February 16, 2018 | David Kohn

Clinical Trial Is the Final Test Before FDA Approves Use of Promising Nonsurgical Treatment Option
University of Maryland Medicine (the University of Maryland Medical Center (UMMC) and the University of Maryland School of Medicine (UMSOM)) is leading a phase 3 study to test the safety and efficacy of using MRI-guided focused ultrasound on the brain in order to treat Parkinson’s disease. The pivotal study is the final step before the U.S. Food and Drug Administration (FDA) will consider approving the new technology for widespread use as a nonsurgical treatment option to eliminate key motor symptoms of this common neurological condition.
“The goal of the focused ultrasound treatment is to both lessen the main symptoms of Parkinson’s disease, which include tremors, rigidity and slow movement, as well as treat the dyskinesia that is a medication side effect, so that less medication is needed,” says principal investigator Howard M. Eisenberg, MD, professor and chair of neurosurgery at UMSOM and chair of neurosurgery at UMMC.
MRI-guided focused ultrasound is a noninvasive technique that uses sound wave energy to ablate cells within the body. Magnetic resonance imaging (MRI) allows doctors to define the target inside the body and create a heat map so they know exactly where to aim. In this case, doctors guide ultrasound waves through the skin and skull to precisely target the globus pallidus, a structure deep in the brain that helps regulate voluntary movement. This approach does not use radiation or invasive surgery.
As many as one million Americans have Parkinson’s disease, a chronic, degenerative disorder for which there is no cure. The second most common movement disorder, Parkinson’s disease results from the malfunction or loss of brain cells crucial for movement and coordination. Symptoms include motor difficulties such as tremor, rigidity and impaired balance. People with Parkinson’s can also experience non-motor symptoms of cognitive impairment, depression and anxiety, and autonomic dysfunction.
Current treatments include medication, with levodopa being the most widely used. In advanced cases, deep brain stimulation with surgically implanted micro-electrodes is used to treat motor symptoms of tremor, rigidity and dyskinesia. Dyskinesia (abnormal, distorted movement) is a common medication side effect that can drastically affect quality of life for patients with Parkinson’s.
This is the second clinical trial of MRI-guided focused ultrasound for Parkinson’s disease. The pilot study, also led by University of Maryland Medicine, began in 2015 and showed promising results.
“The results of the pilot trial, so far, are very encouraging,” says Dr. Eisenberg of the 2015 trial that involved 20 patients, most of whom were treated at UMMC.
The pilot trial focused on a subset of patients who had symptoms that were worse on one side of the body, as well as severe dyskinesia where medication had failed. The patients received focused ultrasound and most experienced significant improvement in their tremors. The new larger study aims for 80 to 100 participants, and is designed with a softer inclusion criteria, so more patients will be eligible.
“For people with Parkinson’s disease and other movement disorders such as essential tremor, focused ultrasound is an appealing alternative to deep brain stimulation because it does not involve more invasive surgery,” says Paul S. Fishman, MD, PhD, professor of neurology at UMSOM and a neurologist at UMMC.
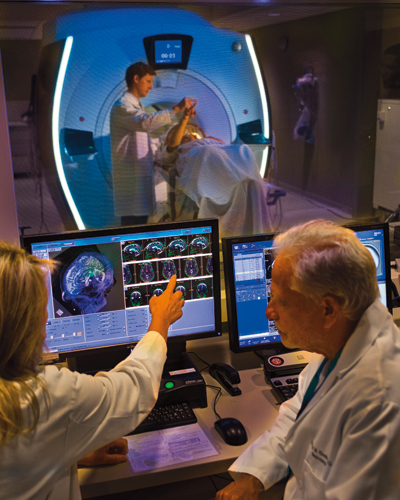
The procedure is performed in an outpatient setting. The patient is awake the entire time, lying in an MRI scanner with a head-immobilizing frame fitted with a transducer helmet, which converts energy from one form to another. Ultrasonic energy is targeted through the skull to the globus pallidus of the brain, and images picked up during the procedure give doctors a real-time temperature map of the area being treated. Doctors raise the temperature in a very restricted area of the brain to ablate tissue. During the procedure, the patient is awake, alert and giving feedback, which allows doctors to monitor the immediate effects of treatment and make adjustments.
“University of Maryland Medicine is a world leader in pioneering MRI-guided focused ultrasound to become a new standard of care for treating many devastating brain diseases including Parkinson’s, essential tremor and glioblastoma, an often deadly type of brain cancer,” says E. Albert Reece, MD, PhD, MBA, vice president for medical affairs at the University of Maryland and the John Z. and Akiko K. Bowers Distinguished Professor and dean of UMSOM.
The multi-site Parkinson’s study is expected to begin in February 2018 with UMMC as the primary treatment site. Insightec is funding the study. Dr. Eisenberg is a consultant to Insightec. For more information about this or other clinical trials for Parkinson’s disease, please contact Charlene Aldrich, RN, MSN, clinical research manager, at 410-328-5332.
About the University of Maryland Medical Center
The University of Maryland Medical Center (UMMC) comprises two hospitals in Baltimore: an 800-bed teaching hospital – the flagship institution of the 14-hospital University of Maryland Medical System (UMMS) – and a 200-bed community teaching hospital, UMMC Midtown Campus. UMMC is a national and regional referral center for trauma, cancer care, neurological care, cardiac care, diabetes and endocrinology, women’s and children’s health, and has one of the largest solid organ transplant programs in the country. All physicians on staff at the flagship hospital are faculty physicians of the University of Maryland School of Medicine. At UMMC Midtown Campus, faculty physicians work alongside community physicians to provide patients with the highest quality care. UMMC Midtown Campus was founded in 1881 and is located one mile away from the University Campus hospital.
About the University of Maryland School of Medicine
Commemorating its 210th Anniversary, the University of Maryland School of Medicine was chartered in 1807 as the first public medical school in the United States. It continues today as one of the fastest growing, upper-tier biomedical research enterprises in the world -- with 43 academic departments, centers, institutes, and programs; and a faculty of more than 3,000 physicians, scientists, and allied health professionals, including members of the National Academy of Medicine, and distinguished recipient of the Albert E. Lasker Award in Medical Research. With an operating budget of more than $1 billion, the School of Medicine works closely in partnership with the University of Maryland Medical Center and Medical System to provide research-intensive, academic and clinically-based care for more than 1.2 million patients each year. The School has 1,307 students, 685 residents, 562 fellows, and nearly $450 million in extramural funding, with more than half of its academic departments ranked in the top 20 among all public medical schools in the nation in research funding. As one of the seven professional schools that make up the University of Maryland, Baltimore campus, the School of Medicine has nearly 7,000 total employees. The combined School and Medical System (“University of Maryland Medicine”) has a total budget of $5 billion and an economic impact of nearly $15 billion on the state and local community. The School of Medicine faculty, which ranks as the 8th-highest public medical school in research productivity, has been an innovator in translational medicine with 600 active patents and 24 start-up companies. The School works locally, nationally, and globally, with research and treatment facilities in 36 countries around the world. Visit medschool.umaryland.edu/
Contact
Office of Public Affairs
655 West Baltimore Street
Bressler Research Building 14-002
Baltimore, Maryland 21201-1559
Contact Media Relations
(410) 706-5260
Related stories

