Search
281-300 of 321 results by Haney Mallemat
Question
13 year-old right-hand dominant male following assault with blunt object. Diagnosis?
Show Answer
Show References
Pregnancy causes many physiologic changes, which may be challenging during trauma resuscitations. A few pearls on the ABC’s:
Airway
- Increased progesterone levels cause mucosal hyperemia and edema, increasing risk of bleeding and smaller (i.e., edematous) airway.
- PEARL: Have smaller tubes ready and let the most experienced person intubate.
Breathing
- The enlarging uterus pushes the diaphragms into the thorax, reducing the total lung capacity and the functional residual capacity.
- PEARL: During intubation, patients in late pregnancy may have less oxygenation reserve and apnea time, desaturating faster during RSI.
Circulation
- The late stage uterus can compress the IVC when supine, reducing venous return to the heart (i.e., the Supine-Hypotension syndrome) subsequently reducing cardiac output.
- PEARL: Have a 30-degree wedge placed under patient's right hip, moving the uterus off IVC and improving venous return.
- BONUS PEARL: During resuscitation, ask medical students to manually move the uterus midline, relieving the compressed IVC. They will appreciate that you got them clinically involved.
Show References
Question
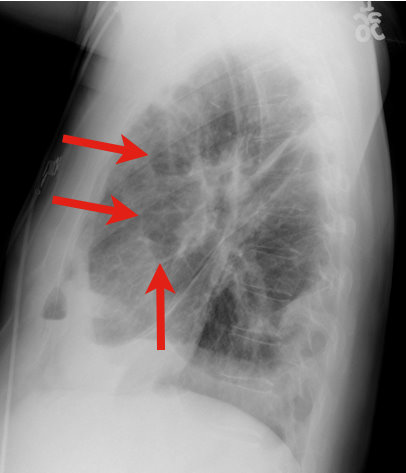
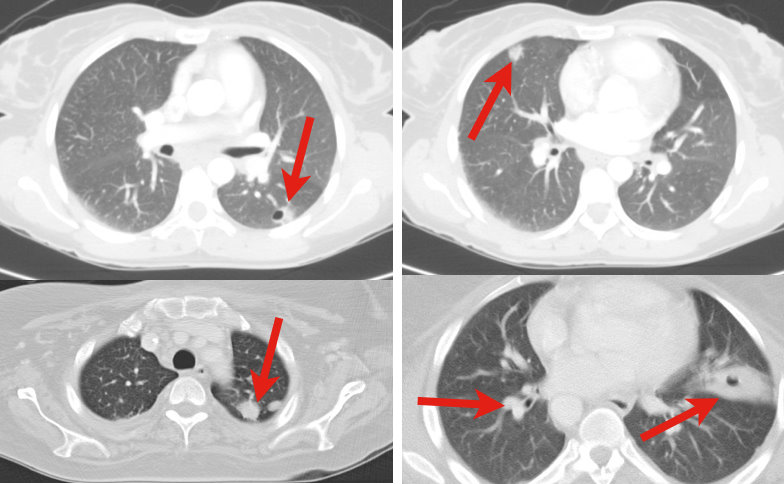
34 y.o. male with history of IVDA (intravenous drug abuse) complains of fever, chills and cough. Diagnosis?

Show Answer
Show References
Heat stroke is hyperthermia (>41.6 Celsius / 106 Fahrenheit) plus neurologic findings (e.g., altered mental status, seizures, coma, etc.); it also causes systemic inflammation response syndrome (i.e., cytokine release), coagulation disorders (e.g., thrombosis in end organs) and tissue abnormalities (e.g., acute kidney injury and rhabdomyolysis)
Two classifications exist:
- Exertional heatstroke (young people engaged in strenuous physical activities in hot climates)
- Non-exertional heatstroke occurring in sedentary people (elderly, debilitated, or chronically-ill patients) who are unprotected from the elements (e.g., trapped in apartments during heat waves)
Treatment includes:
- Insertion of a continuous core thermometer
- Supporting ABC’s
- Cooling by at least to 0.2 degrees celsius per minute to 39 degrees (to avoid overshoot)
- Benzodiazepines for sedation, shivering, and seizures
- Antipyretics and phenytoin have not been shown beneficial
- Support and protect end-organs with particular attention to kidneys; increased risk of kidney injury from rhabdomyolysis, ischemia and systemic inflammation.
Despite the most aggressive therapy, up to 30% survivors may have permanent neurologic or multi-organ system dysfunction months to years after recovery
Show References
Question
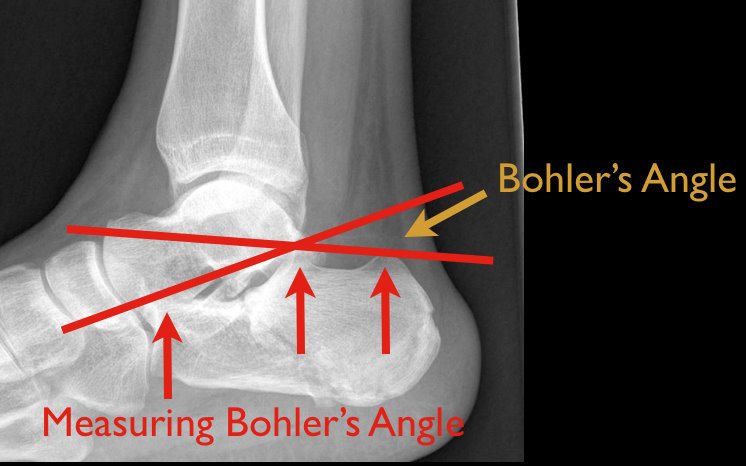
48 year old male following 15 foot fall onto both feet. What is the diagnosis?
…and why is it called the “Lover’s Fracture”?

