"The Prevention Pipeline": UMMC and UMSOM training the next generation of preventive medicine leaders
The Prevention Pipeline is a space dedicated to sharing the people, ideas, and work that drive preventive medicine forward. This blog brings together medical students, residents, and faculty who are united by a commitment to prevention, population health, and upstream approaches to improving health outcomes.
Resident Reflection posts will feature writing by the residents that offers readers an inside look at both their personal paths and their journeys within our program. These reflection posts explore what drew them to the field of preventive medicine and how their interests, skills, and professional identities evolve as they progress toward graduation and future careers.
Some posts will highlight work or research completed in the classroom, projects during practicum rotations, or efforts within the community. Each resident’s passions and career aspirations are unique, and thus the reflections will span a wide range of topics. Along the way, readers may join residents on their walk to work along the harbor, share in the culinary delights of the city, or even learn what they do for fun outside of medicine.
The Student Spotlight highlights the voices and experiences of medical students who are exploring preventive medicine, public health, and population-based care, with a particular emphasis on lifestyle medicine. These posts feature reflections on students’ academic journeys, clinical experiences, research projects, and community engagement that have shaped their interest in prevention, health promotion, and behavior change. Through personal narratives this section showcases how medical students are engaging with upstream determinants of health—including nutrition, physical activity, stress management, sleep, and social connection—and envisioning their future roles as physician leaders in prevention, lifestyle medicine, policy, and public health.
Faculty Features spotlight the voices and work of our faculty and graduates who are advancing prevention and population health in meaningful ways. Through personal reflections, mentorship insights, and career narratives, contributors share lessons learned, pivotal moments, and practical advice for trainees and early-career professionals navigating preventive medicine and public health careers.
_________________________________________________________________________
Read the blogs below:
Welcome to the The Prevention Pipeline
UMMC and UMSOM training the next generation of preventive medicine leaders
January 12, 2026
Happy New Year and welcome to The Prevention Pipeline!
As we begin 2026, the University of Maryland Preventive Medicine residency program is excited to launch The Prevention Pipeline, a space dedicated to sharing the people, ideas, and work that drive preventive medicine forward. This blog brings together medical students, residents, and faculty who are united by a commitment to prevention, population health, and upstream approaches to improving health outcomes.
The Prevention Pipeline highlights the full continuum of training and practice in preventive medicine. Here, medical students explore their early interests and experiences, residents reflect on the challenges and rewards of preventive medicine training, and faculty share expertise, mentorship, and perspectives shaped by years of practice and leadership. Together, these voices reflect the collaborative and interdisciplinary nature of our field.
Throughout the year, this blog will feature accomplishments and milestones, timely public health topics, research and quality improvement efforts, and real-world examples of prevention in action—from clinical preventive services to community-based and policy-level interventions. Our goal is to foster learning, dialogue, and inspiration while showcasing the vital role preventive medicine plays in advancing health equity and population well-being.
As we look ahead to the coming year, we invite readers and contributors alike to engage with The Prevention Pipeline: celebrate successes, reflect on lessons learned, and share ideas that strengthen the future prevention workforce. We look forward to growing this community together and continuing the important work of building health—upstream.
Welcome to a new year—standing outside UMSOM on this crisp January day, I invite you to come follow along with me in The Prevention Pipeline!
Marissa Khajavi MD, MPH
Program Director, Public Health and General Preventive Medicine Residency

Resident Reflections | Insights from preventive medicine residents on training, practice, and professional growth
How Policy Shapes Healthcare, Gabe Pontipiedra
January 20, 2026
How Policy Shapes Healthcare
How Policy Shapes Health Care— The Importance of Involvement of Trainees
As the Maryland Legislative Session starts we are thinking all things policy!
Policies influence everything from access to care and insurance coverage to public health funding and prevention efforts. Physicians witness the downstream effects of these decisions every day—caring for patients whose health is shaped as much by policy and social conditions as by clinical care.
Physician involvement in policy is essential. Clinicians bring real-world experience, scientific expertise, and an understanding of unintended consequences that can strengthen policy decisions. In preventive medicine and public health, policy is one of our most powerful tools to improve population health, reduce inequities, and address health upstream. Engaging in policy—through advocacy, research, education, or advisory roles—allows physicians to help build a more effective, equitable, and prevention-focused health system.
We strive to provide our residents with a rich policy experience. Below find PGY-3 Dr. Gabriel Pontipiedra’s reflection on his policy work thus far. --Marissa Khajavi MD, MPH Program Director
I was drawn to Preventive Medicine because it focuses on addressing health upstream, instead of only reacting once disease has already occurred. During medical school and my prior residency training, I often felt frustrated by how frequently social determinants of health, policy decisions, and inequities were acknowledged but not meaningfully addressed in clinical settings. Preventive Medicine felt like the place where public health, policy, and patient care could actually come together in a real and impactful way.
My policy rotation with The American College of Preventive Medicine (ACPM) and time working on Capitol Hill this past fall were especially meaningful experiences. Translating evidence into advocacy and seeing firsthand how policy decisions shape population health was incredibly eye-opening and reinforced the idea that physicians can—and should—play roles beyond the clinic.
The work I completed with The Maryland Department of Health (MDH) in the Office of Minority and Health Disparities was also meaningful. I worked to analyze racial disparities in infant mortality and low birth weight across Maryland counties. That project brought together data analysis, health equity, and policy relevance in a way that strongly reflects my interests. Seeing how these data directly informed conversations around accountability and targeted intervention was both validating and motivating, and it underscored the potential for policy to address these inequities.
Building on this foundation, my current rotation with MDH in the Bureau of Maternal and Child Health has placed me at the center of the legislative process during session. Through helping prepare testimony, conducting research, and attending hearings in Annapolis, I am seeing firsthand how evidence on infant mortality and disparities can shape policy decisions. Being part of this fast-paced and critically important space has reinforced my belief that thoughtful, data-driven policy work is essential to improving outcomes for mothers and infants across Maryland.
-- Gabe Pontipiedra DO PGY-3 and Chief Resident

Student Spotlight | Medical student perspectives, reflections, and pathways
Healthy Doctors, Connected Lives, Salim Muhammed
January 26, 2026
Health Doctors, Connected Lives
Our program believes we must be healthy doctors to take care of our patients!
A component of our program is the integration of the American College of Lifestyle Medicine curriculum where residents' complete modules, didactics/activities, and lifestyle medicine clinical training. I personally am a strong believer in lifestyle as a preventive tool and that includes one of the pillars of lifestyle medicine- positive social connections.
Strong social connections are powerful—and often overlooked—determinant of health. Meaningful relationships with family, friends, coworkers, and community members are associated with lower rates of chronic disease, improved mental health, and increased longevity, while social isolation has been linked to higher risks of depression, cardiovascular disease, and premature mortality. From a preventive medicine perspective, fostering social connection is an upstream intervention that supports resilience, healthy behaviors, and equitable health outcomes.
Salim Muhammed, MS2, is a member of the Lifestyle Medicine Interest Group. Below he shares why he is interested in Lifestyle Medicine and touches on the importance of social connections for personal and patient health.
-- Marissa Khajavi PD and LMIG advisor
I find Lifestyle Medicine both rewarding and empowering because it gets back to the fundamentals of health and tackles the root causes of disease in a way that is sustainable and effective. What’s especially fascinating is the approach on leveraging and protecting our physiological systems for treatment and prevention. That’s a message and movement I’m excited to practice, share, and promote through LMIG.
Lmig.umsom- Our awesome M2 SGA president shares what her village looks like.
Who we consider in our circle can shift throughout our life—things happen. We move. Priorities change. Major health changes. Death. But throughout it all, our community is grounded all the same: A support system, the people we share our biggest news with first, the ones we can call late at night, and those we can be vulnerable with.