Wednesday, November 13, 2019
UM School of Medicine Establishes Endowed Professorship in Neurosurgery Through Private Gifts and Matching State Funds
University of Maryland School of Medicine (UMSOM) Dean E. Albert Reece, MD, PhD, MBA, announced today that the UMSOM has been awarded matching funds from the Maryland E-Nnovation Initiative Fund (MEIF), administered by the Maryland Department of Commerce. The funds, when combined with private philanthropy, will enable UMSOM to establish the Howard M. Eisenberg, MD, Distinguished Professorship in Neurosurgery.

Thursday, March 28, 2019
UM School of Medicine Announces Leadership Transition in Department of Neurosurgery
Dean E Albert Reece, MD, PhD, MBA, announced today that longtime Chair of the Department of Neurosurgery and nationally-recognized neurosurgeon Howard M. Eisenberg, MD, will be stepping down at the end of this academic year as chair after 23 years. He will return to the full-time faculty of the UMSOM Department of Neurosurgery, retaining his title as the R.K. Thompson Professor of Neurosurgery. He will continue his research and his efforts advancing surgical techniques including gamma knife radiosurgery and image-guided focused ultrasound.

Thursday, August 09, 2018
University of Maryland School of Medicine Scientists to Conduct First FDA-Approved Study of Focused Ultrasound to Open Blood-Brain Barrier
In the first such clinical trial in the United States, physician-scientists with the University of Maryland School of Medicine (UMSOM) are investigating the use of MRI-guided focused ultrasound to open the blood-brain barrier. The trial will be conducted with patients undergoing brain cancer surgery at the University of Maryland Medical Center (UMMC).
Tuesday, August 30, 2016
New Study Shows Breakthrough Treatment for Essential Tremor Using Focused Ultrasound
University of Maryland School of Medicine (UM SOM) researchers, along with an international group of investigators, have discovered for the first time that treatment with MRI-guided focused ultrasound can effectively treat patients with essential tremor (ET), a neurological movement disorder that affects an estimated 10 million people in the U.S. The results, which are published in the forthcoming issue of the New England Journal of Medicine, led to recent approval of the treatment by the Food & Drug Administration (FDA),
