD, MPH, the Dr. Joseph S. and Irene P. McLaughlin Professorship in Cardiothoracic Surgery, Professor of Surgery, and Chief of Cardiac Surgery at UMSOM. “This kind of innovation is a testament to the incredible teamwork and collaboration we are fortunate to enjoy here at the University of Maryland Medical Center.”
Brad Taylor, MD, MPH, Professor of Surgery and Vice Chief, Division of Cardiac Surgery and Shahab Toursavadkohi, MD, Assistant Professor of Surgery, the University of Maryland Center for Aortic Disease is among the nation's top tier of centers for the treatment of aortic dissection and aneurysm. The Center's comprehensive array of aortic clinical trials helps ensure University of Maryland Medical Center (UMMC) surgeons provide definitive treatment for every patient presented to them with aortic disease including the more complex in nature. Only an elite group of the nation's hospitals currently offer access to as many state-of-the-art, investigational aortic repair devices as available at UMMC through participation in a clinical trial. For many patients, these early feasibility trials and pivotal trials are the reason they are alive today.
The following current prominent University of Maryland (UM) Center for Aortic Disease trials investigate leading-edge devices to supply a full gamut of minimally invasive, endovascular solutions for disease along any portion of the aorta, including the ascending aorta and the aortic arch. As such, these trials well-equip UM surgeons to provide definitive care, and ultimately hope, for all patients regardless of their case complexity or ability to tolerate surgery.
This operation represents the new frontier in endovascular repair of the aortic root, aortic valve and ascending aorta and significantly diminishes the physiologic demands of recovery for the patient. It is a testament to the team of cardiac, vascular, and interventional cardiologists whose collective intelligence was used to solve a complex problem for patients now and into the future.
The team, led by Mehrdad Ghoreishi, MD, Associate Professor of Cardiac Surgery at the University of Maryland School of Medicine and Co-Director of the Center for Aortic Disease at UMMC, and Shahab Toursavadkohi, MD, Associate Professor of Vascular Surgery at UMSOM and Co-Director of the Center for Aortic Disease, is advancing medicine and recreating the approach to treating ATAAD.
Please click the link below to learn more about the Endo-Bentall procedure and Aortic Root treatment.
Published Study
Recent Awards
- Aidan Wiley was awarded 1st place at the 46th Annual Medical Student Research Day. Aidan spent the past summer working on a project, Evaluating the Use of Ocular Thermography to Detect Carotid Stenosis, at the Center for Vascular Research.
- Congratulations To Dr. Stephen Kavic as the recipient of the Campbell and Jeanette Plugge Professorship in Surgery.
Welcome New Faculty

Benjamin D. Powers, MD, FACS, FSSO
Assistant Professor, Division of General and Oncologic Surgery
Dr. Powers obtained his medical degree from Wayne State University School of Medicine in 2009. He completed his general surgery residency in 2016 from Temple University Hospital where he was Chief Resident. He completed a two-year Complex General Surgical Oncology Fellowship from Moffitt Cancer Center, where he was asked to join the faculty as an Assistant Professor in the Department of Oncologic Sciences at the University of South Florida, Morsani College of Medicine.

Assistant Professor, Division of Thoracic Surgery and Surgical Care
Dr. Krause obtained a juris doctor degree in 2008 from the University of Michigan Law School and his medical degree in 2012 from the University of Michigan Medical School. He started his internship here at the University of Maryland Medical Center from 2012-2015 and spent two-years in Surgical Critical Care Fellowship program at the University of Pennsylvania, before returning in 2017 to complete his Integrated Thoracic Surgery Residency here at the University of Maryland.

Assistant Professor, Division of Thoracic Surgery.
Dr. Egyud obtained his medical degree from Boston University School of Medicine in 2013. He completed his general surgery residency, including a two-year postdoctoral fellowship, from Boston Medical Center in 2020, serving as Administrative Chief Resident. He completed a two-year fellowship in Cardiothoracic Surgery at the Texas Heart Institute of Baylor’s College of Medicine in July 2023.

Clinical Assistant Professor, Division of Vascular Surgery
Dr. Harding obtained his Doctor of Osteopathic Medicine from the Edward Via College of Osteopathic Medicine in 2017 graduating summa cum laude. He was a recipient of a four-year Health Professions Scholarship from the United States Air Force and was later chosen as the Vascular Surgery Resident of the Year and recipient of the Society of Clinical Vascular Surgery Scholarship in 2022.

Instructor, Division of Vascular Surgery
Dr. Gupta obtained his MD from the American University of Antigua, College of Medicine in 2016 graduating magna cum laude. He completed his general surgery residency at Saint Agnes Hospital Center in Baltimore in 2021 serving as Administrative Chief Resident.