Resident Reflections | Insights from preventive medicine residents on training, practice, and professional growth
From data to prevention, a resident's journey in clinical informatics, Dr. Jenny Su
February 2, 2026
From data to prevention, a resident's journey in clinical informatics
In today’s data-driven healthcare landscape, informatics plays a critical role in transforming information into action. From identifying population-level trends to improving clinical decision-making, medical informatics is a powerful tool for advancing prevention, equity, and high-value care.
At the University of Maryland, preventive medicine residents have exceptional opportunities to build informatics skills and learn how data can be leveraged to improve patient and population health.
A cornerstone of this training is mentorship from leaders in the field, including Dr. Michael Grasso, Director of the Clinical Informatics Group at the University of Maryland School of Medicine. Through this work, residents are exposed to the practical applications of informatics across clinical care, quality improvement, and health systems innovation—preparing them to lead in an increasingly data-driven healthcare environment.
Read below PGY-3 Dr. Jenny Su’s experience during her informatics rotation with Dr. Grasso.
-Marissa Khajavi, Program Director
My transition into Preventive Medicine was driven by a conviction that we must move beyond reactive care to design healthcare systems where the healthiest path is the easiest for both clinician and patient to follow. Before residency, I built a deep foundation in clinical informatics by working with multiple hospital networks across the country. Navigating and optimizing numerous versions of Epic provided me with a unique perspective on adapting to the specific workflows and challenges of diverse organizations, both large and small. Through these experiences, I learned to reduce documentation burdens and translate real-world data into actionable insights, sparking my interest in the "why" behind healthcare policy and systems management.
This expertise was solidified during a rotation with Informatics Department Chair, Dr. Michael Grasso, where I created two projects to help narrow the gap between raw data and clinical action. I created the "Cosmos User Guide for the Population Health Research and Informatics Provider" to empower fellow clinicians, and I conducted original research using the robust Cosmos database. My research poster, "Inpatient Admission Risk within 6-12 Months after GLP-1 Initiation Compared With Atorvastatin Among Patients With Atrial Fibrillation and BMI >= 25, An Epic Cosmos Based Analysis," exemplifies how I utilized real-world evidence from over 300 million patients to generate the foundation for future potential actionable clinical insights. By merging these informatics capabilities with my clinical training, I am dedicated to building a future of real-world evidence-based and data-driven care that makes lasting wellness more accessible for everyone.
-Jenny Su PGY 3

Student Spotlight | Medical student perspectives, reflections, and pathways
Movement as Medicine: Prevention Beyond the Exam Room, Nina Kolodgie
February 9, 2026
Movement as Medicine, Prevention Beyond the Exam Room
Prevention starts long before the exam room, and few things illustrate that better than movement. Regular physical activity is one of the most powerful tools we have to improve physical health, mental well-being, and longevity. It reduces the risk of chronic disease, sharpens cognition, and helps us show up more fully for our patients and our communities.
As preventive medicine physicians, being better doctors means bringing our best selves to work. That requires practicing what we preach. Whether it’s carving out time for a walk, a run, or a stretch between meetings, exercise isn’t just something we recommend—it’s something we live.
Maybe we will bump into each other on a jog around Baltimore’s harbor - prevention really is the best medicine.
Below Nina Kolodgie, MS2, shares why she is interested in lifestyle medicine and how physical activity fits in.
-Marissa Khajavi Program Director
I'm excited to be a part of the Lifestyle in Medicine Interest group, especially since my background in college sports and exercise science taught me firsthand how much our daily habits actually drive health and performance. Beyond that, my work with families facing social determinants of health barriers showed me that linking people to key resources is just as crucial for their health as any clinical plan. Together, these experiences—from the swimming pool to resource navigation—have shaped how I think about sustainable health, and I’m eager to bring this lens to supporting patients in achieving lasting improvements in wellness and recovery.
Recently, I took part in the Lifestyle in Medicine Zumba event led by Dr. Koka, a pathology faculty member at UMMC. The event was a fun, energizing reminder of the importance of physical activity, particularly for medical students navigating long hours, heavy workloads, and seasons when getting outside can be challenging. Making time to move helps relieve stress, improve mood, and reinforces exercise as a powerful tool for chronic disease prevention and recovery. Ultimately, physical activity isn’t just about fitness—it’s about building lifelong habits that promote resilience, health, and well-being for ourselves and for the patients we will one day serve.
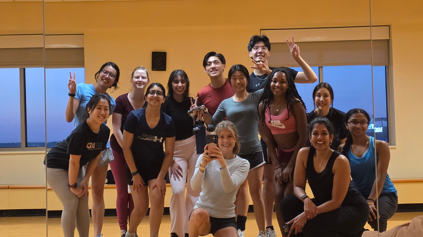
Faculty Features | Preventive Medicine in Practice
Dr. Nadia Saif
February 16, 2026
Faculty Features: Preventive Medicine in Practice
In this Preventive Medicine in Practice, we spotlight Dr. Nadia Saif a UMB Preventive Medicine graduate whose career journey—from residency to the USPHS Commissioned Corps and CDC—illustrates the dynamic and impactful pathways available in public health practice.
-Marissa Khajavi Program Director
I graduated in 2023 from the University of Maryland, Baltimore, Preventive Medicine Residency, completing the MS in Clinical Research and Epidemiology track. After residency, I joined the United States Public Health Service (USPHS) Commissioned Corps and completed CDC’s two-year Epidemic Intelligence Service (EIS) fellowship at the National Institute for Occupational Safety and Health (NIOSH) in Morgantown, West Virginia. I now serve as a medical officer in the Division of Health and Nutrition Examination Surveys at CDC’s National Center for Health Statistics.
During my time with EIS at NIOSH, my work focused on occupational injuries. I analyzed multiple data sources—including national trauma data, emergency department visits, and the National Violent Death Reporting System—to better understand patterns and risk factors for workplace injury and death. In my current role, I analyze data from the National Health and Nutrition Examination Survey (NHANES), which integrates household interviews, physical exams, laboratory testing, and dietary data to assess the health of the U.S. population. My work spans topics such as prescription medication and dietary supplement use, anemia, nutrition, and cardiovascular risk factors.
One of the most rewarding aspects of my work is applying complex survey data methods to answer timely, systems-level questions that draw on my clinical background. I’m continually learning new analytic skills and collaborating with colleagues who share a commitment to protecting and promoting public health.
If I could offer one piece of advice to those entering the field, it would be this: don’t be afraid to take calculated risks. Careers in preventive medicine are rarely linear. Be open to unexpected opportunities, reflect on the impact you hope to make, and pursue paths that align with that vision—even if they look different from what you originally imagined.

