Search
1-20 of 41 results with category "Infectious Disease"
Intraabdominal infections leading to sepsis can come from cholecystitis, small bowel perforation, gastric perforation, left sided colonic diverticulitis, right sided diverticulitis and appendicitis. When to initiate source control and antibiotics is controversial. These authors propose breaking patient populations into three groups:
- Class A Healthy patients have no or else well-controlled comorbidities, and no immunocompromise, so that the IAI is the main problem.
- Class B Patients with moderate comorbidities and/or moderate immunocompromise are at risk of adverse outcomes due to their predisposing conditions, but are currently clinically stable. However, the IAI could rapidly worsen the prognosis.
- Class C Patients with severe comorbidities with advanced stages and/or severe immunocompromise, in which the infection worsens an already severe clinical condition.
From this they propose algorithms to treat these intraabdominal infections such as (note the different approach to right and left diverticulitis):
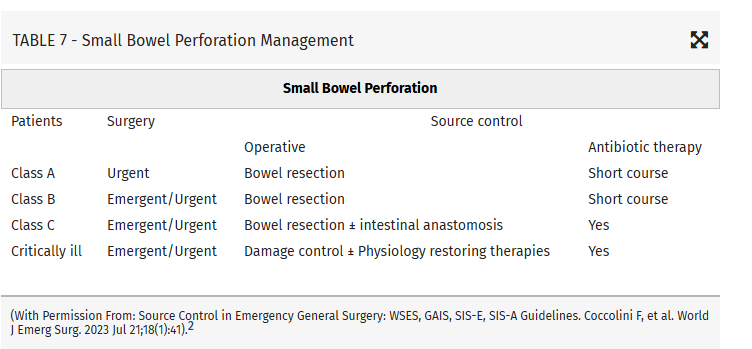

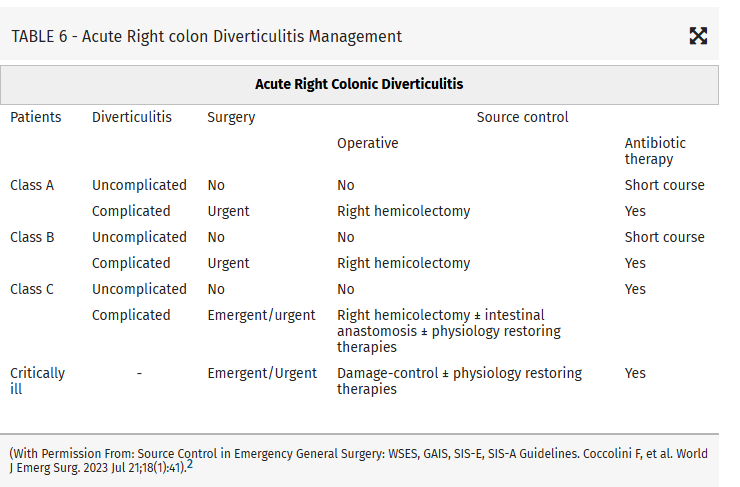
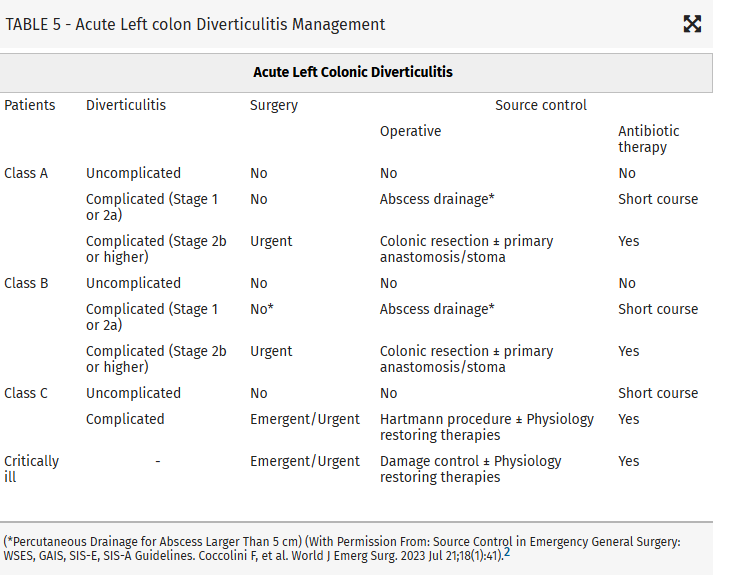
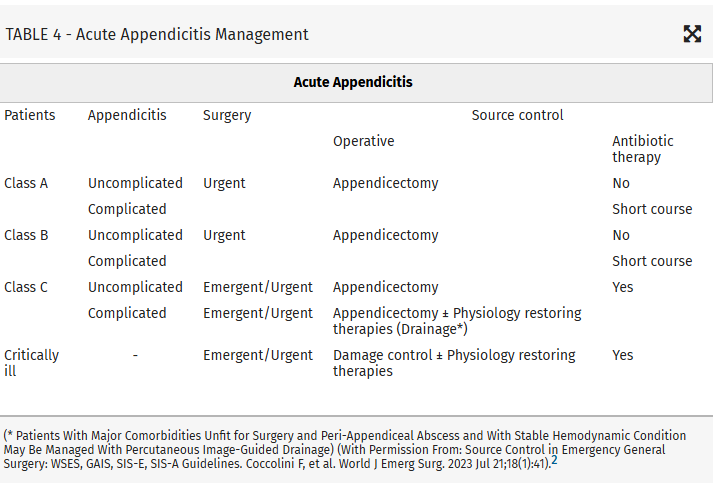
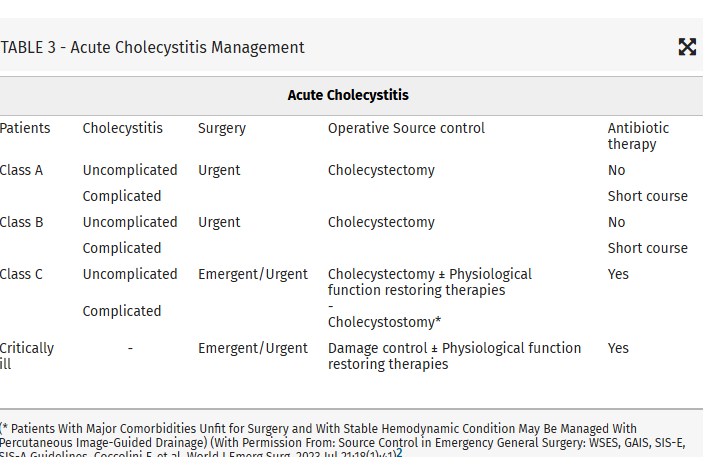
Show References
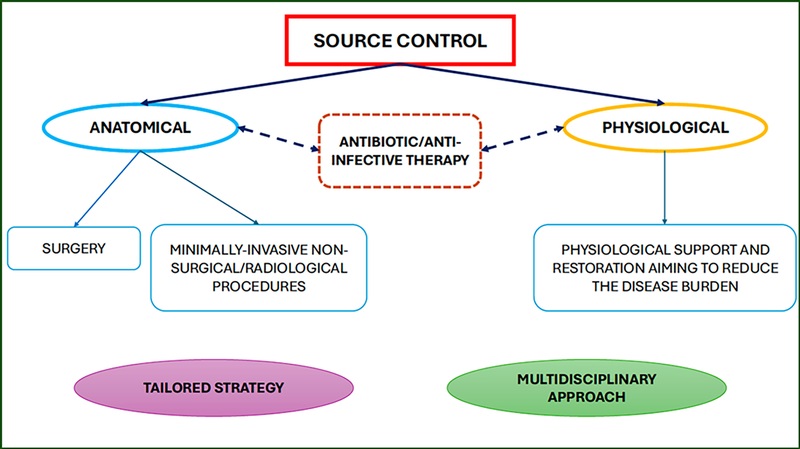
This article looks at source control as it relates to intrabdominal sources for sepsis. Key take aways are:
- They believe surgery is the best service to mange these complex patients in consultation with medicine, heme-onc, transplant, EM, etc. (Is that how it is done at your institution?)
