Search
41-60 of 93 results by Mimi Lu
Dehydration is a common pediatric ED presentation. Oral rehydration (although first choice) is often not possible secondary to patient cooperation and/ or persistent vomiting. Intravenous (IV) hydration is often difficult, requiring multiple attempts especially in the young dehydrated infant.
Hyaluronan is a mucopolysaccharude present in connective tissue that prevents the spread of substances through the subcutneous space. Hyaluronidase is a human DNA-derived enzyme that breaks down hyaluronan and temporarily increases its permeability, thereby allowing fluid to be absorbed with the capillary and lymphatic systems.
In one study, patients age 1 month to 10 years were randomized to recieve 20 mL/kg bolus NS via subcutaneous (SC) or IV route over one hour, then as needed. The mean volume infused in the ED was 334.3 mL (SC) vs 299.6 mL (IV). Succesful line placement occured in all 73 SC patients and only 59/75 IV patients. There was a higher proportion of satisfaction for clinicians and parents for ease of use and satisfaction, respectively.
Bottom line: Consider subcutaneous hyaluronidase faciliated rehydration in mild to moderately dehydrated children, especially with difficult IV access.
Show References
There are numerous different causes of pediatric hemorrhagic diarrhea. Consider a pediatric patient with bloody diarrhea as being at risk for developing hemolytic uremic syndrome. Most cases of hemolytic uremic syndrome are caused by O157:H7 strains of E Coli that release Shiga-like toxin from the gut. Systemic release of the toxin causes microvascular thromboses in the renal microvasculature. The characteristic microangiopathic hemolysis results with anemia, thrombocytopenia and peripheral schistocytes seen on laboratory studies, in addition to acute renal failure.
Antibiotics have been controversial in the treatment of pediatric hemorrhagic diarrhea due to concern that they worsen toxin release from children infected with E Coli O157:H7 and thus increase the risk of developing hemolytic uremic syndrome. Numerous previous studies have provided conflicting data regarding the true risk (1). A recent prospective study showed antibiotic treatment increases the risk (2). Most recommendations warn against using antibiotics to treat pediatric hemorrhagic diarrhea unless the patient is septic.
Bottom line: Avoid treating pediatric hemorrhagic diarrhea with antibiotics
Show References
A recent retrospective study examined predictors of survival for pediatric traumatic out-of-hospital cardiac arrest. Of the 362 patients included in the study, none had spontaneous circulation upon arrival in ED. BLS was initiated by EMS in the field with a mean response time of 5.4 minutes and mean transport time of 10.2 minutes. The study compared MAP, cardiac rhythm, urine output, skin color of face/trunk, initial GCS and body temperature.
In this study, 9% of kids made it to discharge, 11 of which had good neurologic outcome and 23 with poor neurologic outcome. Predictors of survival were:
- High or normal BP
- Normal heart rate after ROSC
- Sinus rhythm after ROSC
- Urine output >1 ml/kg/hr
- Noncyanotic skin color
- GCS >7 on arrival
Reference: Predictors of survival and neurologic outcomes in children with traumatic out-of-hospital cardiac arrest during the early postresuscitative period. Lin YR, Wu HP, Chen WL, et al. Journal Trauma Acute Care Surg. Sept 2013:75(3);439-447.
Cringing at the thought of sewing up another screaming 2 year old?
Consider intranasal fentanyl.
Who: Young, otherwise healthy pediatric patients undergoing minor procedures (laceration repair, fracture reduction/splinting, etc...)
What: Fentanyl (2mcg/kg)
When: 5 minutes pre-procedure
Where: Intranasal
Why: More effective than PO, less invasive than IV while being equally efficacious.
How: Use an atomizer, splitting the dose between each nostril.
Department Reduces time to analgesic Administration, Anna Holdgate, MBBS, Academic Emergency Medicine 2010, 17:214-217.
Ultrasound findings of appendicitis
- noncompressible appendix with an outer diameter in any portion > 6mm
- appendicolith
- hyperechoic periappendiceal fat
- loss of echogenic submucosal layer
- increased blood flow of the appendix on color Doppler ultrasound scanning
- periappendiceal collections seen in the absence of a visualized abnormal appendix
Ultrasound images:
http://www.youtube.com/watch?v=d9jKM6x52nk
http://sonocloud.org/watch_video.php?v=MWHM3D7KD25H
http://sonocloud.org/watch_video.php?v=54862AYWGHGA
An overweight 5 year old male presents with acute onset abdominal pain that localizes to the right lower quadrant. What are some causes of a limited or nondiagnostic ultrasound study in children?