Show Answer
Show References
Amiodarone is a class III anti-arrhythmic for tachyarrhythmias
Although most patients remain euthyroid on amiodarone, 4-18% develop thyroid disease months to years after exposure.
Amiodarone-induced thyroid disease occurs because amiodarone is structurally similar to triiodothyronine and thyroxine and each 200mg tablet contains 75 mg of iodine.
Two types of amiodarone-induced thyroid disease:
- Amiodarone-induced hypothyroidism (AIH)
- Amiodarone-induced thyrotoxicosis (AIT)
Amiodarone-induced hypothyroidism (AIH)
- Presents with subtle to overt hypothyroidism
- Treat by discontinuing amiodarone; thyroid recovers within 3 months
- If amiodarone cannot be discontinued, start levothyroxine
Amiodarone-induced thyrotoxicosis (AIT)
- Sudden symptom onset months to years following exposure; mean 2-47 months post-exposure
- Can be a life-threatening presentation (similar to thyroid storm) with severe cardiac manifestations and hemodynamic instability
- Treatment (treat like thyroid storm, if severe)
- Discontinue drug, if possible
- Thionamides (inhibit enzyme producing thyroid hormones)
- Methimazole or propylthiouracil
- Beta-blockers
- Steroids
- Airway and hemodynamic support
Show References
Question
49 y.o. female on Trimethoprim/sulfamethoxazole presents with rash and oral mucus membrane lesions. Diagnosis?

Show Answer
Show References
Cancer patients admitted to ICUs with AKI or who develop AKI during their ICU stay have increased risk of morbidity and mortality. AKI in cancer patients is typically multi-factorial:
Causes indirectly related to malignancy
-
Septic, cardiogenic, or hypovolemic shock (most common)
-
Nephrotoxins:
-
Aminoglycosides
-
Contrast-induced nephropathy
-
Chemotherapy
-
-
Hemolytic-Uremic Syndrome
Causes directly related to malignancy
-
Tumor-lysis syndrome
-
Disseminated Intravascular Coagulation
-
Obstruction of urinary tract by malignancy
-
Multiple Myeloma of the kidney
-
Hypercalcemia
Because AKI increases the already elevated morbidity and mortality in these patients, prevention (e.g., using low-osmolar IV contrast, avoiding nephrotoxins), early identification (e.g., strict attention to urine output and renal function), and aggressive treatment (e.g., early initiation of renal replacement therapy) is essential.
Show References
Question
13 y.o. with shoulder trauma (during basketball game). Arm held in adduction and exquisite scapular tenderness. Diagnosis?

Show Answer
Show References
Bleeding associated with uremia is a spectrum, from mild cases (e.g., bruising or prolonged bleeding from venipuncture) to life-threatening (e.g., GI or intracranial bleed). The exact pathologic mechanisms are not understood, but are likely multi-factorial (e.g., dysfunctional von Willebrand’s Factor (vWF) and factor VIII, increased NO, etc.)
Besides dialysis, treatments for uremic bleeding include:
- DDAVP (fastest)
- 0.3-0.4 micrograms/kg IV or SC
- Increases vWF and factor VIII release
- Advantages: Begins < 1 hour
- Disadvantages: Tachyphylaxis; Stored factors deplete
- Cryoprecipitate
- Replaces fibrinogen, vWF, and factor VIII
- Advantages: Works 1-4 hours
- Disadvantages: transfusion reactions, infections, pulmonary edema, etc.
- Conjugated Estrogens
- Unclear mechanism; possibly increases ADP and thromboxane activity
- 0.6 mg/kg once daily x 5 days
- Advantages: Short and long-term effects
- Disadvantages: Hot flashes (males too!)
- Recombinant Erythropoietin (slowest)
- 40-150 U/kg three times weekly
- Multiple mechanisms
- Advantages: Helps anemia (common in renal failure) as well as bleeding complications.
- Disadvantages: Up to 7 days to observe effects
Show References
Question
13 y.o. female with ankle pain following fall down escalator. What's the diagnosis? (Hint: Look very closely)