From the Desk of Dr. Khajavi
Designing for Flourishing
March 2, 2026
Designing for Flourishing: Reflections from the ACGME “Meaning in Medicine” Conference

Attending the Accreditation Council for Graduate Medical Education (ACGME) conference this year was a time of connection, reflection, and growth. This year's "Meaning in Medicine” conference was a reminder of why our work in graduate medical education matters.
One idea that resonated deeply was that, as physicians, we have a multiplier effect. As teachers and program directors, the impact we have on our residents extends far beyond our direct interactions. They go on to care for thousands of patients, to teach students and colleagues, and to model professional identity for the next generation. The culture we help create today echoes forward in ways we may never fully see.
Our role as faculty is to help residents achieve their full potential. To help them meet that potential, we must create a sustainable, supportive training experience. If our young doctors are thriving—both personally and professionally—then that culture of wellness, balance, and purpose is more likely to carry forward to their trainees and mentees. That is the multiplier effect in action.
I was especially grateful to hear from leaders advancing wellness in medical education, including Dr. Stuart Slavin, Vice President for Well-Being at ACGME. His message challenged us to think beyond environmental stressors alone. While systems absolutely matter, he emphasized that other drivers of stress can include our own thoughts and reactions to situations.
|
Dr. Stuart Slavin, Vice President for Well-Being at ACGME |
One metaphor he shared was the “Stanford duck.” From above the water, the duck appears calm and effortless. Beneath the surface, its feet are paddling furiously. In medicine, many of us are that duck—and we assume others are floating more easily than we are. We fail to recognize that our colleagues may be working just as hard beneath the surface.
Dr. Slavin highlighted three key skills to help address these internal drivers:
- Metacognition – Becoming aware of how we think about our experiences.
- Mindfulness – Anchoring attention to the present moment.
- Self-compassion and cognitive skills – Learning to challenge unhelpful thought patterns and respond to ourselves with understanding rather than judgment.
He also reminded us that cultivating positive emotion does not require grand gestures. Sometimes it can be as simple as pausing to think, “Wow, that burrito I ate today was amazing.” (And trust me—it was. San Diego did not disappoint.) Small moments matter.
Another presentation focusing on wellness was “Developing a Sustainable Approach to Well-Being,” led by Dr. Greg Guldner, Chief Wellness and Retention Officer, and Dr. Jason An, Designated Institutional Official at HCA Healthcare. They shared how they built wellness into a residency program from the ground up—not as an add-on, but as a foundational design principle.
Rather than asking residents to find wellness outside of their already full lives, they asked a different question: How do we intentionally build wellness into the structure of training itself?
Their message reinforced a powerful shift in mindset:
What if wellness didn’t exist outside of our jobs, but was intentionally built into them?
What if our goal shifted from merely reducing burnout to actively helping our learners flourish?
Flourishing is more than the absence of burnout. It is engagement, connection, growth, and meaning. It is designing systems where residents can do meaningful work, feel supported in doing it, and grow into the physicians they aspire to become.
I found my own moments of flourishing at the conference—meeting new colleagues who share a passion for teaching, taking in the views of San Diego, and reconnecting with fellow preventive medicine program directors over tacos. These moments of connection and reflection are not separate from our professional mission; they fuel it.
-Marissa Khajavi
Program Director Preventive Medicine Residency

|
Preventive Medicine colleagues: Dr. Terra Forward (Joint Base Lewis McChord, Washington) and Dr. Bala Simon (University of Arkansas Medical Sciences Little Rock, Arkansas) |
Resident Reflections | Preventive Medicine in Practice
Beyond the Exam Room: A Preventive Medicine Resident’s Journey Upstream, Dr. Maia Tinder
March 9, 2026
Beyond the Exam Room: A Preventive Medicine Resident’s Journey Upstream
Meet PGY-3 resident Dr. Maia Tinder. Dr. Tinder entered our program with an impressive foundation. She completed a combined Internal Medicine–Pediatrics residency at the University of Alabama, graduating in 2023, and is double board-certified in Internal Medicine and Pediatrics. Following residency, she spent one year in clinical practice as a primary care physician at Christiana Primary Care in Pennsylvania, where she further refined her clinical skills prior to beginning preventive medicine training. Maia will graduate from our program this year after which she has accepted a role as a Clinical Professor at Penn Medicine in Philadelphia. Read below to learn why Dr. Tinder chose to pursue Preventive Medicine and how insights from her practicum rotation will shape her future work.
- Marissa Khajavi, MD, MPH
Preventive Medicine Residency Program Directory
I chose to pursue preventive medicine residency after completing residency in internal medicine and pediatrics to deepen my training in public health and develop skills to better address the structural drivers of health. My clinical work made clear that many of the challenges my patients faced—particularly those rooted in inequity—could not be solved through the traditional medical system alone. I came to preventive medicine to learn how to work upstream.
During my rotation with the Maryland Department of Health Maternal and Child Health Bureau (MCHB) during the Maryland legislative session, I saw firsthand how policy shapes the environments in which families live and receive care. When a bill is introduced in the Maryland House or Senate and deemed relevant to maternal and child health or to MCHB operations, it is routed to the bureau for review. I was assigned bills as they were introduced, conducting background research to assess how proposed language and terms aligned—or conflicted—with medical evidence, national recommendations, and existing state initiatives and needs.
I drafted position papers and proposed amendments to provide legislators with clear, evidence-based public health perspectives. This work involved thoughtful synthesis, collaboration with the MCHB team, coordination across other divisions of the department, and engagement with external partners. We followed each bill through hearings and votes, reporting back to the team and refining our approach in real time. The process was dynamic, rigorous, and deeply collaborative.
In the near term, I plan to practice academic medicine in an underserved setting, integrating medical education and equity-focused quality improvement. Long term, I can see myself returning to governmental public health—working to shape the systems and policies that influence health at a population level. This rotation affirmed that advancing health equity requires both clinical insight and policy engagement, and I am eager to continue building skills at that intersection.

