Get to Know: Stefan H. Kappe, PhD
April 20, 2026
Distinguished parasitologist and immunologist Stefan Kappe, PhD, recently became the new Director of the UM School of Medicine’s Center for Vaccine Development and Global Health (CVD) and the Myron M. Levine, MD, DTPH Professor of Vaccinology and Vice Chair for Research in the Department of Pediatrics. During his work at the University of Washington and Seattle Children’s Research Institute, he pioneered the use of genetic engineering to develop live attenuated vaccines against the deadly malaria parasites that sicken hundreds of millions of people and kill up to a million people worldwide each year.
In an edited interview, Dr. Kappe discussed his interest in malaria, his lab’s transformative approach to developing a vaccine for the disease, and his vision for the future of CVD.
Q: Can you tell us about your work in Seattle before coming to CVD?
I've been working on malaria since I did my PhD research at the University of Notre Dame. I continued that work as a postdoc at New York University School of Medicine before heading to Seattle more than 20 years ago to start my own research laboratory. We used a variety of preclinical models to interrogate immune responses and understand the interaction of the malaria parasite with the host. At the same time, we were getting better and better in genetically engineering parasites.
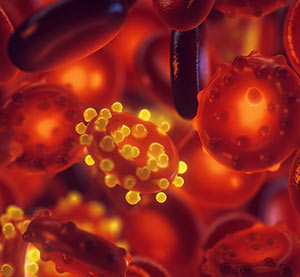
Based on our work to understand the parasite's biology when it first infects the liver and immune system interactions, we focused on developing vaccines that produce immunity against the malaria parasite during this first phase in the human host. The parasite infects the liver first, multiplying there without producing symptoms before getting into the bloodstream and infecting red blood cells, where it causes disease and death. Our goal is to focus on stopping the parasite in the liver before it can go into the bloodstream.
Q: How did you become interested in malaria?
 I’ve always been fascinated by the complexity of biology: As a boy growing up in a small village in Germany, my playground was nature. I was captivated by the insects, snakes, and frogs I found. At university, I took courses in parasitology and began doing experimental work with parasites that infect chickens, which are related to those that cause malaria. While I found the biology of parasites fascinating—every organism that lives on earth has at least one parasite species—I wanted to focus on something more relevant to human health. That’s how I began studying malaria.
I’ve always been fascinated by the complexity of biology: As a boy growing up in a small village in Germany, my playground was nature. I was captivated by the insects, snakes, and frogs I found. At university, I took courses in parasitology and began doing experimental work with parasites that infect chickens, which are related to those that cause malaria. While I found the biology of parasites fascinating—every organism that lives on earth has at least one parasite species—I wanted to focus on something more relevant to human health. That’s how I began studying malaria.
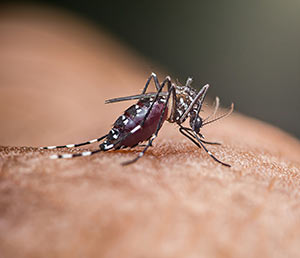
The malaria parasite’s life cycle of infection is sophisticated. It is transmitted to humans by a mosquito bite and then infects the liver. It makes new stages in the liver that then invade the bloodstream and infect red blood cells. It makes sexual stages within the red blood cells, pretty much like a sperm and egg, that get taken up by mosquitoes again when they bite and take blood from an infected person. Sex occurs in the mosquito and then the parasite goes to the salivary glands, where it is laying in wait for the mosquito to bite again and infect a new person. The biology is just very complex and beautiful, in a way. But it’s also deadly, which is how I got interested in malaria and malaria vaccines.
An estimated 300 to 500 million people are suffering from malaria each year, so the health burden is tremendous. About up to a million of those people infected will die, with much of the morbidity and mortality concentrated in sub-Saharan Africa, but it’s also prevalent in Southeast Asia and South America.
Q: Tell us about your approach using live attenuated malaria parasites and how it’s different than what’s been tried before.
 The malaria parasite contains about 5,000 proteins, and the traditional approach to vaccine development has been to pick a single protein of the 5,000, make it into a recombinant protein, and immunize with it in the hope that you get potent immune responses that block infection. The approach has borne fruit. There are two vaccines, RTS,S and R21, currently being implemented in Africa, but they offer only modest protection against malaria, between 20 and 50%. While they are good tools to lower the disease burden, they cannot ultimately eliminate malaria.