Associate Professor, Division of General and Oncologic Surgery
Dr. Sundaram obtained his medical degree from the University of Maryland School of Medicine in 1990. He completed his General Surgery Residency in 1995 from Christiana Care and his Surgical Oncology Fellowship in 1997 from the University of Miami. He received his MBA in Health Care Administration from the University of Miami in 2001.
.jpg)
Clinical Assistant Professor, Division of Cardiac Surgery
Dr. Belyayev obtained his medical degree from Uniformed Services University School of Medicine in 2015. He completed his General Surgery Residency from Walter Reed National Military Medical Center in 2021. In addition, he completed a one-year Transplant Immunology Fellowship from MedStar Georgetown Transplant Institute at Georgetown University in 2019, and a two-year Cardiothoracic Surgery Residency from Brigham and Women’s Hospital at Harvard Medical School in July 2023.

Professor, Division of Cardiac Surgery
Dr. Massey obtained his medical degree from the Medical College of Georgia Augusta in 1990. He completed his General Surgery Residency at the University of Louisville in Kentucky, Thoracic and Cardiovascular Surgery Residency from the University of Texas Southwestern, and Heart and Lung Transplantation Fellowship from Duke University Medical Center.

Joseph & Corinne Schwartz
Transforming the Future Through Philanthropy
Remembering Joseph and Corinne Schwartz
On February 6th, Valeria R. Mas, MS, PhD was invested as the inaugural Joseph and Corinne Schwartz Professor of Surgical Sciences Research in Transplantation. This $1.5 Million endowment was given to the University of Maryland School of Medicine by the late Joseph M. Schwartz and Corinne "Peachy" Schwartz, to support discovery and advancement in transplantation science.
Joseph and Corinne believed in philanthropy’s power to influence lasting social change. They made an impact by generously donating more than $6 million to the University of Maryland School of Medicine and Medical Center during their lifetime. They established the Joseph and Corinne Schwartz Division of Transplantation, the Joseph and Corinne Schwartz Professorship in General Surgery held by Jian-Ying Wang, MD, PhD, the Joseph and Corinne Schwartz Surgical Suite, and the Joseph and Corinne Schwartz Stroke and Brain Injury Center.
As a 1939 Baltimore City College graduate, Joseph had a remarkable life that included serving in World War II, where he flew 31 bombing missions over Germany as the lead navigator for his squadron. In the 1960s, 70s, and 80s, he built an impressive real estate portfolio, constructing 1,500 apartment units and large townhome developments in the Baltimore Metropolitan area. He also played a role in the revitalization of Fells Point, including the development of Thames Point Apartments. He had diverse interests including owning the San Diego Mariner hockey team and a racehorse named Sudanese.
After Joseph 's passing in November 1999, Corinne continued the family legacy by making generous donations to many organizations like St. Jude's Children's Research Hospital and the National Aquarium in Baltimore until her passing in 2018.
Joe and Corinne made an enduring legacy that will impact thousands of lives for generations. We are grateful for their significant contributions to the advancement of medicine, academic research and education.

Service Excellence
What’s New in FY24?
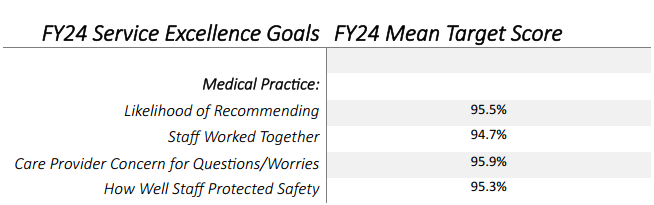
Every year, FPI reviews the current Service Excellence goals to ensure they are still in line with the organization’s focus and what matters most to our patients. Creating positive patient experiences and gaining loyalty to drive the likelihood of recommending our practices to others is what we strive for each day.
As we enter FY24, Likelihood to Recommend will remain our overall goal and we will continue to track Staff Worked Together and Care Provider Concern for Questions/Worries. In lieu of Wait Time, we are now focusing on How Well Staff Protected Safety. This is something that has proven important to our patients and a key driver. We are off to a strong start and have the ability to achieve our goals in FY24. Strive for excellence in all that you do and gain the loyalty of our patients to keep them coming back.
Surgical Education Updates
The University of Maryland Department of Surgery continues to enjoy great successes, and has become a destination for surgical education.
Ten students from the senior class of Maryland medical students have applied for general surgery residency this year. This represents about 7% of the graduating class. The national Match Day for our students is Friday, March 15, 2024.
The residency program also remains incredibly popular, and we received nearly 2,000 applications for our six positions. The University of Maryland attracts almost double the number of applicants as an average surgery residency program. Part of the appeal is that our residents are incredibly academically productive: over the first six months of this academic year, the residents combined for a phenomenal 51 peer-reviewed publications! It is no surprise that all of our chief residents matched into premier fellowship positions:
Megan Birkhold, Pediatric surgery, University of California San Diego
Laura Cooper, Colon and rectal surgery, Pennsylvania State University
Richa Kalsi, Vascular surgery, University of Maryland
Olivia Martin, Surgical oncology, Roswell Park
Neerav Patel, Minimally invasive surgery, University of Maryland
Nikhil Prasad, Cardiothoracic surgery, Brigham and Womens Hospital.
A number of donors have recognized the impact of our surgical trainees. We are grateful to report that individual donors pledged over $500,000 in donations this year to support resident education and research.