Student Spotlight | A Student Perspective on LIfestyle Medicine
Prioritizing self-care in medicine: Sleeping better, Salim Muhammed
March 16, 2026
Prioritizing self-care in medicine: Sleeping better
In our busy lives, sleep is often sacrificed.
Wellness in medicine does not begin with doing more—it begins with restoring what sustains us. When we prioritize sleep, we strengthen our capacity to learn, to lead, and to care.
Below MS 2, Salim Muhammed recognizes the importance of sleep and writes some tips for a better night's rest.
- Marissa Khajavi, MD, MPH
Preventive Medicine Residency Program Directory
For the longest, sleep wasn’t at the top of my list when it came to improving my health. But about 5 years ago, I started to learn sleep’s role in other domains of health–– from cognition, mood, and even disease risk–– and it completely shifted my perspective and practice.
What surprised me most wasn’t just the science behind it or even that 1 great night’s sleep effect, but the consistency factor. Continuously working on my sleep, I started to notice that I was showing up the next day more sharp, focused, and productive. When I get consistently good sleep, I notice it immediately: I retain information better, engage more in conversations, make clearer decisions, and feel more emotionally steady. And doing all of this without the need for caffeine!
For medical trainees and attending physicians, working on this lifestyle medicine pillar, one-step at a time, can allow us to learn efficiently, care attentively, and sustain ourselves in a demanding profession. In a field where we’re constantly asked to give our best to others, sleep is one the most practical and simple (though not necessarily easy) ways we can make sure we give it our best.
I hope this post not only highlights the practice steps to improve sleep but also serves as encouragement. Working on sleep can feel small, but its impact is tremendous acutely and over the long run.
Today we are exploring one of the six pillars of health — Sleep.

Sleep is something pretty much every animal does— whether it’s 3-4 hours, >18 hours, or anywhere between. Its presence across the animal king down tells us it plays an important role. Sleep is important for memory, focus, attention, immune health, mood, and even pain.
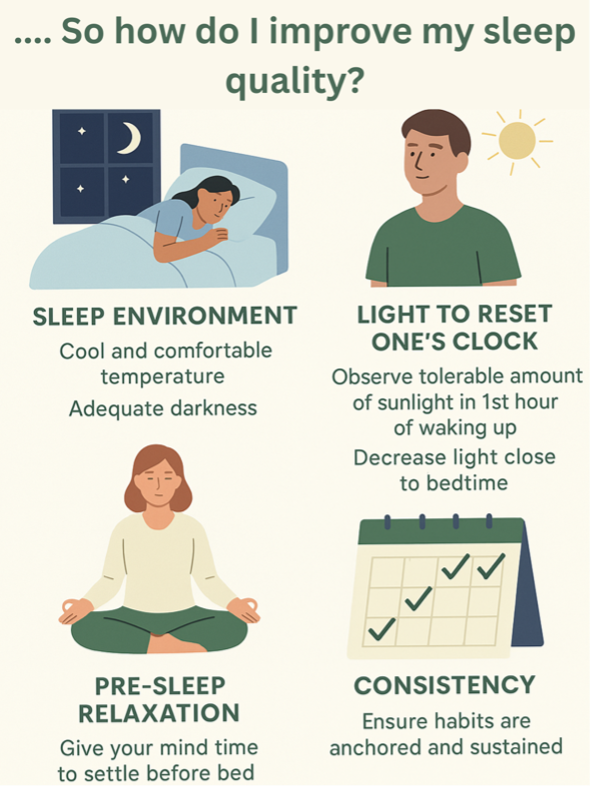
Though sleep quality includes how many hours we’re getting, it also includes how long it takes to fall asleep (latency); how often we wake up at night (fragmentation); and how much of our time in bed is actually spent sleeping (efficiency). Here are some simple ways to support better quality sleep.
Temperature: Our body naturally cools as we prepare for sleep. A cooler bedroom or warm shower couple hours before bed can help reach that relaxed, lower temperature.
Light: Light is the most potent signal (zeitgeber) that synchronizes our internal biological clock with the external environment. Keeping the lights dim in the evening (yes, means less doom scrolling) and getting sunlight within the 1st hour can help set a consistent rhythm over time. Do this enough and we may never need an alarm clock (yep it’s that awesome).
Mindset: Keeping our mind busy makes it difficult to fall asleep quickly. Slow breathing focusing on decreasing rate but increasing our depth of breathing; gentle relaxation methods; or giving yourself time to unwind (no thoughts, just looking up at the sky and counting sheep) can make a difference.
Consistency: Even improving one area and sticking to it can help. Layer other habits once the basics become routine and you’ll see the + ∆ in your sleep quality, and hopefully your other aspects of health.
Faculty Features | Preventive Medicine in Practice
Dr. Jamie Sibel
March 23, 2026
Preventive Medicine in Practice
This blog series spotlights the voices and work of our faculty and graduates who are advancing prevention and population health in meaningful ways. Through personal reflections, mentorship insights, and career narratives, contributors share lessons learned, pivotal moments, and practical advice for trainees and early-career professionals navigating preventive medicine and public health careers.
In this Preventive Medicine in Practice, we feature Dr. Jamie Sibel, a UMB Preventive Medicine graduate, making a big impact at the local public health level.
___________________________________________
I graduated from the University of Maryland Public Health and General Preventive Medicine Residency in 2022 and now serve as the Medical Deputy Health Officer for the Harford County and Cecil County Health Departments. In my dual role, no two days look the same. My work spans both clinical and administrative public health, from overseeing communicable disease investigations and supporting STI and family planning services to collaborating with schools, hospitals, and state partners. I spend a significant amount of time providing guidance and oversight to clinical programs, advising on disease outbreak response, and turning public health guidance into practical action at the local level.
My primary focus areas include communicable disease control, immunizations, reproductive health, and strengthening local public health systems. Much of what I do centers on early detection and rapid response, ensuring timely disease reporting, coordinating efforts during public health threats, and improving access to clinical preventive services. I also incorporate social and structural factors, such as access to care, housing stability, and education, into program planning and partnerships because those realities shape health outcomes just as much as any clinical intervention.
What I find most rewarding is the ability to influence health at both the individual and population levels. Whether helping contain an outbreak, treating a patient, improving a clinical program, or building partnerships that expand access to care, the impact is often preventive and sometimes invisible, which is part of what makes it so powerful. Seeing strong public health infrastructure quietly protect a community is incredibly motivating.
My advice to those entering the field is to stay connected to what originally drew you to preventive medicine and public health. The work can be complex and, at times, bureaucratic due to its governmental nature, but a clear sense of purpose keeps you grounded. When your career aligns with your values and passions, it becomes much easier to navigate challenges and continue advocating for meaningful change.