Show Answer
- Necrotizing enterocolitis with predilection for cecum.
- Occurs in the immunosuppressed, especially when neutropenic (<500 PMNs)
- Typically a polymicrobial infection; gram positive cocci, gram negative rods, anaerobes, and/or fungal.
- Classically, right lower quadrant pain but can present with diffuse abdominal pain and peritoneal signs.
- CT scan with IV and PO contrast is diagnostic (see below)
- Treatment:
- Culture and begin broad spectrum antibiotics (cover anaerobes) and antifungals (if suspected)
- Aggressive resuscitation
- Surgical consult for GI perforation or clinical deterioration
- High mortality (40-50%)
TIP: Suspect when abdominal pain presents 10-14 after chemotherapy (when PMNs are lowest).

Show References
Although oral metronidazole is indicated for mild to moderate Clostridium difficile associated diarrhea, oral vancomycin should be considered first-line therapy in critically-ill patients with moderate to severe disease. Vancomycin dosing should begin at 125mg PO q6 and increased to 250mg q6 if poor enteral absorption exists. Consider adding metronidazole IV if either reduced enteral absorption or severe disease exists.
Recently, fidaxomicin has been shown to be non-inferior to oral vancomycin in the treatment of mild to moderate C. difficile. While promising, the study population was not critically-ill and extrapolation should be avoided.
Show References
Question
70 yo female from nursing home with fever. RUQ ultrasound is shown below. Diagnosis?

Show Answer
A mortality benefit from combination antimicrobial therapy has not been clearly demonstrated in sepsis. However, when only the most severely-ill patients (i.e., septic shock) are considered in subgroup analysis, there appears to be a mortality benefit to using two antimicrobials against a suspected organism.
Combination antimicrobial therapy may reduce mortality through three mechanisms.
- Increased probability that the causative organism will respond to at least one drug.
- Preventing emergence of antimicrobial resistance.
- Two antimicrobials may act synergistically.
Always obtain appropriate cultures before initiating therapy. Although identification and susceptibility of the organism may take some time, eventually narrowing antimicrobial therapy to monotherapy in the ICU is still recommended.
Show References
Question
Patient presents with the following X ray after yawning. Diagnosis?

Show Answer
Show References
Vancomycin is often started empirically for gram-positive and MRSA coverage. Although effective and generally well-tolerated, emerging resistance and side-effect profiles limit its use in some patients. Two alternatives are Linezolid and Daptomycin.
Linezolid
- 600 mg IV every 12 hours
- No renal dosing
- Better lung penetration in pneumonia (compared to Vancomycin)
- Side effects: Serotonin Syndrome (w/ concurrent MAOIs), hypersensitivity reaction, and myelosuppresssion
Daptomycin
- 4 mg/kg IV once daily (skin/subcutaneous tissues infection), 6 mg/kg IV once daily (bacteremia or endocarditis), or 6-8mg/kg IV once daily (bacteremia with intravascular line)
- Renally dosed by altering administration frequency; no change in dose.
- NEVER use for pneumonia; pulmonary surfactant binds and inactivates drug.
- Side effects: Reversible rhabdomyolysis (requires weekly CPK levels)
Show References
Question
60 y/o male transferred from local rehab facility c/o abdominal pain.

Show Answer
Show References
Emergency Medicine physicians are gaining experience with non-invasive ventilation (i.e., Bi-level ventilation and continuous positive-pressure ventilation) in managing respiratory distress and failure. Although NIV is commonly used across a variety of pathologies, the best data exists for use with COPD exacerbation and cardiogenic pulmonary edema (CHF, not an acute MI)
Although other indications for NIV have been studied, the data is less robust (eg., smaller study size, weak control groups, etc.). If there are no contraindications, however, many experts still support a trial of NIV in the following populations:
- Asthma
- Severe community acquired pneumonia
- Acute lung injury / Acute Respiratory Distress Syndrome
- Chest trauma (lung contusion, rib fractures, flail chest,etc)
- Immunosuppression with acute respiratory failure
- Neuromuscular respiratory failure (eg., Myesthenia Gravis)
- Cystic Fibrosis
- Pneumocystis Jiroveci Pneumonia
- “Do not intubate” status
Failure to clinically improve during a NIV trial should prompt invasive mechanical ventilation.