Search
321-340 of 543 results with category "Pediatrics"
- Nebulized epinephrine: 0.9mg/kg for racemic epi or 0.03 mL/kg of the 2.25% solution (diluted in 3mL) - improves oxygen saturation and respiratory rate, but does not affect admission rates
- Hypertonic saline (3%): decreases hospital length of stay and improves clinical scores, possibly by decreasing airway edema and mucus plugging
- Nasal CPAP: improves ventilation in children with bronchiolitis and hypercapnia
- Heliox: decreases respiratory distress, by reducing gaseous flow resistance and improving alveolar ventilation
Interventions that have shown no benefit and are not recommended:
- Anticholinergics
- oral and/or inhaled corticosteroids
Reference:
Joesph, M. Evidence-Based Assessment and Management of Acute Bronchiolitis in the Emergency Department. Pediatric Emergency Medicine Practice 2011; 8(3)
Parents bring in their child who placed a bead, seed, or other object up her nose. What do you do? Who should you call?
Research suggests that a decades-old home remedy (of sorts) known as the “mother’s kiss” may do the trick for children 1-8 years of age. It’s also much less invasive or frightening than some of the tools and techniques used in emergency departments with a success rate approaching 60%
What Is the “Mother’s Kiss”?
First described in 1965, here’s how the mother’s kiss technique works:
- The parent or caretaker places their mouth over their child’s mouth while holding the unaffected nostril closed with one finger.
- The parent or caretaker blows into the child’s mouth.
- The forceful breath may force the object out (warning: may want to wear protective covering as other things have been known to fly out as well!)
Epidemiology:
Trampoline injuries doubled between 1991 and 1996, increasing from 39,000 injuries per year to more then 83,000 injuries per year. Injury rates and trampoline sales peaked in 2004 and have been decreasing since; however, hospitalization rates are still between 3% and 14%.
Risk Factors:
¾ of injuries occur when multiple people are on the trampoline at once
Smaller participants were 14x more likely to be injured then their heavier playmates
Falls account for 27-39% of all injuries
Springs and frames account for 20% of injuries
Up to ½ of injuries occur despite adult supervision
Injury types:
Lower extremity injuries are more common than upper extremity
Head and neck injuries accounted for 10-17% of trampoline injuries
Unique Injuries:
Proximal tibial fractures
Manubriosternal dislocations and sternal injuries
Vertebral artery dissection
Atlanto-axial subluxation
Show References
Question
A 1 year old gets sent from their pediatrician’s office for rule out meningitis. They presented with fever for 2 days and neck rigidity. Your LP results are normal. What additional test should you consider?
Show Answer
Conventional pediatric nasal cannula can safely deliver up to 4 lpm but are limited by cooling and drying of the airway. This leads to decreased airway patency, nasal mucosal injury, bleeding and possibly increase in coagulase negative staph infections.
HFNC delivers flow up to 40 lpm with 95-100% relative humidity at a controlled temperature. In infants, the initial flow rate is set between 2-4 lpm and can be increased to 8 lpm. Older children and can be started at 10 lpm and increased as high as 40 lpm. Oxygen is also adjustable.
Studies have shown improved comfort, respiratory rate and oxygenation compared to nasal CPAP.
Show References
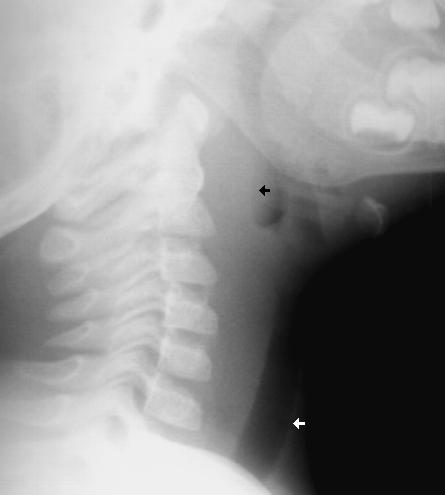
- The differential of child with stridor <6m:
- Tips for the treatment of croup:
- approximately 1% of children in DKA have some degree of cerebral edema, and up to 25% of them may die
- known risk factors include the following:
- younger children (especially <5 years)
- new onset or newly diagnosed
- increased BUN at presentation
- severity of acidosis at presentation
- bicarbonate therapy use
- failure of sodium to improve following therapy
Show References
We often ask our pediatric patients if there vaccines are up to date, but what does this mean?