Acute appendicitis is a time sensitive diagnosis. Ultrasound is frequently used as the initial diagnostic imaging in children. There are several reasons why the appendix may not be visualized, including retro-cecal location, normal appendix, perforation, and inflammation around the distal tip. An additional clinical predictor associated with poor or inconclusive ultrasound results in appendicitis is increased BMI (body mass index).
A study examining 263 pediatric patients found when BMI > 85th percentile and clinical probability of appendicitis was <50%, 58% of ultrasounds were nondiagnostic. Children with a BMI <85th percentile and clinical probability of appendicitis was <50%, had nondiagonstic scans 42% of the time. These trends were also mimicked in the patients with a higher clinical probability of appendicitis. In the child with a nondiagnostic ultrasound, options include observation and repeat ultrasound scan or CT scan, both of which have associated risks.
2013 AAP AOM Guidelines UPDATE
- Severe unilateral or bilateral AOM (>6mo): give antibiotics. Severe AOM is defined as fever >102.2 (39 C), moderate/severe otalgia, or symptoms >48h.
- Nonsevere unilateral AOM (6-23 months): Advise the parents to consider a period of close observation and follow up (24-72h). If the childs clinical status deteriorates give antibiotics.
- Nonsevere bilateral AOM (6-23 months): give antibiotics.
- Nonsevere unilateral or bilateral AOM (>24 months): Advise the parents to consider a period of close observation and follow up (24-72h). If the childs clinical status deteriorates, give antibiotics.
You have diagnosed an infant or child with pneumonia. How do you decide if they need admission?
The Pediatric Infectious Disease Society and the British Thoracic Society each have guidelines from 2011 to help with this decision.
In children, it is important to consider the maximum doses of local anesthetics when performing a laceration repair or painful procedure like abscess drainage. If there are multiple lacerations, or large lacerations, it may be possible to exceed those doses if one is not careful.
Max doses of common anesthetics
- Lidocaine WITHOUT epinephrine – 4 mg/kg (0.4 mL/kg of 1% lidocaine)
- Lidocaine WITH epinephrine – 7 mg/kg (0.7 mL/kg of 1% lidocaine)
- Bupivicaine WITHOUT epinephrine – 2 mg/kg (0.8 mL/kg of 0.25% bupivicaine)
- Bupivicaine WITH epinephrine – 3 mg/kg (1.2 mL/kg of 0.25% bupivicaine)
For example, in a 20 kg child (an average 5-6 year old), the maximum doses would be:
- Lidocaine 1% - 8 ml
- Lidocaine 1% with epi – 14 ml
- Lidocaine 2% - 4 ml
- Bupivicaine 0.25% - 16 ml
- Bupivicaine 0.25% with epi - 24 ml
Pearls:
- For added safety, some advocate not exceeding 80% of the max dose in children < 8 years of age
- Higher concentration of lidocaine beyond 1% does not improve the time of onset or duration of action and may increases the risk of toxicity
- The addition of epinephrine increases the maximum dose and duration of action, but may be more painful during infiltration
- If the repair requires large amount of local anesthetic, consider doing an regional block
Luu JL, Wendtland CL, Gross MF, et al. Three percent saline administration during pediatric critical care transport. Ped Emerg Care 2011;27(12):1113-1117
Question
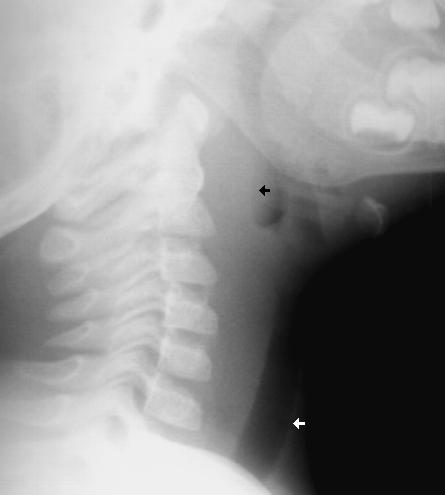
Patient: A 10 year old female is brought to the ED after swallowing 2 beads (see image). Based on the findings, what are your concerns and what is the disposition?