- Source control should be both anatomic as well as physiologic (below)
- Timing of source control is controversial
- Antibiotic stewardship is still important even in these complex patients
Those at high risk of morbidity and mortality from intraabdominal infection associated sepsis include:
Mild–moderate immune deficiency: Elderly (according to the age and general status of the patient), Malnourished, Diabetic, Burns, Trauma, Uremic, Active malignancy, not on chemotherapy, HIV with CD4+ count >200/mm3, Splenectomized, Severe immune deficiencyAIDS HIV with CD4+ count <200/mm3, Transplant (solid organ, bone marrow), High-dose steroids (more than 20 mg/day prednisone), Malignancy on chemotherapy, Neutrophil count <1,000/mm3
High-risk population (medical or surgical causes)Low serum albumin concentration Older age Obesity Smoking Diabetes mellitus Ischemia secondary to vascular disease or irradiation Prolonged or delayed/late procedures
Show References
Treatment of Staphylococcus aureus bacteremia has traditionally required several weeks of intravenous antibiotics. This approach carries medical risks, such as catheter-associated infection or thrombosis, as well as significant social and financial burdens for patients. Dalbavancin, a long-acting intravenous lipoglycopeptide with activity against S. aureus (including MRSA), has been proposed as a more convenient alternative. This study evaluated the efficacy and safety of dalbavancin compared with standard therapy for S. aureus bacteremia.
Two hundred adults were enrolled in this open-label, randomized clinical trial, which was conducted in the United States and Canada. After blood cultures cleared, participants were randomized to complete therapy with dalbavancin (administered on Days 1 and 8) or with standard treatment (cefazolin for MSSA and vancomycin or daptomycin for MRSA).
The primary outcome was the Desirability of Outcome Ranking (DOOR) at Day 70, incorporating five domains: clinical success, infectious complications, safety events, mortality, and health-related quality of life.
Dalbavancin was not superior to standard therapy for treating S. aureus bacteremia, and adverse events were similar between groups. A key strength of this study was the inclusion of people who inject drugs, a population at high risk for S. aureus bacteremia and often underrepresented in trials. A major limitation was that the DOOR metric did not account for important social and economic factors, such as disposition (home versus skilled nursing facility), caregiver burden, or treatment cost.
Key Takeaway: Dalbavancin may be a suitable alternative to traditional therapy for Staphylococcus aureus bacteremia, offering less frequent dosing and a shorter treatment course. Further research is needed to identify which patients benefit most and to evaluate its impact on social and economic factors such as discharge disposition, caregiver burden, and treatment costs.
Show References
In a Danish study of 558 patients with a brain abscess, those that had early surgical drainage did better than those treated conservatively with antibiotics only. Prompt neurosurgical consultation is warranted for these patients.
Show References
Typically Coccidioidomycosis is seen in the Southwestern US. The authors of this study, using climate modeling predict endemic areas will spread across the US to include Idaho, the Dakotas, Nebraska and Wyoming.
Clinically, “Patients with pulmonary Coccidioides infection frequently experience fever, cough, and shortness of breath. Chest radiographic imaging may demonstrate lobar, segmental, or multifocal consolidations; cavitary lesions; and lung nodules. Given these nonspecific findings, patients with coccidioidomycosis are often treated for community-acquired pneumonia. Coccidioidomycosis should be considered in patients not improving with antibiotic treatment or in those who have exposure to or reside in endemic areas. Up to 50% of patients with pulmonary coccidioidomycosis have erythema nodosum, approximately 25% to 30% have peripheral eosinophilia, and approximately 25% have arthralgias (particularly symmetric knee and ankle arthralgia). Up to 10% of patients diagnosed with coccidioidomycosis develop disseminated disease, including skin, central nervous system, and bone and joint infection.”
Show References
In the April edition of Annals of EM, there are opposing view points on the optimal antibiotic regiment for necrotizing soft tissue infection. One group proposes linezolid alone will cover all the worrisome pathogens namely group A Strep and Staph. There are less side effects including C. Diff infection with this medication. Another group suggests sticking to vancomycin plus/minus BLactam along with clindamycin. Their arguement centers around clindamycin is useful as an antitoxin more so than its antibacterial property.
Both offer reasonable evidence and neither is compelling enough to say one is superior to the other.
Show References
The Jarisch-Herxheimer reaction (JHR) is a non-specific set of symptoms (fever, malaise, worsened rash, hemodynamic instability, leukocytosis) seen after treating syphillis and other spirochete induced infections. In this study 1 in 4 patients treated with 2.4 million units of benzathine penicillin G developed a short lived JHR. Those who developed the reaction were more likely HIV negative, had secondary syphillis and had successful treatment at 6 months.
Show References
Risk factors for necrotizing soft tissue infections include: obesity, diabetes mellitus, peripheral vascular disease, immunosuppression, injection drug use, and deep traumatic wounds.
“Any anatomical site can be involved, but the most common sites are perineal, anorectal, foot, or lower extremities.”