Hepatitis B: birth, 2 and 6 months
Diphtheria/Tetanus and Acellular Pertussis: 2, 4 and 6 months
Pneumococcal vaccine: 2, 4 and 6 months
Haemophilus influenzae B : 2, 4 and 6 months
Polio: 2, 4 and 6 months
Rotavirus: 2 and 4 months or 2, 4 and 6 months depending on the brand.
Influenza: 6 months and older
Children less than 8 years old should receive 2 doses of flu vaccine at least 4 weeks apart during the first flu season that they are immunized. Children older than 2 years are eligible for the nasal vaccine if they do not have asthma, wheezing in the past 12 months or other medical conditions that predispose them to flu complications.
To see the full vaccine schedule including exact time frames between doses and catch up schedules, see: http://www.cdc.gov/vaccines/
Show References
The incidence of pediatric syncope is common with 15%-25% of children and adolescents experiencing at least one episode of syncope before adulthood. Incidence peaks between the ages of 15 and 19 years for both sexes.
Although most causes of pediatric syncope are benign, an appropriate evaluation must be performed to exclude rare life-threatening disorders. In contrast to adults, vasodepressor syncope (also known as vasovagal) is the most frequent cause of pediatric syncope (61%–80%). Cardiac disorders only represent 2% to 6% of pediatric cases but account for 85% of sudden death in children and adolescent athletes. 17% of young athletes with sudden death have a history of syncope.
Key features on history and physical examination for identifying high-risk patients include exercise-related symptoms, a family history of sudden death, a history of cardiac disease, an abnormal cardiac examination, or an abnormal ECG.
- sleep disruption silimar to a nightmare, but much more dramatic most often between 4-12 years
- sudden fear reaction which occurs during the transition to and from deep non-REM sleep while nightmares occur during REM sleep
- occurs 2-3 hours after falling asleep when the child suddenly awakens in distress and may thrash about, scream, cry
- child returns to sleep with no memory of the event the following morning
- often occurs when a child is stressed, overtired, on new medication, or sleeping in a new environment
- do not awaken the child during the event but rather allow them to calm on their own
Ligamentous laxity is increased in children and ligamentous injury is more common than fractures.
If fractures occur, they are more likely to be in the upper cervical spine in infants and the lower cervical spine in older children.
Pseudosubluxation: physiologic subluxation between C2-3 and C3-4 may exist until age 16 years
Screening Assessment/Clearance for Verbal Children
-Midline C-spine tenderness?
-Pain with active motion?
-Altered level of alertness?
-Evidence of intoxication?
-Focal neurological deficit?
-Distracting painful injury?
-High impact injury?
Screening Assessment/Clearance for Pre-Verbal Children
-Neurological assessment of basic reflexes
-Response to painful stimuli
-Equal movements of all extremities
-Response to sound (eye tracking)
-Extremity strength and resistance
-Palpate posterior C-spine (observe for facial grimace)
-Feel for step-offs, deformities
-Verify full range of motion of neck (may need to be creative)
-Repeat neurological assessment
If concern arises on screening assessment, keep child in hard cervical collar and image (may start with x-ray and progress to CT if still concerned and x-rays negative).
If imaging negative, but persistent suspicion based on neurological deficits consider SCIWORA (Spinal Cord Injury WithOut Radiographic Abnormality) which exists in up to 50% of children with cervical cord injury, and may require MRI to further identify injury.
The PALS algorithm includes 5 points in management. The first two points are optimally reached within one hour:
1) Recognition of sepsis and vascular access
2) 20ml/kg IVF X 3 within 1 hour or 60ml/kg IVFs within 15 minutes and antibiotic administration
3) Determine if fluid responsive
A recent study at a tertiary care children's hospital retrospectively reviewed 126 patients diagnosed with sepsis. Their findings:
- 37% received 60ml/kg in 60 minutes
- 11% received 60ml/kg in 15 minutes
- 70% received antibiotics in 60 minutes
- In 49% of cases fluids were delivered via IV infusion pump versus manual or pressure bag
- There was a 57% shorter overall hospital stay and 42% shorter ICU stay in patients that received 60ml/kg IVFs within 60 minutes.