|
From left to right: Dr. Jamie Sibel, Jennifer Mangold RN (Director of Clinical Health), and Ronya Nassar MPH (Director of Population Health and Public Information Officer) |
|---|
Accomplishments and Milestones
March 30, 2026
Accomplishments and Milestones
We are thrilled to celebrate our PGY-3 resident, Dr. Jenny Su, as she embarks on the next chapter of her medical journey. Dr. Su has matched into the Obesity Medicine Fellowship at Atrium Health in Charlotte, and we could not be prouder of her accomplishments!
Dr. Su is a PGY-3 Preventive Medicine resident at the University of Maryland and a graduate of PCOM‑Georgia in Suwanee, GA. She completed her intern year in Family Medicine, which strengthened her foundation in comprehensive primary care and chronic disease management. Prior to her residency, she also worked with multiple large hospital networks across the United States in Epic clinical informatics, focusing on workflow optimization, reducing documentation burden, and translating real-world data into actionable insights. Her clinical interests include diabetes management, dysautonomia, obesity medicine, and chronic disease prevention, with a particular passion for empowering patients through systems-level innovation and clear, accessible communication.
Following graduation, Dr. Su will begin her Obesity Medicine Fellowship at Atrium Health, where she aims to advance data-driven, patient-centered approaches to treating obesity and related disorders.
Reflecting on her journey, Dr. Su shared:
“My work in informatics led me to learn more about data systems management as well as healthcare systems-level policy and management. Preventive Medicine seemed like a natural fit because it allows me to take a whole-picture view—understanding the why, not just the how.”
“The specialty is far more dynamic than most people realize. It’s not just about guidelines—it’s about redesigning systems, using data intelligently, and creating environments where healthier outcomes become the natural default for entire populations.”
When she’s not diving into data or patient care, Dr. Su loves to explore the world. Now on her third passport, she has filled at least one passport entirely with visas. She enjoys walking, photography, and capturing moments from her travels. One of her recent favorite photos features the iconic Domino Sugars sign illuminating Baltimore Harbor, viewed from a thoughtfully designed gravel beach with fallen wood benches—merging the industrial and natural worlds in a single frame. As the largest marketer of refined sugar in the U.S., it’s a striking symbol of the intersections between industry, environment, and health—a fitting metaphor for her approach to Preventive Medicine.

Resident Reflections | Insights from preventive medicine residents on training, practice, and professional growth
Service Learning at Stillmeadow PeacePark, Dr. Ike Enenmoh
April 6, 2026
Resident Reflections
Some of the most meaningful experiences in my career and medical training so far have happened outside of the hospital or clinic walls, immersed in community and learning what it means to care for people in the context of their lives and their familiar environments. This is a large part of what drew me to Preventive Medicine; I wanted to develop and cultivate the skills necessary to meaningfully improve health on the community and population level in the places I care so much about. What I’ve been grateful to understand by living and learning in Baltimore City is how so many grassroots community organizations, neighborhoods, and faith leaders and congregations have been practicing community health on their own by understanding local needs and working to address them directly. The Stillmeadow Community Fellowship and PeacePark in West Baltimore is no different, and that is part of what makes our program partnership with them so special.
As part of the MPH portion of our program, to strengthen our foundations in public health, we take part in what is called service learning. Although we may not have known what to call it, for many of us who find our way to Preventive Medicine, service-learning often plays a large role in how we’ve learned how to partner, communicate with, and show up for the communities we serve. Service-learning broadly describes educational experiences structured around intentional community service and grounded in reflection, reciprocity, and active engagement. As learners, we began our service-learning experience with Stillmeadow after being introduced to their 10-acre Urban Forest and PeacePark in West Baltimore during a class trip (if you have a chance to visit or volunteer on the 1st and 3rd Saturday of each month to see it for yourself, they’ve stewarded a beautiful piece of land and I highly recommend!). During this experience, we gained a glimpse of the various operations taking place at the PeacePark, from their learning center and flood prevention programs, to their community and pollinator gardens, all while being taught by and getting to know Pastor Michael and the incredible youth leaders who have helped steward the land at Stillmeadow. These same youth leaders helped us get to the service part of the learning, which for us meant getting our hands dirty identifying poison ivy, and removing invasive plant species in the gardens to ensure that ecosystems of native plants at the park would be able to thrive in the coming seasons.
We later expanded this experience by interviewing the various partners that have helped Stillmeadow cultivate their beautiful PeacePark over the last several years and writing their profiles to go on Stillmeadow’s website. Our group profiled the Smithsonian Environmental Research Center and learned how their partnership has leveraged environmental research to realize Stillmeadow’s educational goals. These experiences made it much more meaningful when our program joined Stillmeadow in celebrating the 5th anniversary of their PeacePark this past October. One of the things I’ve appreciated most about this service-learning experience is how it takes us out of the classroom to ground our education in the lives of the real people we serve, making the walls of the university more porous through direct engagement and mutuality. Both the partner profiles and the 5th anniversary celebration also highlighted how important collaboration is, sometimes across the local, city, and state levels, in realizing lasting public health goals. Stillmeadow has been able to steward an incredible long-term endeavor that feeds, protects, and educates the surrounding community by building a network of intentional collaboration and I’m grateful that through this program, we get to learn from and contribute to that.
Click here to learn more about Stillmeadow PeacePark
 Pictured far left: PGY 2 residents Dr. Ike Enenmoh and Dr. Gabriel Sanz
Pictured far left: PGY 2 residents Dr. Ike Enenmoh and Dr. Gabriel Sanz
Student Spotlight | Medical student perspectives, reflections, and pathways
Plant-Based Diets for Chronic Disease Prevention, Jennifer Paul Quinn
April 13, 2026
Student Spotlight: Medical student perspectives, reflections, and pathways
In preventive medicine and lifestyle medicine, nutrition is central—we are taught to address root causes of disease and to use evidence-based dietary patterns as a foundation for health. As rates of conditions like cardiovascular disease, diabetes, and obesity continue to rise, nutrition offers a practical, effective approach to improving population health. In Blog Post 13, we highlight the concept of food as medicine, featuring MS-3 Jennifer Paul Quinn, a registered dietitian who shares her experience incorporating nutrition in her life and practice.
-Marissa Khajavi, MD, MPH
Plant-Based Diets for Chronic Disease Prevention
From a public health perspective, dietary patterns represent one of the most powerful modifiable risk factors for chronic disease and one of our greatest tools for population-level disease prevention. Optimal nutrition is one of the six pillars of lifestyle medicine and is essential to addressing the root causes of chronic disease. Organizations such as the American College of Lifestyle Medicine (ACLM) promote evidence-based plant-forward nutrition as part of comprehensive chronic disease prevention. ACLM recommends an eating pattern centered on a variety of minimally processed vegetables, fruits, whole grains, legumes, nuts, and seeds.
A growing body of research demonstrates that whole food, plant-based dietary patterns are associated with lower risk of chronic diseases, including cardiovascular disease, type 2 diabetes, hypertension, obesity, chronic kidney disease, and certain cancers. Plant-based diets are effective in optimizing key cardiometabolic risk factors for these diseases. Evidence from meta-analyses of both observational studies and clinical trials demonstrates that plant-based diets are associated with and improve risk factors, including blood pressure, total and LDL cholesterol, body mass index, body weight, and hemoglobin A1c.
These benefits are driven in part by overall diet quality. Whole food, plant-based diets are higher in dietary fiber and antioxidants, and lower in saturated fat, cholesterol, and processed foods. They are also anti-inflammatory, lower in energy density, and support a more favorable gut microbiome. Collectively, these mechanisms support the role of plant-based nutrition as a therapeutic tool to prevent disease and improve health and longevity in our patients.
My Personal Plant-based Lifestyle
I became vegan over 12 years ago after discovering the health benefits of plant-based diets and their role in disease prevention. Over time, and especially in recent years as a busy medical student and mom of two young children, I have found it increasingly important to prioritize self-care, including maintaining a healthy diet. Eating in a way that emphasizes whole plant foods allows me to support my own long-term health while also reinforcing the same evidence-based principles I encourage in patient care. As a future family medicine physician who understands food as a foundation of health, I plan to incorporate lifestyle and preventive medicine into my practice. Living the principles that I teach grants me greater insight into the challenges and opportunities patients face when making lifestyle changes.
Learn More and Try it Out!
As future providers, understanding how nutrition shapes health outcomes is an essential part of patient care. For medical students interested in learning more, educational resources and courses are available through ACLM. I would recommend the following courses, which are free for ACLM members:
1. Lifestyle medicine essentials course bundle
2. Lifestyle Medicine Fundamentals: Framework for Success
There are also several great conferences you can attend:
● International Conference on Nutrition in Medicine
● Plant-based Prevention of Disease Conference
● Lifestyle Medicine Conference
● Preventive Medicine Conference
My background as a dietitian has shown me firsthand how the way we approach food shapes both our personal health and our ability to care for patients. I encourage medical students to explore integrating plant-predominant eating into their own lives. We spend years learning about taking care of patients, but we should also learn to care for ourselves! It can also help us better understand the changes we often ask our patients to make. Aligning our habits with the principles we promote strengthens our credibility and enhances our effectiveness as clinicians.
Faculty Features | Preventive Medicine in Practice
Dr. Cara Dooley
April 20, 2026
Faculty Features: Preventive Medicine in Practice
This blog series spotlights the voices and work of our faculty and graduates who are advancing prevention and population health in meaningful ways. Through personal reflections, mentorship insights, and career narratives, contributors share lessons learned, pivotal moments, and practical advice for trainees and early-career professionals navigating preventive medicine and public health careers.
In this Preventive Medicine in Practice, we feature Dr. Cara Dooley, a UMB Preventive Medicine 2023 graduate, who applies her clinical and epidemiologic expertise to lead her work in pharmacovigilance at the FDA. Dr. Dooley offers practical advice to students and current residents based on her own experience in the field.
-Marissa Khajavi, MD, MPH
I graduated from Maryland's preventive medicine program in 2023. I currently work at the U.S. Food and Drug Administration as a medical officer. In my position, I perform public health surveillance called pharmacovigilance and manage a portfolio of products. I review protocols, clinical data and study results as well. I consider my role to be a well-balanced combination of both my medical knowledge and epidemiology skills. I use a variety of data systems and my work products are written reports, memos and presentations. I work in a team but my assignments are mostly independent. I find my work to be interesting, meaningful, and rewarding.
My advice for someone interested in the field of preventive medicine is to take any opportunities to network and learn about different paths within preventive medicine and public health. Other preventive medicine graduates are a great resource, if not the best available resource. A phone call as a medical student or resident may lead to a job opportunity later - I can attest to this.
As you do this, try to understand yourself and your goals as well as possible: what skills do you like to use and what kind of environment do you want to work in. I leaned into my epidemiology skills, for instance, but you may like program administration, policy, or other areas of public health.
Public health and preventive medicine are broad fields. Although you may find that potential employers are less familiar with your specialty, as a preventive medicine physician, you have many unique skills and experiences that make you stand out. Remember to sell your strengths. Some uncertainty is normal, especially when looking for your first position but trust the process! If you do your homework, you will find a path that suits you. That's what others told me, and I found it to be true.

