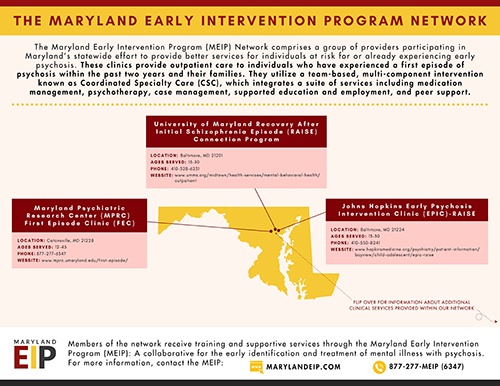
Our team has compiled the below materials related to early psychosis, pathways to treatment, and our work at the MEIP.
Maryland EIP Flyers
Resources for Youth, Families, and Providers
For Youth and Families:
- Understanding Psychosis (NIH).pdf
- Understanding Psychosis - Resources and Recovery (NAMI)
- Coping when someone in your family has psychosis (EPI)
- Understanding Psychosis - A guide for young people and their supporters (BPS)
- Promoting Recovery from First Episode Psychosis - A Guide for Families (CAMH)
- Understanding A First Episode of Psychosis - Caregiver Guide (SAMHSA)
- [book] The First Episode of Psychosis: A Guide for Young People and Their Families (Broussard & Compton)
- [book] The Complete Family Guide to Schizophrenia: Helping Your Loved One Get the Most Out of Life (Mueser & Gingerich)
- Coordinated Specialty Care Fact Sheet & Checklist (NIH)
- Strategic Sharing Workbook - Youth Voice in Advocacy (NFF)
- Navigating a First Episode of Psychosis for Muslim Patients & Families (HH)
- Early Serious Mental Illness Treatment Locator (SAMHSA)
- Early Psychosis Intervention Network (EPINET) Clinics
For Providers:
- Psychosis Screening in Primary Care (CEDAR)
- Coordinated Specialty Care for FEP - Costs & Financing Strategies (SAMHSA)
Lived Experience Videos & Teaching Tools
Experiences of Young Adults: Living with Mental Illness and Psychosis
Using federal American Rescue Plan Act (ARPA) funding through the State of Maryland, the University of Maryland School of Medicine, Morgan State University, and the University of Maryland, Baltimore County collaborated to improve the quality and depth of clinical training related to psychosis. As part of this work, a series of lived experience videos and associated tools and guidelines were developed to improve awareness and understanding of psychosis in young adults.
View and download the Historical & Ethical Considerations for Early Identification of Psychosis slide deck.
Together, these materials are intended to support faculty and other trainers in teaching about the early identification and treatment of mental illness with psychosis for pre-service health and mental health students as well as professionals in the field. The videos include the lived experiences of young adults and families; we are indebted to them for their honesty, vulnerability, and willingness to share their reflections.
These videos are considered property of the three universities and should only be used for educational purposes. They should not be downloaded or shared outside of the classroom or the clinic setting. The videos are intended to be used as part of courses and training that integrate the best practices and the foundational information that is provided in the associated materials.