Show References
These infections remain difficult to diagnose early and early diagnosis is key to limiting morbidity and mortality.
“The classic clinical signs and symptoms are rarely all present especially in early disease. Crepitus or gas in the soft tissues, while specific, is only present in approximately 10% of patients. More often, the presenting symptoms are nonspecific: fever, pain, induration, and edema. Pain out of proportion to examination is a more specific finding that may assist in differentiation of NSTI from cellulitis.”
Show References
By Bobbi-Jo Lowie, MD
Assistant Professor
Emergency Medicine
University of Maryland School of Medicine
Since April of 2024 there have been 36 confirmed cases of avian influenza A across the United States. Avian influenza, primarily caused by influenza viruses that infect birds, can pose significant health risks to both animals and humans. The most notable strains include H5N1 and H7N9, with H5N1 being particularly alarming due to its high mortality rate among infected humans. The virus primarily spreads from birds to humans through direct contact with infected birds, their droppings, or contaminated environments. Although there have been recorded cases of human-to-human transmission, this usually occurs only in close-contact situations.
In humans, avian influenza can present with symptoms ranging from mild respiratory illness to severe pneumonia. Patients may experience fever, cough, sore throat, muscle aches, and in severe cases, gastrointestinal symptoms. Those that have more moderate or severe illness may develop shortness of breath, altered mental status, or seizures. Complications include acute respiratory failure, pulmonary hemorrhage among others, with respiratory failure being the most common cause of death in this patient population.
Diagnosing avian influenza involves a combination of clinical presentation, travel history, and exposure to birds and confirmation through PCR testing of upper respiratory tract samples like a nasopharyngeal swab.
Treatment for avian influenza focuses on antiviral medications such as oseltamivir which is most effective when administered early in the course of the illness but still administered after 48 hours of illness. Supportive care is essential for managing severe cases, especially those that progress to acute respiratory distress syndrome.
Background:
- Monkeypox virus (MPXV) has two distinct genetic clades (subtypes of MPXV), I and II, which are endemic to central and west Africa, respectively.
- The global mpox outbreak that began in 2022 is caused by MPXV II
- The recent outbreak in Democratic Republic of Congo (DRC) is caused by MPXV I
What’s new?
- Democratic Republic of Congo (DRC) has reported more than 22,000 suspect cases of MPXV I since January 1, 2023 (annual median of 3,767 suspect MPXV I cases in prior 6 years)
- Largest number of yearly suspected MPXV I cases ever recorded
- More widespread than any previous outbreak, resulting in transmission to neighboring countries [Republic of the Congo (ROC), the Central African Republic (CAR), Burundi, Rwanda, and Uganda].
Who is at risk?
Patients with epidemiologic characteristics and lesions or other signs and symptoms consistent with mpox. This includes anyone with travel to DRC or any of its neighboring countries (ROC, CAR, Rwanda, Burundi, Uganda, Zambia, Angola, Tanzania, and South Sudan) in the previous 21 days.
What to look for?
- Rash that may be located on the hands, feet, chest, face, mouth, anus or near the genitals
- Lesions are firm or rubbery, well-circumscribed, deep-seated, and often develop umbilication (see below).
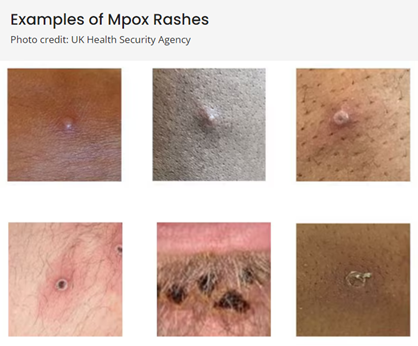
(Above photos from https://www.cdc.gov/poxvirus/mpox/clinicians/clinical-recognition.html)
- Lesions progress through four stages—macular, papular, vesicular, to pustular—before scabbing over and desquamation. They are often described as painful until the healing phase when they become itchy (crusts).
- Fever, chills, swollen lymph nodes
- Fatigue, myalgia (muscle aches and backache), headache
- Respiratory symptoms like sore throat, nasal congestion, and cough
- Illness lasts 2-4 weeks
- Once all scabs have fallen off and a fresh layer of skin has formed, a person is no longer contagious.
What to do?
If mpox is suspected in a patient:
- Isolate the patient in a single patient room (no special air filtration is required).
- Use PPE (Gown, gloves, eye protection, and NIOSH-approved particulate respirator equipped with N95 filters or higher).