Accomplishments and MIlestones
Turning Communication & Creativity into Public Health Impact, Erika Shook
April 27, 2026
Accomplishments and Milestones: Turning Communication & Creativity into Public Health Impact
In this Accomplishments and Milestones blog post, we are proud to celebrate Erika Shook, a dual-degree MPH and Social Work student, as she approaches graduation in just one month. During her time in the program, Erica has demonstrated a strong commitment to advancing public health and social impact, drawing on her background in advertising, public relations, and communications to bring creativity and innovation to her public health work.
Within our Preventive Medicine Residency Program, residents complete their MPH alongside students like Erika, fostering close collaboration and lasting professional relationships within the MPH cohort. Our faculty are engaged in teaching and mentoring MPH students, further strengthening these connections and enriching the learning environment. We recognize the dedication, creativity, and growth that have defined Erika’s journey, and we look forward with excitement to all that lies ahead. We invite you to read Erika’s reflection as she shares insights from her experience and the path that brought her to this important milestone.
-Marissa Khajavi, MD, MPH, Director
Preventive Medicine Residency Program
My Pathway to my MPH at the University of Maryland, Baltimore
Coming from a background in advertising, public relations, and communications, I never anticipated a path to a career in public health. When I landed my job at the University of Maryland School of Social Work as a public relations specialist, I figured I would be working in traditional media and pitching press releases. To my surprise, I was doing communications for research projects in men’s mental health, suicide prevention, and opioid recovery. With support from my principal investigators and research colleagues, I was able to integrate my creative skills into public health communications that would support community partnerships, develop a wide range of creative materials to translate research into action, and collaborate with experts in the field.
Because of my exposure to behavioral health research at the School of Social Work, I wanted to learn more about what went into the interventions we create and evidence-based practices we support. I cared deeply about the communities that we work with and wanted to learn how I can further make a positive impact. In 2023, I began my MPH at the University of Maryland School of Medicine.
While I wish I could reflect on everything I did during my program, I would like to highlight a few of my accomplishments that I am most proud of.
National Academy of Medicine DC Public Health Case Challenge 2024
Each year, the National Academy of Medicine hosts a public health case challenge in Washington, D.C., where local university students are tasked with solving an emerging public health issue. Universities form small teams of interdisciplinary students and are given a case to develop an intervention within two weeks and present to a panel of expert judges.
During the year I participated, we had to work on a case study to address substance use and mental health concerns among emerging adults in the DMV area. Our team had four students representing public health, social work, law, and medicine. With my background in communications, coursework in public health, and work in mental health and substance use research, I knew I would be a great support to our team in developing an effective intervention. While I can say this time might have been the most stressful two weeks of my life, having to juggle school, work, and stress, I am extremely proud of the intervention we developed.
Our intervention titled, “Guiding Resilience and Offering Wellness (GROW) at Community College,” focused on DC community college students with a three-pronged approach. Utilizing a wellness leadership workshop and certification program, case management team, and Interactive Screening Program, our intervention met community college students where they were and addressed upstream, mid-stream, and downstream prevention approaches.
Our intervention was backed with supporting data, describing the need to focus on community college students and tailoring interventions that fit their lifestyles. Our presentation was comprehensive, understandable, and engaging, so that audiences, no matter the background, could understand the “why” behind our work.
With hard work and dedication from all my teammates, we were awarded the 2024 grand prize.
Delta Omega Student Poster Session at the American Public Health Association (APHA) Annual Meeting & Expo 2025
In 2025, I was selected to present my poster for the Delta Omega Student Poster Session at APHA. My poster, “Utilizing High-Tech and High-Touch Methods to Engage Men in Suicide Prevention Through a State-Wide Mental Health Campaign,” demonstrated my work at the School of Social Work where our research team is implementing a free men’s mental health intervention in the state of Ohio. I was able to present about our public health campaign, our successes, and best practices.
This was my first time being a first author and presenting a poster at a conference. I was proud of myself that I wrote an abstract and developed a research poster. This was also my first APHA experience. It was really amazing to be able to attend a conference that had such a diverse amount of interesting topic areas where I got to meet many like-minded professionals and learn about new research.
I would like to thank our school’s chapter, Beta Tau, the national honor society, Delta Omega, and everyone in our MPH program who made this possible.
MPH Practicum Experience at the UMB Community Engagement Center Health Suite
Since mainly working in an office setting, I knew I wanted to get into the community and do hands-on public health work. This led me to my practicum at the UMB Community Engagement Center (CEC) Health Suite. Located in West Baltimore, the CEC is a central place where community members can access a variety of programming such as fitness classes, workforce development, art classes, financial services, health and wellness support, and more.
More specifically, the Health Suite takes a holistic approach and works with community members on their health goals and helps address the social determinants of health. Led by nurses, the Health Suite offers care management, health education, screenings and assessments, provider referrals, and connections to local support.
I worked on two projects during my time at the Health Suite: the development of a student community outreach guide and the creation of a nutrition program facilitator guide.
As the Health Suite helps address the social determinants of health, volunteer medical and nursing students support the Health Suite by engaging in community outreach to support the community with resources and programming provided by the CEC. As students may be new to community outreach, I developed a guide that will help prepare students before they engage in outreach. Creating processes for before, during, and after outreach will help ensure consistency across cohorts of students. One of my favorite parts of the guide I developed is a role-playing scenario section, where students can practice presented scenarios of engaging with neighbors and what resources to offer that will provide the best support for individuals they meet. I am excited for the Health Suite to be able to implement this guide with incoming students.
The second project I worked on was creating a facilitator guide for a nutrition education program, the “Healthy Food Shopping” class. Taught by medical residents, this class teaches community members about healthy eating and how to shop for those options at the grocery store. The class also includes a trip to the local grocery store with a voucher to shop. From existing curriculum, I revamped the content to be engaging and community responsive. Covering topics such as MyPlate, portion and serving sizes, nutrition labels, and healthy substitutions, I added hand-on classroom activities and developed a take-home resource packet to reinforce what is learned. The guide also includes a script for facilitators to teach from. With what I have created, the plan is for the program to be implemented starting this summer.
Plans After Graduation
After reflecting on MPH journey, I extended my deepest appreciation and gratitude to my professors, administration (Dr. St. George, Dr. Jones, Ms. Longo, and Ms. Manning), classmates, colleagues at School of Social Work (Dr. Jodi Frey and Amanda Mosby), practicum preceptor (Dr. Kelly Doran), friends, family, and everyone who cheered me on during this time.
Everything I have learned in and outside the classroom has prepared me for a career in public health, I hope to pursue a career in health education or health communications, where I can uplift our communities and support the health and well-being of those around us.