Show Answer
- Nebulized epinephrine: 0.9mg/kg for racemic epi or 0.03 mL/kg of the 2.25% solution (diluted in 3mL) - improves oxygen saturation and respiratory rate, but does not affect admission rates
- Hypertonic saline (3%): decreases hospital length of stay and improves clinical scores, possibly by decreasing airway edema and mucus plugging
- Nasal CPAP: improves ventilation in children with bronchiolitis and hypercapnia
- Heliox: decreases respiratory distress, by reducing gaseous flow resistance and improving alveolar ventilation
Interventions that have shown no benefit and are not recommended:
- Anticholinergics
- oral and/or inhaled corticosteroids
Reference:
Joesph, M. Evidence-Based Assessment and Management of Acute Bronchiolitis in the Emergency Department. Pediatric Emergency Medicine Practice 2011; 8(3)
Parents bring in their child who placed a bead, seed, or other object up her nose. What do you do? Who should you call?
Research suggests that a decades-old home remedy (of sorts) known as the “mother’s kiss” may do the trick for children 1-8 years of age. It’s also much less invasive or frightening than some of the tools and techniques used in emergency departments with a success rate approaching 60%
What Is the “Mother’s Kiss”?
First described in 1965, here’s how the mother’s kiss technique works:
- The parent or caretaker places their mouth over their child’s mouth while holding the unaffected nostril closed with one finger.
- The parent or caretaker blows into the child’s mouth.
- The forceful breath may force the object out (warning: may want to wear protective covering as other things have been known to fly out as well!)
Question
A 1 year old gets sent from their pediatrician’s office for rule out meningitis. They presented with fever for 2 days and neck rigidity. Your LP results are normal. What additional test should you consider?
Show Answer
- The differential of child with stridor <6m:
- Tips for the treatment of croup:
The incidence of pediatric syncope is common with 15%-25% of children and adolescents experiencing at least one episode of syncope before adulthood. Incidence peaks between the ages of 15 and 19 years for both sexes.
Although most causes of pediatric syncope are benign, an appropriate evaluation must be performed to exclude rare life-threatening disorders. In contrast to adults, vasodepressor syncope (also known as vasovagal) is the most frequent cause of pediatric syncope (61%–80%). Cardiac disorders only represent 2% to 6% of pediatric cases but account for 85% of sudden death in children and adolescent athletes. 17% of young athletes with sudden death have a history of syncope.
Key features on history and physical examination for identifying high-risk patients include exercise-related symptoms, a family history of sudden death, a history of cardiac disease, an abnormal cardiac examination, or an abnormal ECG.
The PALS algorithm includes 5 points in management. The first two points are optimally reached within one hour:
1) Recognition of sepsis and vascular access
2) 20ml/kg IVF X 3 within 1 hour or 60ml/kg IVFs within 15 minutes and antibiotic administration
3) Determine if fluid responsive
A recent study at a tertiary care children's hospital retrospectively reviewed 126 patients diagnosed with sepsis. Their findings:
- 37% received 60ml/kg in 60 minutes
- 11% received 60ml/kg in 15 minutes
- 70% received antibiotics in 60 minutes
- In 49% of cases fluids were delivered via IV infusion pump versus manual or pressure bag
- There was a 57% shorter overall hospital stay and 42% shorter ICU stay in patients that received 60ml/kg IVFs within 60 minutes.
- Liver enzymes, coagulation profiles, and lactic acid levels were obtained in "few" patients.
Conclusions:
Suboptimal fluid resuscitation in sepsis is linked to longer hospital stays. Knowledge of PALS guideline and faster administration of fluid were thought to have been causes of poor adherence.
Additionally, parameters measured in sepsis including lactic acid, coagulation studies, and liver enzymes were not routinely collected. The authors concluded this came from a lack of knowledge of their utility in sepsis.
References:
Paul R, et al. "Adherence to PALS Sepsis Guidelines and Hospital Length of Stay." Pediatrics: 2012 Jul 2 [epub adhead of print].