- Liver enzymes, coagulation profiles, and lactic acid levels were obtained in "few" patients.
Conclusions:
Suboptimal fluid resuscitation in sepsis is linked to longer hospital stays. Knowledge of PALS guideline and faster administration of fluid were thought to have been causes of poor adherence.
Additionally, parameters measured in sepsis including lactic acid, coagulation studies, and liver enzymes were not routinely collected. The authors concluded this came from a lack of knowledge of their utility in sepsis.
References:
Paul R, et al. "Adherence to PALS Sepsis Guidelines and Hospital Length of Stay." Pediatrics: 2012 Jul 2 [epub adhead of print].
Types:
- Uniphasic anaphylaxis: occuring immediately after exposure to allergen, resolves over minutes to hours and does not recur
- Biphasic anaphylaxis: occuring after apparent resolution of symptoms typically 8 hours after the first reaction. Occur in up to 23% of adults and up to 11% of children with anaphylaxis
Treatment:
1. First line: IM epinephrine 1:1000 solution
- vasoconstrictor effects on hypotension and peripheral vasodilation; bronchodilator effects on upper respiratory obstruction
- NO absolute contraindication for use in anaphylaxis
- Dosage: Adult: 0.3 - 0.5mg; Peds: 0.01mg/kg (max 0.3mg)
- can be repeated every 5-15 minutes
2. Adjunctive therapy:
- H1 Blocker: diphenhydramine 1-2mg/kg up to 50mg IV
- H2 Blocker: ranitidine 1-2mg/kg
- Corticosteroid: 1-2 mg/kg for prevention of biphasic reactions
- Bronchodilator: Albuterol for bronchospasm
- Glucagon: for refractory hypotension or if patient is on beta blocker
- Dosage: Adult: 1-5 mg; Peds 20-30microgm/kg
- Dose may be repeated or followed by infusion of 5-15 mg/min
- place patient in recumbent position if tolerated with lower extremities elevated
- supplemental O2
- IV fluids for hypotension
Fatalities: typically seen with peanut or treenut ingestions from cardiopulmonary arrest. Associated with delayed or inappropriate epinephrine dosing
Disposition:
- Mild reaction with symptom resolution: observe for 4-6 hrs (ACEP, AAP)
- Recurrent symptoms or incomplete resolution: admit
Reference:
1. World Allergy Organization Guidelines for the Assessment and Management of Anaphylaxis, Feb 2011
2. Guidelines for the Diagnosis and Management of Food Allergy in the United States: Report of the NIAID-Sponsored Expert Panel Oct 2010
If you have a patient who meets (or has had close exposure to someone meeting) the clinical case definition of pertussis (a cough lasting at least 2 weeks with one of the following: paroxysms of coughing, inspiratory “whoop,” or post-tussive vomiting) here are some important points to keep in mind:
Vaccination
- Be wary that children younger than 7 might not be “up to date” for pertussis vaccination.
- The recommended schedule is four primary doses of DTap at 2, 4, 6 and 15-18 months, and a fifth DTap booster at 4- 6 years old. ACIP now recommends kids 7 and older get a Tdap booster if their immunizations were previously incomplete.
Testing
- The available testing modalities for routine surveillance are culture and/or PCR (from a posterior nasopharyngeal swab or aspirate) and serologic testing.
- Serologic results are not currently accepted as laboratory confirmation for purposes of national surveillance, but may be more useful for testing patients in the convalescent stage.
Treatment
- The CDC recommends treatment of clinical or confirmed cases with one of these regimens:
- Azithromycin daily x 5 days
- Clarithromycin BID x 7 days
- Erythromycin QID x 14 days
- Trimethoprim/sulfamethoxazole (Bactrim) BID x 14 days if resistance or allergy to macrolides
- However, a 2011-updated Cochrane review showed that short-term antibiotics (azithromycin for 3-5 days, or clarithromycin or erythromycin for 7 days) were as effective as long-term (erythromycin for 10-14 days) (RR 1.01) (95% CI 0.98-1.04). Trimethoprim/sulfamethoxazole for seven days was also effective.