Resident Reflections | Insights from preventive medicine residents on training, practice, and professional growth
A Different Kind of Classroom, Dr. Gabriel Sanz
May 4, 2026
Resident Reflections: A Different Kind of Classroom
University of Maryland Preventive Medicine resident PGY-2 Dr. Gabriel Sanz reflects on an educational experience that challenged many of his long-held assumptions about advocacy, health disparities, and systems change. Through the MPH Health Equity and Social Justice course (taught by Dr. Lori Edwards), he took part of immersive learning. Read Dr. Sanz’s thoughtful reflection post below.
-Marissa Khajavi, MD, MPH, Director
Preventive Medicine Residency Program
Starting as far back as Model UN in high school, I have always been the person in the room complaining about the system. I’ve spent my academic and professional career caring deeply about social justice and being an advocate whenever possible. Naturally, I thought I was well-versed in the subject. I thought I had the vocabulary and the insight to explain how these systems work and why they fail our patients.
It turns out I was a classic victim of the Dunning-Kruger effect; the cognitive bias where limited knowledge of a subject makes one overestimate their own competence.
As a preventive medicine resident completing my MPH at the University of Maryland, I took a course called Health Equity and Social Justice led by Dr. Lori Edwards, Associate Professor and Associate Dean at the UMB School of Nursing. Dr. Edwards is very active outside of academia and uses her extensive experience engaging with the community to design the curriculum. The course didn’t just fill a few gaps in my knowledge; it showed me how the health disparities we see are part of a problem significantly larger, deeper, and more calculated than I ever realized.
The Hybrid Approach
This class forgoes the standard lecture format. Instead, Dr. Edwards created a hybrid, highly participatory experience. The first few lectures focus on core concepts and historical context and rely heavily on students sharing their experiences. This is followed by a variety of guest speakers who come in to share how they are actively contributing to equity in their respective fields. It moves the conversation from abstract theory to the concrete ways social justice can be practiced on the ground.
Beyond the classroom, one of our key experiences was a walk through the city with Johns Hopkins. Mr. Hopkins is the director of Baltimore Heritage, a nonprofit organization dedicated to saving historic buildings and revitalizing neighborhoods. As someone who has driven through the city countless times, it dawned on me that I had never stopped considering the rich history of the area.
I felt a sense of embarrassment realizing how little I knew about the history of redlining and the specific systemic mechanisms that were put in place to cement racial disparities in Baltimore. Perhaps because I was not born or raised here, I neglected to learn some of the most impactful historical precedents to the larger inequities we see today. It highlighted the importance of learning from and engaging locally with the community before attempting to make state or nationwide changes.
Looking Ahead
The course goes far beyond the surface level. It explores the massive impact of social capital on health outcomes while offering achievable solutions. Though I often feel cynical about the prospect of enacting any real change, seeing community leaders showcase their success transformed much of my frustration into hope.
Ultimately, I believe that this type of immersive learning offers a huge benefit for any healthcare professional, regardless of their career stage.