- Intubation and any procedures likely to spread oral secretions should be performed in an airborne infection isolation room.
- Notify your local health department immediately.
- Evaluate all suspected cases related to DRC or its neighboring countries with laboratory testing (rather than clinical diagnosis alone).
- Counsel patients about staying away from other people and not sharing things they have touched with others; and cleaning and disinfecting the spaces they occupy regularly to limit household contamination.
- Recommend mpox vaccine to asymptomatic close contacts of cases of MPXV.
- Offer treatment with oral tecovirimat (TPOXX), available through the STOMP Trial. To enroll in STOMP, in the US call 1-855-876-9997.
Show References
The Infectious Disease Society of America in 2023 recommended a single dose of an aminoglycoside for uncomplicated cystitis treatment in those with resistance or other contraindications to first line oral agents who were otherwise well enough to be discharged. This very small study (13 participants) suggest this strategy works for complicated (“male sex, urinary flow obstruction, renal failure or transplantation, urinary retention, or indwelling catheters”) cystitis patients who could otherwise be discharged home.
Show References
- Didanosine: pancreatitis
- Indinavir: nephrolithiasis
- Isoniazid: hepatitis
- Trimethoprim-sulfamethoxazole: hyperkalemia, Stevens-Johnson Syndrome
- Ritonavir: paresthesias, metabolic syndrome
- Pentamidine: hyperglycemia or hypoglycemia
- Efavirenz: psychosis
- Dapsone: hepatitis
- Nevirapine: hepatic failure
- AZT: bone marrow suppression and macrocytic anemia
- IDSA/SHEA recently released a guideline update for the management of Clostridium difficle infections
- Discontinue inciting antibiotic therapy as soon as possible
- Metronidazole is no longer considered first line therapy for C. difficle infection
- Treatment course for 10 days unless initial fulminant or recurrence requiring vancomycin taper
- Remember: Vancomycin IV does not cross into the GI tract and cannot be used to treat C. difficile
| Clinical Definition | Treatment | |
| Initial episode, non-severe | WBC ≤ 15,000 AND SCr <1.5 |
If above agents unavailable, metronidazole PO 500mg 3x daily
|
| Initial episode, severe | WBC ≥ 15,000 OR SCr >1.5 |
|
| Initial episode, fulminant | Hypotension, shock, ileus, megacolon |
|
| First Recurrence |
|
|
Show References
Debating between cefepime or piperacillin/tazobactam for your septic patient? Use this table to help you decide.
|
|
| Cefepime | Piperacillin/Tazobactam |
| Gram Negative Spectrum | Pseudomonas aeruginosa | Yes | Yes |
| Aerobic gram negative organisms | E. coli Klebsiella sp. Proteus mirabilis M catarrhalis H. influenza | E. coli Klebsiella sp. Proteus mirabilis M. catarrhalis H. influenza | |
| Anerobic gram negative organisms | No | B. fragilis
| |
| Gram Positive Spectrum | MRSA | No | No |
| Aerobic gram positive organisms | MSSA CoNS Group A Strep S. pneumoniae
| MSSA CoNS Group A Strep S. pneumoniae E. faecalis | |
| Anaerobic gram positive organisms | P. acnes Peptostreptococci | P. acnes Peptostreptococci Clostridium sp. | |
| Infection Site Concerns | CNS Penetration | Yes | No1 |
| Urine Penetration | Yes | Yes | |
| Lung Penetration | Yes | Low2 | |
| Dosing Frequency (Normal Renal Function) | Q8h | Q6h | |
1. Tazobactam CNS penetration is limited, thus limiting antipseudomonal activity in the CNS
2. Low pulmonary penetration, may not achieve therapeutic levels in patients with critical illness
Show Additional Information
Show References
Community-associated Clostridium difficile infection (CA-CDI) represents 41% of all CDI cases annually. The association of specific outpatient exposures was assessed in a case control study by Guh, et al. They reviewed the CDC’s active surveillance reporting from 10 states through the Emerging Infections Program (Maryland participates).