Department of Surgery Highlights
The Grand Opening of our state-of-the-art Office-Based Lab in Largo, MD.
At this new location, faculty physicians from the University of Maryland School of Medicine are providing expert vascular and surgical care to residents of Prince George’s County and surrounding areas.

Resident Wellness Day: is a day prepared for the General Surgery Residents to relax and do some fun activities with there peers.
December 28, 2023, We had a Sip & Paint with food/beverages.

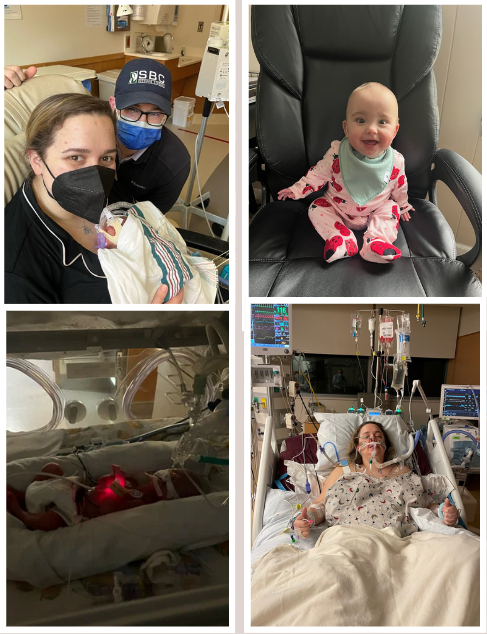
Kaitlyn Vecere - Birth Story
Hi, my name is Kaitlyn Vecere. If you are a member of the Department of Surgery, you’ve probably seen me in the Chair’s Suite in passing, emailed me to ask for an EPIC report, or come to my office to find candy. However, some of you may not know about my daughter, Charlotte, and the events surrounding her birth…
March 15th will be a day I will never forget. Certainly, all mothers must say that about the day their first child is born. March 15th was a chilly Wednesday in 2023, a rather plain day, if you ask me. I reported to work in the morning, as usual but, around 9:30, or so, I started not feeling too well. I was having some stomach cramping, or what I though was stomach cramping, that just didn’t seem to get better, no matter what I did. Unlike most upset stomachs, ginger ale and Tylenol were no match for this pain. Since the office was quiet, I thought I might lay down on Dr. Lau’s couch to see if I just needed to be horizontal for a minute. Well, a minute turned into an hour, which turned into becoming cold, lightheaded, and calling my husband to come pick me up. I called Women’s Health in the 419 Building to see if they agreed that I should be seen prior to heading back to Carroll County. They agreed and instructed me to go to Labor and Delivery in the hospital. In the time it took for my husband to get me into a wheelchair and take me to the 7th floor (my office is only on 8), my pain became excruciating. Fast forward to L&D triage: we’re checking all the potential causes, I’ve gotten some pain medicine onboard, yet the cause of my pain is not incredibly obvious. After being in triage for a little over an hour, my symptoms became an emergency.
Around 1:30 that afternoon, I was told I was experiencing a placental abruption, that I was going to be having an emergency c-section, and we needed to get rolling. I gave my husband a kiss, let a couple of tears roll down my cheek, and I was out. The last thing I remember is the anesthesia team preparing to intubate me with the LMA – I saw it come from over/behind me, it touched my lip, and I was out. My daughter, Charlotte Jane, was born at 1:42pm via emergency c-section at 25 weeks and 1 day gestation. Charlotte came into the world blue and pulseless, requiring immediate resuscitation and care from the Neonatal Intensive Care Unit team. I was in the OR for about 4 hours and lost more than half of my blood volume. According to my husband, I was following commands much earlier than 11:30 that night but I don’t remember anything before then. When I had fully come around, I was in the SICU, still intubated, with an open abdomen, and restrained, so I didn’t self-extubate. The first thing I wrote on my whiteboard was, “how is the baby?” I wouldn’t meet her for 2 days.
Well, after spending 5 days in the hospital myself, and 90 days for Charlotte, I’m happy to report that we’re planning her 1st birthday party and she is thriving! She’s come an awful long way from the tiny baby that joined us back in March. Her heart defect is resolving, she is off oxygen, and her eyes are fully vascularized! Saying thank you everyone who cared for us just doesn’t seem like enough. Thank you to Dr. Lankford for delivering our girl safely. Thank you to Dr. Schofield for being Charlotte’s voice while I was recovering. Thank you to Dr. Desai for taking off that horrible wound vac and closing my belly. Thank you to the NICU, SICU, Labor and Delivery, and Mother-Baby nurses. Thank you, University of Maryland Medical Center.