Baltimore Love Mural, by Michael Owen
Accomplishments and MIlestones
MPH Poster Day, Dr. Marissa Khajavi
May 11, 2026
Accomplishments and Milestones: MPH Poster Day
Spring is always an exciting season in our residency program. It is a time of new beginnings as we welcome a new class of residents into the program while also celebrating the next chapter for our graduating PGY-3 residents. This time of year is both joyful and bittersweet, and it is a reminder of just how quickly these years pass.
Over the course of their residency, I have had the privilege of getting to know Maia, Gabe, and Jenny not only as residents, but as individuals. I have watched their growth, resilience, and personal development as they progressed through the residency and MPH program. Every course, assignment, clinic experience, and practicum opportunity served as another building block in shaping them into the thoughtful and skilled public health professionals they are today.
As graduation approaches this week, I find myself reflecting not only on their accomplishments, but also on the many people who helped guide them along the way. I think about the faculty, mentors, and staff throughout the Department of Epidemiology and Public Health and the Division of Preventive Medicine who contributed to their education and growth. I think about the physicians and teams at the University of Maryland Medical Center and the Baltimore VA Medical Center, as well as the dedicated preceptors at their public health practicum sites. Their journeys have been supported by an incredible community of educators, colleagues, and mentors who invested their time, knowledge, and encouragement into these residents.
As a graduate of this program myself, I understand firsthand the profound impact that support system can have. Now, as Program Director, I am deeply grateful to everyone who continues to support and mentor our residents and students throughout their training. The strength of the preventive medicine pipeline depends on these collective efforts to educate, inspire, and prepare the next generation of public health leaders.
This past Thursday, May 7, we also celebrated the MPH Poster Session, where students presented the projects they completed during their practicum experiences. It was a wonderful opportunity for students to share their work with the faculty, mentors, and peers who have supported them throughout the process. To all of the faculty members who attended and engaged with students about their projects, thank you for your continued encouragement and investment in their success. I would especially like to recognize Dr. Ann Gruber-Baldini, Dr. Jessica Brown, Dr. Carrie Wolfson, and Dr. Sania Amr for serving as poster judges and helping make the event such a meaningful experience for our students. Thank you to MPH Director Dr. Diane Marie St. George for your steadfast leadership and dedication to teaching, and to Department Chair Dr. Andreea Creanga for fostering and uplifting a strong culture of mentorship within our department.
Looking forward to celebrating our students and all their accomplishments at graduation this week, while cheering them on as they begin the next chapter of their careers!
Left to right: Dr. Maia Tinder (PGY-3), Dr. Marissa Khajavi, Dr. Jenny Su (PGY-3), and Dr. Gabriel Pontipiedra (PGY-3)
Dr. Shivakumar Narayanan

Erika Shook
Faculty Features | Preventive Medicine in Practice
The City as Teacher: Exploring How Baltimore’s Past and Present Shape Health, Dr. Mariss Khajavi
May 18, 2026
Faculty Features | Preventive Medicine in Practice
The City as Teacher: Exploring How Baltimore’s Past and Present Shape Health
As the Community and Population Health Track Chair for the American College of Preventive Medicine conference, I had the opportunity to create and lead an interactive walking workshop titled The City as Teacher: Exploring How Baltimore’s Past and Present Shape Health. Designed as an immersive learning experience through downtown Baltimore, the workshop explored how the city’s history continues to shape present-day health outcomes and offered participants a chance to engage directly with the social and structural factors that influence community health. We were fortunate to have along Dr. Lori Edwards to join us as a community expert, lending her insight and expertise throughout the tour. One of my favorite parts of the experience was seeing our preventive medicine residents' step into the role of tour guides and educators—bringing Baltimore’s history and public health story to life. Keep reading to see which superlative award they were given at the end of the tour.
Throughout the tour, we saw how Baltimore’s identity as the “City of Firsts” reflects a history of innovation, growth, and resilience—but also how that same history has shaped present-day health outcomes.
From the Inner Harbor and port, learners explored how Baltimore’s early success as a shipping and industrial hub created opportunity and population growth while also contributing to environmental exposures that continue to impact community health today. Along Pratt Street and Camden Yards, discussions centered on how conflict—from the Revolutionary War to the Civil War—helped shape Baltimore as a critical American city, while reminding us that violence and instability leave lasting effects on communities.
At Davidge Hall and surrounding institutions, participants reflected on Baltimore’s extraordinary leadership in medicine and public health innovation, including the roots of preventive medicine education and the city’s role in advancing medical training. At the same time, the tour highlighted an important lesson: world-class healthcare institutions do not automatically guarantee equitable access, utilization, or outcomes.
Near the Bromo Seltzer Tower, learners discussed industrialization and the Great Baltimore Fire of 1904, examining how rebuilding efforts transformed the city while leaving lasting environmental health impacts tied to chronic disease.
At the MLK corridor and near the R Adams Cowley Shock Trauma Center, the group examined the enduring impact of redlining and segregation. Participants reflected on how housing policy, disinvestment, and structural inequities continue to shape differences in education, safety, chronic disease, trauma exposure, and life expectancy across neighborhoods only miles apart.
At Westminster Hall and Burying Ground, learners reflected on how far public health has advanced—from a life expectancy in the 40s during the 1800s to today—while recognizing that not all communities have benefited equally from these improvements.
The tour also explored the lasting impact of structural racism and medical mistrust through stories such as Henrietta Lacks, the 1968 and 2015 uprisings, and the opioid epidemic. These conversations highlighted how racism, inequity, and ethical failures continue to influence trust, opportunity, and health outcomes today.
The experience concluded at Lexington Market and we stood before a powerful piece of art called Robert and Rosetta, commemorating enslaved people who were sold at the market, including Rosetta as listed in the historical record, a stark reminder that human beings were once treated as property in this space and denied their humanity; more recently, the 2015 death of Freddie Gray in Baltimore following severe injuries sustained in police custody brought national attention to issues of police brutality, systemic racism, and inequity, and sparked citywide protest and renewed framing of these harms as urgent public health concerns.
Learners also discussed community-driven solutions such as Baltimore’s Safe Streets program and reflected on how meaningful progress in public health must be rooted in partnership, prevention, and community strength. More than anything, the tour reminded us that preventive medicine extends far beyond clinics and hospitals. Public health lives in neighborhoods, housing, transportation, policy, history, and trust. Baltimore’s story continues to shape the future of health equity—and our learners left inspired to be part of that work.
Throughout the conference, it was refreshing to see researchers, physicians, and hospital system leaders discussing their work to address and advance many of the issues highlighted throughout the tour. This included a plenary titled “At the Crossroads of Housing, Harm Reduction, and HIV: Lessons from Baltimore,” featuring panel speakers Baltimore City Commissioner of Health Dr. Michelle Taylor, MD, DrPH, MPA, and Associate Professor at University of Maryland school of nursing Dr. Marik Moen, PhD, MPH, MSN, RN. Another plenary, “Building Trust and Public Confidence in Turbulent Times,” featured Dr. Tiffany Wiggins, MD, MPH, FACOG, Vice President and Chief Health Impact Officer at the University of Maryland Medical System, who spoke about the importance of strengthening trust and advancing health equity within our hospital systems and communities.
Baltimore’s story is still being written. And as preventive medicine physicians, public health professionals, and community leaders, we all have a role in shaping what comes next.
And now onto the resident tour guide superlatives:
• Dr. Jenny Su— Best Dressed Award for effortlessly bringing style to the streets of Baltimore.
• Dr. Gabriel Sanz — Cool, Calm, and Collected Award for staying poised and steady through every stop on the tour.
• Dr. Ikechukwu Enenmoh — Future Professional Tour Guide Award for taking the role so seriously and proving that his voice was made for a microphone.
• Dr. Maia Tinder — First to the Finish Line Award for leading the pace from start to finish aka gets it done.
• Dr. Gabriel Pontipiedra — Most Personal Touch Award for enriching the experience by connecting the tour stops to his own lived experiences and reflections.

Tour Group

Workshop and Tour Team

Dr. Edwards sharing her hope picture of Baltimore

Pictured middle: Dr. Marik Moen and far right: Dr. Michelle Taylor

Far right: Dr. Tiffany Wiggins