Cases: ≥18, + C. difficile stool specimen collected as an outpatient or within 3 days of hospitalization, with no overnight stay in a health care facility in the prior 12 weeks, and no prior CDI diagnosis
Controls: matched 1:1 for age and sex within the same surveillance catchment area as the case patient on the date of the collection specimen. Exclusion criteria: prior diagnosis of CDI, diarrheal illness, overnight stay in health care facility in the prior 12 weeks
Data Collection: telephone interview, standardized questionnaire or comorbidities, medication use, outpatient health care visits, household and dietary exposures in the prior 12 weeks
Results: 452 participants (226 pairs), over 50% were ≥ 60 years of age, 70.4% female, and 29% were hospitalized within 7 days of diagnosis, no patients developed toxic megacolon or required colectomy.
Cases had more health care exposures, including the emergency department (11.2% vs 1.4% p <0.0001), urgent care (9.9% vs 1.8%, p=0.0003). In addition, cases also reported higher antibiotic exposures (62.2% vs 10.3%, p<0.0001) with statistically significant higher exposure to cephalosporins, clindamycin, fluoroquinolones, metronidazole, and beta-lactam and/or beta-lactamase inhibitor combination. The most common antibiotic indications were ear or sinus infections, URI, SSTI, dental procedure, and UTI. No differences were found in household or dietary exposures.
Take-home point: This study highlighted the risk for CA-CDI infection for patients presenting to an ED and reiterates that exposures to fluoroquinolones, cephalosporins, beta-lactam and/or beta-lactamase inhibitor combinations, and clindamycin significantly increases the risk of CA-CDI infection. Reducing unnecessary outpatient antibiotic prescribing may prevent further CA-CDI. 36% of case patients did not have any antibiotic or outpatient health care exposure; therefore, additional risk factors may exist.
Show References
Take home points:
- Cellulitis is overdiagnosed
- 1/3 of patients diagnosed with cellulitis in the ED are ultimately given a different diagnosis
- The most common final diagnoses are vascular or inflammatory conditions.
- The over treatment of cellulitis increases healthcare costs, increases risk of adverse reactions, and can contribute to the development of drug resistant organisms.
Show Additional Information
Zika virus and its transmission is currently an important infectious disease topic in the United States and the Western Hemisphere. With domestic spread in the Continental United States, and the likely further spread to other parts of the southern United States, continued vigilance by healthcare providers remains important.
What are the signs and symptoms of Zika?
Most common signs and symptoms are:
- Fever
- Rash
- Arthralgias
- Conjunctivitis (generally nonpurulent)
Other symptoms can include
- Myalgias
- Headaches
- Retro-orbital pain
- Gastrointestinal upset
Symptoms can generally last 2 to 7 days. Most individuals will have minimal or no significant symptoms and may not seek medical care. These symptoms are similar to other arboviruses, such as dengue or chikungunya. Potential serious complications include Guillian Barre syndrome.
Of course, the main concern remains infection of pregnant women and the impact that Zika has on the developing fetus, especially for the brain.
Show References
Cutaneous larva migrans (CLM) is an acquired dermatosis
- Seen in patients returning from the tropics
- Often seen in patient with a history of sunbathing or in barefoot beachgoers
- Caused by the larvae of various nematode parasites of the hookworm family (Ancylostomatidae), with Ancylostoma braziliense the most frequently found in humans.
Clinical manifestations:
- Linear, serpentine erythematous lesions
- Intense pruritus
- Will often heal spontaneously over weeks or months without treatment
Treatment:
- Thiabendazole (applied topically)
- Oral alternatives include other anti-parasitic medications such as albendazole, ivermectin
- Oral thiabendazole as a single dose can be used, but is less effective than albendazole or ivermectin
- Consider antibiotics if there is secondary bacterial infections
- Freezing the leading edge has been previously used, but is considered ineffective and painful.
Bottom Line:
- Consider CLM the next time a patient complains of a linear, erythematous itchy rash after returning from their all-inclusive stay in a Caribbean resort
Show References
Attachments
Borrella mayonii a new species
There is a new bacteria that is causing Lyme disease. Borrella burgdorferi is the typical bacteria associated with lyme disease, but now several cases of Borrelia mayonii have been isolated from patients and ticks that live in Minnesota, Wisconsin and North Dakota. What is unique about this new species is that it is associated with nausea, vomiting, diffuse macular rashes, and neuro symptoms [e.g.: confusion, visual disturbance, and somnolence) along with the typical lyme disease symptoms of arthralgias and headaches.
Current lyme tests should detect this new species and treatment is the same as Borrella burgdorferi. The take home pearl is that we may see patients with "atypical" lyme disease symptoms so this should be on our differential for patients presenting with rashes, nausea, vomiting and neurologic complaints.