- Insufficient evidence to decide whether there is clear benefit for treating healthy contacts, but the CDC does recommend prophylactic treatment of close contacts and family members.
References:
Altunaiji SM, Kukuruzovic RH, Curtis NC, Massie J. Antibiotics for whooping cough (pertussis). Cochrane Database of Systematic Reviews 2007, Issue 3. Art. No.: CD004404. DOI: 10.1002/14651858.CD004404.pub3
http://www.cdc.gov/vaccines/pubs/surv-manual/chpt10-pertussis.html
- small growth of grainy pink/redish tissue that forms on an area of the umbilical stump which is inflamed and produces a sticky mucous dishcarge not allowing normal tissue to grow on top of it
- caused by abnormal tissue healing after the remaining umbilical cord dries up and falls off
- treatment is painless as the granuloma lacks innervation, and requires applying chemical silver nitrate directly to the granumloma to burn the tissue off
- although rare, careful examination of the tissue is needed to enssure the tissue is not intestinal or bladder in origin
Henoch-Schonlein Purpura (aka. Anaphylactoid purpura) is a small vessel vasculitis.
Background:
- most commonly diagnosed vasculitide in childhood
- age range 3-15 years, mean age 4yo, mostly <7yo (75% cases)
- more cases in Winter and Spring months
- boys more commonly than girls (2:1)
- IgA-mediated leukoclastic vasculitis
Clinical Features:
- Rash: progresses to petechiae, purpura; occurs on lower extremities and buttocks in dependent areas
- Joints: arthritis/arthralgia mainly of large joints (knees, ankles)
- GI: colicky abdominal pain, may occur with melena (33%) or less likely, hematemesis; ultrasound for intussusception (2-14%)
- Renal: microscopic hematuria with/without proteinuria; usually transient but may lead to progressive renal disease in patients with more severe, persistent symptoms
- Orchitis and/or angioedema may also occur
Etiology:
- unknown
- preceding URI (50%)
- associated with bacteria (Strep pyogenes, Legionella, Mycoplasma), viruses (EBV, CMV, parvovirus), drugs (penicillin, cephalosporins), and insect bites
Diagnosis:
- clinical features
- lab studies that are helpful but nonspecific: high WBC, high ESR, high IgA, normal platelet and coagulation studies
Treatment:
- supportive care, may last up to 4 weeks
- steroids may be helpful but evidence has not shown true benefit
- recurrence happens in 40% of cases
- G6PD deficiency
- Asphyxia
- Lethergy
- Sepsis
- Albumin < 3.0
- Maternal and fetal blood type
- Birth hx: term or preterm, GBS, TORCH infections
- Fever
- Poor feeding/ feeding patterns, including whether mom feels engorged and if latching is successful
Bonus pearl: Types of Jaundice by Age
- < 24 hrs: hemolyis, TORCH, bruising from birth trauma (ie- cephalohematoma), acquired infection
- Day 2-3: Physiologic
- Day 3-7: infection, congenital diseases, TORCH
- >1 week: Breast Milk Jaundice, breast feeding jaundice, drug hemolysis, hypothyroidism, biliary atresia, hepatitis, red cell membrane disorders (SS, HS, G6PD deficiency)
Approximately 12,000 children are diagnosed with malignancies in the USA each year. Cancer is the second leading cause of death in children in the USA. Acute leukemias are the most common type of cancer, 26% of all cancer diagnosis. Brain tumors and lymphomas are the next most common categories of neoplasm in children.
Findings which should prompt further work-up in the ED are: pallor, bleeding: petechiae, purpura, bone pain, limp, painless lymphadenopathy, gingival hyperplasia, abdominal mass, night sweats, pruritis, and unintended weight loss
- congenital disorder which is the most common cause of stridor in infancy
- larynx appears disproportionately small, and supporting structures are abnormally soft
- stridor begins within the first 4 weeks of life, and accentuates with increased ventilation (crying, excitement, URI, etc.)
- stridor usually resolves by 12 months but may recur with URI until about 3 years of age
- diagnosis is by fiberoptic bronchoscopy or direct laryngoscopy
- therapy is usually not needed, but rarely laser therapy of redundant tissue or traceostomy when stridor occurs with failure to thrive or apnea