The malaria parasite contains about 5,000 proteins, and the traditional approach to vaccine development has been to pick a single protein of the 5,000, make it into a recombinant protein, and immunize with it in the hope that you get potent immune responses that block infection. The approach has borne fruit. There are two vaccines, RTS,S and R21, currently being implemented in Africa, but they offer only modest protection against malaria, between 20 and 50%. While they are good tools to lower the disease burden, they cannot ultimately eliminate malaria.
Our approach is what we call an antigen-agnostic approach; we don't pick proteins from the parasite and make them into recombinant vaccines. We use genetic engineering with CRISPR to delete the genes that allow the parasite to leave the liver and cause disease, leaving only those that are important for the parasite to replicate in the liver. These engineered parasites infect the liver and replicate, creating an immune response, and then die off. Instead of picking one target protein, we use a weakened parasite and get an immune response to hundreds, if not thousands, of proteins, inducing very potent immunity. Early stage clinical studies have demonstrated that these vaccines are safe and one study showed around 90% protection against malaria infection with a single dose, which is unheard of.
We’re not the first lab to use a whole parasite approach, and I should note we stand on the shoulders of researchers like Ruth Nussenzweig and Jerome Vanderberg, who in the 1960s showed that you could irradiate malaria parasites to weaken them and use them in immunizations. There are drawbacks to that approach, notably that irradiated vaccines are not very practical to make, and it turns out they also do not confer optimal immunity. New genetic engineering technologies are allowing us to use this approach in a practical way and make the vaccine more potent.
Q: What drew you to pursue becoming the director of CVD?
CVD is a unique place with its focus on diseases of global importance, not only diseases that have an impact here in the United States. It is focused on developing interventions, particularly vaccines, that can help fight those global infections; not only malaria, but diarrheal diseases and respiratory infections. While my lab in Seattle was obviously very successful in our vaccine work, the organization I worked for didn’t have this focus on global infectious diseases and vaccines that are needed most in the world, particularly for children.
Now at CVD, I am surrounded by a community of wonderful people who have the mission of eliminating and eradicating infectious diseases globally and saving millions of lives by making vaccines that protect against infectious diseases. It’s exciting, very energizing and a lot of fun, and allows me to not only further develop our malaria vaccine, but to help others at CVD advance their own approaches for other infectious diseases. That's why I came.
Q: What is your vision for the future of CVD? Are there any lines of research you’re personally interested in pursuing?
 There is wonderful work going on in the vaccine space at CVD, as well as implementation work in endemic disease areas like Africa and Southeast Asia. I think the programs in respiratory infections are really very strong, and the enteric infections program, the Shigella work, for example, is just outstanding. CVD’s work in understanding immune response to infection and vaccines is also very well developed.
There is wonderful work going on in the vaccine space at CVD, as well as implementation work in endemic disease areas like Africa and Southeast Asia. I think the programs in respiratory infections are really very strong, and the enteric infections program, the Shigella work, for example, is just outstanding. CVD’s work in understanding immune response to infection and vaccines is also very well developed.
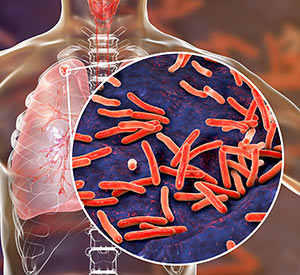
In terms of future projects or where we can do more, tuberculosis is even more important than malaria, in terms of global disease burden, and CVD has room to expand into the tuberculosis space. I’d also like us to develop more research programs focusing on dengue fever, which is close to my heart, with dengue being a mosquito-transmitted disease. We don’t yet have good interventions for dengue.
These are just initial thoughts, and I am still in a fact-finding mode, getting the lay of the land. As I get to know everyone and learn about their projects, I think there are tremendous opportunities for collaboration on the use of disease-transcending research technologies. I also think we can learn faster how to develop better vaccines using computational biology, systems immunology, and artificial intelligence approaches.
Watch the Video
Contact
Office of Public Affairs
655 West Baltimore Street
Bressler Research Building 14-002
Baltimore, Maryland 21201-1559
Contact Media Relations
(410) 706-5260

